Dermatovenerologist
Khasanova
Alina Rashidovna
8 years of experience
Make an appointment
A common purulent-inflammatory skin disease of an infectious type, the causative agent of which is bacteria of the genus streptococci, is called streptoderma. This infection accounts for up to 40% of dermatological diseases characterized by the presence of lesions associated with the formation of pustules. In about a third of cases, the disease is severe and leads to temporary disability for the patient.
general information
Streptodermia refers to a pathology caused by streptococci. If we talk about the external manifestations of the disease, blisters and purulent rashes that itch appear on the skin.
Streptoderma in children can occur in two different forms: acute and chronic. Acute is characterized by pronounced symptoms, and chronic - by periodicity.
According to the degree of damage, the disease is classified into superficial, deep and intertriginous. Each form has a specific feature.
Symptoms of streptoderma at different stages
Dermatologists identify several common symptoms of the disease in question, which will be present at any stage of the development of the pathology and in any of its forms:
- hyperthermia - an increase in body temperature to significant values (above 38);
- general weakness, accompanied by mild nausea and dizziness - symptoms of intoxication of the body;
- pain in the joints and muscle tissue;
- enlargement and tenderness of the lymph nodes in the area of the immediate source of infection.
If we consider the symptoms of streptoderma at different stages, they will be as follows:
- A slight rash consisting of small bubbles with liquid contents. At the beginning of its development, streptoderma does not bother the child; parents only see a “sore” that they do not even pay attention to. And completely in vain! The fact is that a child can scratch or accidentally damage the source of infection, and streptococci will begin to spread and the pathology will expand. Therefore, it is important to start treatment even at such an early stage of the disease - for example, apply ointment for streptoderma on the face.
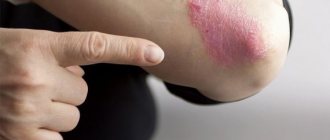
- If no therapeutic measures have been taken, then the source of infection begins to crust over, the blisters increase in size, and tissues not affected by the pathology become inflamed. Streptoderma in this case looks like this: a red-brown crust, from under which yellowish liquid flows out in small quantities, and a red halo is clearly visible around the lesion. If there is a spot of streptoderma on the head, then the hair in this place begins to break and fall out.
- The third stage of development of the disease in question is the widespread spread of streptococcus, the formation of several large spots with a characteristic crust, enlargement and pain when palpating nearby lymph nodes.
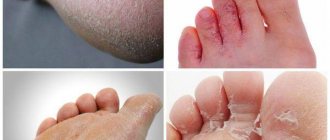
What does dry streptoderma look like? This form of the disease is characterized by slight redness in the area where the infectious agent enters, the presence of a dry crust and the complete absence of liquid contents. If treatment for streptoderma in children was started on time, then after recovery there are no scars or scars left on the skin. In advanced cases, quite serious skin defects can be observed, which cannot but affect the child’s appearance, especially if the pathological focus is located on the face.
Symptoms
If streptoderma occurs, what is the treatment? Before we know the treatment options, let's find out the symptoms. The disease in children occurs in extremely severe forms:
- temperature up to 39C,
- poisoning,
- large lymph nodes.
The texture of the skin may vary depending on the form of the pathology:
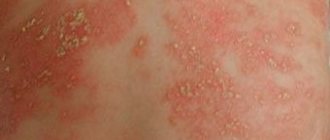
- Superficial. Initially, red spots form on the skin. After a couple of days they turn into blisters with a certain liquid inside. The blisters grow up to two cm in diameter, after which they rupture. Yellow crusts form in this area. After this, the skin in this area heals, and the pathology develops further.
- Dry streptoderma . This form usually occurs in boys. Light and pink spots up to 5 cm in diameter form on the skin. They are found everywhere on the body. After they disappear, scars may remain.
- Streptococcal infection. The pathology extends specifically to the corners of the lips; it is encountered when there is a deficiency of vitamin B. Small cracks form on the skin, causing discomfort. After some time, they form into pustules that become crusty. The child has difficulty consuming food, as it causes pain.
