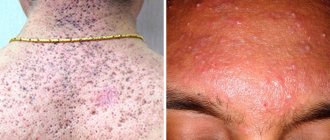
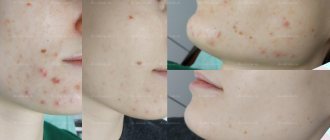
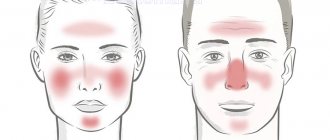
In the first days of a baby's life, a newborn's skin may suddenly become covered with small pimples. These pimples can have different appearances - they can be red, white, they can cover certain areas of the skin, they can appear on the face, or on the whole body. In order not to puzzle over why pimples appeared on the face of a newborn, you need to know about the most common causes of their appearance, and, depending on the cause, select treatment. In general, there are acne that require treatment, and there are those that go away on their own.
What is newborn acne and what causes it?
Between two and five weeks of age, small pimples may appear on your baby's face (usually on the cheeks, nose, eyelids, chin and/or forehead). According to statistics, acne of newborns (or infant acne, neonatal pustulosis) occurs in 30% of babies. Experts do not agree on why acne occurs, but it may be due to one of the following reasons:
- inflammation of the skin caused by fungi of the genus Melassezia, which are part of the normal human microflora and colonize the skin in the first weeks after birth
- overactive sebaceous glands on the baby’s skin, caused by the specific action of maternal hormones (androgens)
Pimples on a newborn's face have nothing in common with acne in teenagers.
Allergic rash
In any case, parents are recommended to consult a doctor to determine the cause of the rash on the baby’s body. If a specialist discovers an allergy, then it is necessary to identify its form and irritant. Typically, the causative agent may be the following:
- the body's reaction to the weather (sun or cold);
- food allergies (in which the allergen product can be consumed by both the baby and the mother, if the former is breastfed);
- heredity (a child is at risk if at least one of his parents is predisposed to allergies);
- cosmetical tools;
- animal hair, dust, pollen;
- vaccination vaccines.
Once the cause of the rash is known, the next important step is to completely eliminate the irritant. It will be easier to do this in cases where the reason lies in external factors that they simply stop using (if they are creams, powders, detergents and other hygiene products). In the case where skin manifestations are the result of consuming certain products, it is important to exclude the product itself. The first signs may appear as early as an hour and a half after eating the allergen. Breastfeeding mothers must follow a diet and avoid spicy, fatty, chocolate, brightly colored fruits and vegetables, and alcohol. In such cases, it will be more difficult to get rid of the rash, since the product must be digested by the intestines, leave the baby’s body, and only after that the spots on the body will begin to disappear. You should know that when the pathogen reaches the baby through mother's milk, the process is delayed and recovery occurs after two weeks. Parents who themselves suffer from allergies should be extremely attentive to what their child is surrounded by and what he eats. Unfortunately, such babies are more prone to skin diseases than others. In this case, the irritant of an adult and an infant can be completely different. At the genetic level, only the predisposition itself is transmitted.
Almost always, allergies as a disease can be prevented. To do this, you will need to fulfill simple requirements:
- maintaining ideal cleanliness in the room, frequent wet cleaning and ventilation;
- introduction of complementary foods no earlier than four months from birth, and in some cases no earlier than six months. At the same time, it is important not to overdo it: if the introduced product is not suitable, then it should be offered to the baby again after one or two weeks;
- Diet compliance by a nursing mother. Drinking large amounts of liquid, broths and soups. Complete exclusion of harmful products;
- You should not self-medicate and try to prevent this or that reaction with the help of medications without appropriate doctor’s recommendations;
- maintaining hygiene and sharing a healthy lifestyle between mother and baby.
Walking in the fresh air, swimming, and hardening will have a positive effect on the health of all family members.
Urticaria and dermatitis are also types of allergic reactions. In the first case, there is a sudden appearance of itchy blisters on any part of the body. Such symptoms can occur from insect bites, from interactions with chemicals, and from eating strong allergens such as cow's milk, nuts, and honey. It is important to consider that prolonged exposure to the pathogen can worsen the baby’s condition, develop into edema and, at the same time, complicate breathing. Therefore, it is necessary to get rid of the presence of the irritant as quickly as possible and consult a doctor. Treatment occurs with the help of antihistamines and sedatives.
Dermatitis , like other types of allergies, is provoked by prolonged exposure to an irritant, increased sensitivity and predisposition to similar manifestations. Symptoms include inflammation of certain areas of the child’s skin (most often the hands, groin, cheeks), possibly burning and discomfort. Dermatitis is divided into several types:
- diaper (long-term interaction of delicate skin with irritants, such as wet diapers, diapers. Here you should change the diaper more often and wash the baby with running warm water before each change.
- Use wet wipes only when necessary, and apply a special protective cream under the diaper.);
- atopic (an outbreak occurs at the immune level, as the body’s response to respiratory and contact irritants. Localized on the cheeks, thighs, arms. Characterized by peeling lesions.);
- allergic (lack of vitamins in the body, consumption of allergic pathogens in food, lack of fresh air, moodiness, hyperactivity).
As in other cases, it is very important to make a diagnosis as quickly as possible and begin treatment in order to prevent transition to a chronic form. All allergenic foods should be excluded from the baby's diet; to reduce itching, the doctor will prescribe the use of a cream or ointment, and also prescribe the necessary medications to eliminate the causes. It is worth understanding that the problem always lies inside, and it is important not only to eliminate external symptoms, but also to completely destroy the original cause of the disease. When an allergy manifests itself against the background of vaccinations for a child, it is important to take into account the child’s predisposition in advance, notify the doctor about this and follow a number of measures prior to vaccination. Such events include the following:
- taking tests;
- use of antihistamines two to three days before vaccination;
- close observation on the day of vaccination and refusal of new products.
Parents need to know that any vaccine contains a potential pathogen. It can be chicken egg white, gelatin and other components that make up the drug. Therefore, after the vaccination has already been done, you need to stay with the child in a medical facility for about half an hour, in order to observe and take measures, if necessary. Most often, doctors do not recommend going for walks on the day of vaccination, especially if the baby is still very small and fragile. It will be necessary to monitor the general condition and possible changes for two weeks.
Rash caused by infections and viruses
Only a specialist can recognize the etiology of the formation of a rash on the baby’s skin and prescribe the need for treatment. But in cases where skin manifestations are accompanied by fever, stool disturbances, vomiting, and difficulty breathing, then most likely the nature of the disease is directly related to infection. Infectious rashes are caused by diseases such as:
- chickenpox (caused by the appearance of blisters containing liquid inside. The areas of spread itch and itch, and the temperature rises to critical levels. Throughout the maturation of the blisters, the child is a carrier of the infection. The affected areas are treated with brilliant green. If all the doctor’s instructions are followed, recovery occurs after 21 days.);
- rubella (this type of infection is characterized by cough, fever, enlarged lymph nodes, intestinal dysfunction, and, as a result, diarrhea and vomiting. The rash is usually not palpable, but appears in the form of redness of the skin. Most often, this disease occurs in children older than two years, but infants can also be infected, especially those who do not have the appropriate vaccination. The disease proceeds without complications and does not require special measures. It is only important to maintain bed rest and reduce the risk of rubella infection for other small family members, since five to seven days, an infected infant can infect unvaccinated children.);
- measles (the main reason for its appearance is the lack of vaccination. Infection occurs by airborne droplets, and symptoms begin to appear no earlier than a week later. As a result, it is not possible to notice the disease in time. Only after a few days do the symptoms of the disease make themselves felt : the temperature rises, a small rash appears first on the inside of the cheeks, head, and then throughout the body.The child’s immunity weakens, so it is necessary to feed it with vitamins during this period, and allow the body to cope with the disease on its own.