- Felon. In a situation where streptococcus spreads to the area around the nails, panaritium develops. Oddly enough, this disease is more often encountered by children at an early age who bite their nails.
- Streptococcal diaper rash. This form of pathology is typical for breastfed children. Blisters form in the folds of the skin.
Understanding how streptoderma begins to develop in children, treatment which requires timely contact with a dermatologist and the implementation of therapeutic actions, not a minute can be lost. If you constantly put off going to the doctor, the pathology can develop into a chronic form, and it will be almost impossible to achieve a final cure.
streptoderma, treatment
What is streptoderma?
Most often, streptoderma occurs in children. The reason for this is the imperfection of the protective function of the skin in childhood and the inability to fully control the child’s hygiene. Outbreaks of streptoderma are not uncommon in closed children's groups and preschool educational institutions. Our portal contains verified pediatric dermatologists and reviews
about them, which will help you choose a good specialist for your child. Streptoderma in adults is a consequence of parental contact with an infected child.
How is streptoderma transmitted?
When answering the question whether streptoderma is contagious or not, it should be noted that infection occurs in two ways:
- contact (direct contact of damaged skin with the skin of a carrier of the disease);
- contact-household (through household items, dishes, toys, towels).
Thus, the disease is contagious.
Classification of streptoderma
According to the nature of its occurrence, streptoderma in children and adults can be:
- primary (streptococci enter the body through damaged areas of the skin, an acute inflammatory process develops);
- secondary (the disease joins an existing streptococcal infection - eczema, chicken pox, herpes simplex virus, etc.).
Foci of streptoderma may appear:
- on the face;
- in the armpits;
- on the skin of the upper and lower extremities;
- on the hands, feet;
- on the folds behind the ears;
- in the groin area;
- in the intergluteal fold;
- in the inframammary folds.
Localization depends on the form of pathology. Dermatologists distinguish the following forms of streptoderma:
- streptococcal impetigo (foci form on the torso, upper and lower extremities, face);
- streptococcal diaper rash (affects the groin area, behind-the-ear folds, intergluteal fold, axillary area);
- bullous impetigo (inflammation occurs on the hands, feet, legs);
- streptococcal ecthyma (inflamed elements appear on the upper and lower extremities, buttocks);
- streptococcal infection (the disease is localized in the corners of the lips);
- tourniol (flaky lesions are diagnosed in the area of the nasal plates).
The spread of streptoderma throughout the body is facilitated by scratching painful areas of the skin, as well as getting water on the lesions (for example, while bathing, swimming in the pool).
Causes
The causative agent of streptoderma, the photo of which you will find below, is group A streptococcus. However, it is worth noting that infection can only develop in a situation where certain factors are present:
- skin damage,
- lack of following basic hygiene rules,
- weak immune system,
- disruption of the endocrine system,
- dermatological diseases,
- depressive mood
- vitamin deficiency,
- constant washing of the skin, which leads to damage to the protective layer,
- strong influence of different temperature ranges,
- poisoning,
- circulatory disorders.
Reasons for the development of streptoderma
The causes of streptoderma include:
- Hormonal changes in the body. Due to hormonal imbalances, the condition of the skin worsens, so the risk of infection increases.
- Skin injuries. The skin protects against the penetration of pathogenic microorganisms. When abrasions and cuts occur, its protective function is reduced - streptococci can freely enter the body.
- Change in skin pH. Normally, the skin glands secrete substances onto the surface of the epithelium, which, when combined with exfoliated cells, create a protective layer. The latter provides protection against the penetration of infectious agents and promotes rapid restoration of the epithelium in case of cuts and injuries. A sharp change in the acid-base balance of the skin can lead to disruption of the microflora of the skin. As a result, the risk of developing an infectious process will increase.