It is recommended to help the baby during this period, based on the symptoms that appear: antipyretics, throat sprays, nasal drops, as well as bed rest and frequent fluid intake. Treatment can take place both at home and in a hospital, under the supervision of a doctor, in order to eliminate the possibility of complications). A dermatologist or allergist will help you make the correct diagnosis. To do this, you need to undergo tests and, if necessary, skin scraping. An important role is played by external factors, the nature of the rashes, their localization, as well as the accompanying deterioration of the baby’s condition. In any case, it is necessary to follow all the doctor’s instructions regarding treatment and compliance with certain rules. The duration of allergies is also particularly influenced by the child’s immunity: the stronger it is, the sooner it will cope with the disease. Parents are required not to panic, but to notice the slightest manifestation of symptoms in time and contact a doctor as soon as possible.
How to get rid of acne in newborns
There are no home remedies to get rid of newborn pimples on the face. You need to wait until they disappear on their own. Typically, newborn acne goes away in about three to four months without leaving any traces. Here's how to take care of your baby's delicate skin if he has pimples:
- Wash him every day with warm water and mild baby soap, then pat dry.
- Try to avoid any rubbing of the affected areas of the skin, as this can make the process worse or even lead to infection.
- Do not apply lotions or oils to your baby's face.
- There is no need to follow a diet, since neonatal acne has nothing to do with the mother’s diet
Do pimples need to be treated?
As you can see from this material, the majority of small white pimples in children go away on their own. You just need to wait, usually by the age of two months, children have completely smooth skin without rashes. You should not squeeze pimples, otherwise there is a risk of damage to the upper layers of the skin, infection and scarring later.
If you doubt the causes of acne, be sure to visit a specialist to make a correct diagnosis. To alleviate the child’s condition, the following options can be recommended:
- washing with boiled water three times a day;
- bathing the baby in a weak solution of potassium permanganate;
- bathing a child in a line;
- rubbing the baby’s face with a decoction of string or chamomile;
- competent care for baby's delicate skin.
Under no circumstances use fucorcin, a strong solution of potassium permanganate or brilliant green for treatment, avoid lotions with alcohol, as all these compounds will negatively affect the baby. You should also forget about fatty oils, ointments, powder, calendula tincture, hormonal ointments, lactic acid bacteria, adsorbents (for example, smecta), antibiotics and antihistamines. And, as already mentioned, you should not squeeze out pimples of any kind in children.
When to see a doctor
If you are concerned about your baby's complexion or if you are concerned that the condition is not improving after three to four months, consult your pediatrician. Your doctor may prescribe a special cream to treat acne in a newborn. Do not use over-the-counter creams or any other medications for acne without first consulting your pediatrician as they may harm your baby. Contact your pediatrician if your newborn has any of these symptoms:
- blisters on the skin
- peeling skin
- heat
- uncharacteristic tearfulness
- poor appetite
Preventive measures
Almost all acne in babies is not dangerous. Their occurrence can be easily avoided if you follow a number of measures:
- watch your diet;
- if there is a reaction to the mixture, replace it;
- properly care for your baby and maintain hygiene;
- give the baby air baths;
- wash your baby’s underwear with specially designed powders.
If acne does not go away for a long time and bothers the newborn, doctors usually prescribe medications: Panthenol, Bepanten or Zinc ointment.
Peeling
On the second or third day after birth, the newborn’s skin begins to peel off. Peeling is observed in everyone, but to varying degrees of severity. Most severe if the baby is post-term. The reason is the same restructuring of the body to exist in the air. The skin loses moisture, and the top layer gradually peels off. Physiological peeling does not require treatment and goes away on its own within a few days.
If the peeling is profuse and leads to deep cracks, the skin is lubricated with special moisturizers - emollients. In case of pronounced peeling, it is necessary to exclude congenital skin diseases such as ichthyosis, hyperkeratosis and others.