Patients with allergic reactions manifested by dermatitis (urticaria, atopic dermatitis, seborrheic dermatitis) are also prone to streptoderma.
Therapy
Streptoderma has occurred ? Even in cases where the initial examination was carried out by a pediatrician, only a dermatologist can select therapy. Doctors in this field have an understanding of drugs with a narrow scope of action.
The first step is to limit the child’s diet. The course of treatment also involves avoiding water procedures, which can cause the spread of the disease. Healthy areas of the skin should be washed with a solution of chamomile, and damaged areas should not be touched at all.
The sick person needs to choose the right wardrobe, from which items of clothing made from synthetics and wool must be removed.
Doctors advise popping blisters that form on the skin with a disinfected needle, after which the abscess should be drained twice a day. Healthy areas of the skin are washed with a boron solution.
If crusts appear on the skin, they should be treated with antibacterial gels or ointments.
In more complex situations, many other medications may be prescribed:
- antibiotics for streptoderma of the tetracycline or chloramphenicol series,
- means that prevent the occurrence of an allergic reaction,
- means aimed at improving the body's immune system,
- vitamin preparations,
- antipyretic.
The set of medications must be discussed with the doctor. With the right treatment, the symptoms disappear within a week, but after the severe form is eliminated, scars may remain. This is what streptoderma looks like .
what does streptoderma look like?
Causes of complications and re-infection
The reason for re-infection may be incorrect therapy when, for example, if you have primary criteria for improvement, you decide to stop therapy. The most important thing is to remember that you need to unquestioningly follow the advice and instructions of your doctor.
streptoderma complications
What can streptoderma be confused with?
Pyoderma
With pyoderma, the sebaceous and sweat glands are damaged. The rash appears in certain areas of the skin - parts of the body, scalp.
Herpetic rash
Herpes is characterized by the presence of blisters with constant inflammatory processes. They burst and provoke development.
Thrush or candidiasis
Candidiasis is characterized by erythematous papules or reddened, wet plaques. In the pathology under consideration, the lesion, as a rule, occurs in the mucous membranes or fold areas.
Manifestations of allergies
An allergic rash continues to occur as long as the influence is the causative agent of the allergy.
Types of disease
- Streptococcal impetigo. The most common standard form of the disease. A characteristic rash forms on the face, arms and legs. This form is also the most limited, since the pathogen does not move beyond the upper layer of the skin, which has certain protective mechanisms. The appearance of the integument does not change, only individual blisters with liquid appear on the reddened areas. Initially, the patient will experience itching, after which the blisters become darker, which helps the blister to crust over. The duration of this process reaches one week. However, it is worth remembering that if the rash resolves, bacteria are further transferred to healthy areas of the integument, which has its negative consequences for the sick person.
- Bullous impetigo. The rashes are located on the arms and legs and had a fairly impressive diameter. Once the blisters open, these areas of skin develop ulcers that can spread quickly.
- Streptococcal diaper rash. Most of the patients are young children and overweight people. The location of the rash is under the mammary glands, in the axillary folds, intergluteal or inguinal-femoral folds. If you are overweight, the abdominal area is affected.
- Ringworm common. Appears in the form of bright pink rashes. The place of appearance is the face. The rash may become smaller due to exposure to direct sunlight. Those areas of the skin that are affected will not take on a tan like before.
- Streptococcal infection is characterized by the formation of blisters in the corners of the mouth. After the blisters disappear, a crack appears in their place, which in a matter of minutes becomes covered with a yellow crust. It also happens that children tear off the crust, but it forms again.
- Streptococcal ecthyma is the most complex form of the disease. The disease is accompanied by the appearance of characteristic lesions and scars on the arms and legs. In case of development of ecthyma, as a rule, there is a deterioration in health.
Provoking factors
Provoking factors are streptococcus and skin damage (minimal is sufficient). The pathogen itself is constantly “in the neighborhood” of a person, but as long as the skin is intact, streptococcus does not manifest itself in any way. A small cut, wound, burn with an open blister is enough for the pathogenic microorganism to enter the tissue - this is how infection occurs. The causes of streptoderma on the arms and legs are frequent damage to the skin of these parts of the body.
But infection does not always occur even with a combination of provoking factors! Often a child’s immunity is so strong, and general hygiene is carried out so thoroughly that streptococci simply have no chance of invading. All parents should know whether streptoderma is contagious and how it is transmitted. This will help to carry out timely prevention and avoid problems.
A child can become infected both in kindergarten and when interacting with any person. The most common route of infection is contact, when the skin comes into direct contact with the skin of a sick person (for example, through hugging or kissing). A little less often, streptoderma is transmitted through household means through towels, toys, and common items. Airborne infection can also occur, but it is extremely rare and is considered an exception.
Therapy and drugs
Throughout the spread of the disease, basic hygiene rules should be observed: in the first days, it is forbidden to take baths and wet impetigo, and it is forbidden to comb the affected areas.
Therapy for this disease is aimed at destroying the pathogen and strengthening the protective functions of the immune system. As a complex treatment, antibacterial drugs of the category of cephalosporins, macrolides and penicillins are prescribed. If you have bullous streptoderma, you should stop taking medications. As an immunocorrective treatment, the drugs “Likopida”, “Amiksin” and their analogues are effective. Treatment with drugs for . Restoration of microflora in the intestines occurs with the help of probiotics and prebiotics. Appropriate antihistamines will help get rid of scabies.
Means that increase the body’s resistance to infections in the form of solutions - “Eleutherococcus”, “Echinacea”, “Leuzea”, etc.
Sets of vitamin nutrients should also be taken in accordance with the instructions.
Local treatment includes antiseptic drugs that prevent the spread of putrefactive bacteria. Such medications include various alcohols, brilliant green, as well as their analogues - “Fukartsin”, “Chlorhexidine”, “Miramistin”, “Rivanol” or the cauterizing agent “Resorcinol”.
The use of a huge number of zinc-based pastes, preparations and ointments for streptoderma in children with intense scabies.
Diagnostic methods
To diagnose streptoderma, the doctor does not limit himself to examination and history taking, since external signs of the disease can easily be confused with other skin infections. To obtain accurate data, the patient is prescribed:
- microscopic examination;
- bacterial culture is the most informative research method, which allows not only to detect the causative agent of infection, but also to establish its pathogenicity, and also to check how sensitive it is to antibiotics.
Both tests are prescribed only if the patient has not used antibiotics or other medications. The patient may need to consult an endocrinologist if he has diabetes or is suspected of having this disease.
Preventive measures and prognosis
Due to the high risk of infection, sick children should keep their distance for some time and not contact other people. Quarantine is provided for up to 10 days. For the entire period of therapy, it is necessary to follow the rules of hygiene.
To prevent the development of the disease, it is necessary to disinfect the child’s personal belongings. Sick children should have a proper diet rich in nutrients. To improve the quality of the immune system, certain measures should be taken.
streptoderma treatment
As a rule, streptoderma ICD 10 in children is cured without any problems. Exacerbation of the disease and re-infection are observed mainly in children from disadvantaged families or in children with weak immunity. With timely treatment, symptoms disappear within one week. If you do not attach any importance to this, the disease can develop into a more severe form. In the worst case, the disease can lead to blood poisoning. For streptoderma, treatment with ointments and antibacterial agents is mandatory.
Prevention
To reduce the risk of infection, you should follow the following rules:
- follow the rules of hygiene,
- disinfect damage to the skin,
- strengthen the name system with useful substances,
- do not carry out frequent water procedures, as this may pose a certain danger for the child,
- In case of primary symptoms, you should immediately consult a doctor.
Streptoderma on the face can be treated, but only if you consult a doctor in a timely manner. The earlier therapy was carried out, the easier it is to exclude complications and transition to the chronic stage. You can undergo a full examination in a clinical clinic.