How to recognize a food allergy and not confuse it with other diseases?
Most often, in order to diagnose a food allergy, a doctor only needs an examination and a detailed interview with the mother. Mom can point out that she herself has a food allergy or point the doctor to a specific food. Sometimes it is difficult to make such a diagnosis right away. Then the doctor may order an examination. First, a general blood test. And then, if necessary, specific allergy tests: examination for immunoglobulins, and at a later age, provocative tests. It is these tests that were chosen as the most informative in the latest clinical recommendations. In addition, your baby may need to consult an allergist, dermatologist or gastroenterologist, depending on the symptoms that are bothering him. And also, additional examination from the gastrointestinal tract.
Diaper rash
A more serious skin reaction to overheating is diaper rash. Occurs in natural folds. It looks like redness, sometimes with weeping and erosion. With a long process, a bacterial or fungal infection may develop, then the surface of the affected skin is moist, bright red, with clear or purulent discharge. Prevention measures are the same as for prickly heat.
The skin in the folds is treated with powders. If normalizing the microclimate and caring for the newborn does not lead to a reduction in diaper rash, you should see a doctor. If complications occur, antibiotic therapy or topical steroid ointments may be needed.
Vascular abnormalities
Congenital anomalies of vascular structure are varied
- A simple nevus is a capillary anomaly. It appears as a pale pink spot or several small spots. The common name “stork bite” or “angel kiss” arose due to its location on the back of the neck and head, on the forehead, bridge of the nose and upper eyelids. The spots fade by the age of two, but can appear when crying or physical activity. No treatment required.
- Port wine stain or flaming nevus. A dark red spot that looks like a hemangioma. It may be one of the manifestations of pathological syndromes. Lasts for a long time. Treatment is not necessary, but can be done if the spot creates a cosmetic defect.
- Venous anomaly - blue-violet painful nodules under the skin. They can also masquerade as a hemangioma. Occur alone or in combination with other anomalies. The danger lies in the possibility of thrombosis of the altered veins. Treatment consists of wearing compression clothing and using aspirin to prevent blood clots. Surgical excision is possible.
- More rare lymphatic, arteriovenous and combined anomalies are found as part of various pathological syndromes.
Seborrheic dermatitis
Appears in infants soon after birth and lasts up to a year. Yellow scales and peeling are most often located on the scalp and behind the ears, but can also be in other folds - axillary, elbow, inguinal. In everyday life they are called “milk crusts”. Because of its similarities to atopic dermatitis, seborrhea is sometimes considered a manifestation of allergies. The causes of this condition are not fully understood, but the relationship with allergies has not been identified.
Seborrhea goes away without treatment, in most cases in the first year of life. Unlike atopic dermatitis, the rash does not cause itching and does not cause discomfort to the child. If for the sake of aesthetics you want to get rid of seborrheic crusts, before bathing the baby’s head is lubricated with oil and then combed out with a soft comb.
In doubtful cases, when seborrhea is located on the body, it makes sense to consult a doctor to clarify the diagnosis.
Infantile hemangioma
Hemangioma is a benign tumor of endothelial cells (endothelium is the inner lining of blood vessels). It may be congenital or appear at 1-2 weeks of life. Superficial hemangiomas are bright red and protrude above the surface of the skin. Deep - blue-purple, sometimes warm to the touch. The element size ranges from a few millimeters to an entire anatomical area (hand, buttock, etc.). In the first 5-6 months, the hemangioma may increase in size and become brighter, then the growth ends and spontaneous regression begins.
Up to 90% of hemangiomas can resolve without treatment.
In this regard, surgical treatment is no longer used routinely. The child is observed by a pediatrician and a surgeon; if hemangiomas are located on the face and neck, in the genital area and near large vessels, conservative treatment is prescribed. The operation is indicated only if it is ineffective.