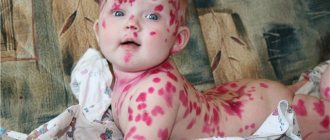
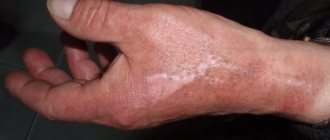
Summer has come - a time for active recreation, summer cottages and vegetable gardens. A time of abrasions and wounds, and therefore a high demand for antiseptics. More than 250 trade names of antiseptics in the form of ointments, solutions, sprays and powders are registered in Russia. Let's figure out which drugs are classified as antiseptics in medicine, how they differ from each other, and which of them can be recommended for every home medicine cabinet.
First of all, we note that the pharmacist independently selects the product only for external use, and the choice of antiseptic for the mucous membranes of the nasopharynx, gastrointestinal tract, respiratory and urinary tract, as well as for the genital organs remains with the doctor. We also remind you that many antiseptics cannot be applied to injured skin. Here are two main points to consider when selling and talking to a client. The mechanism of action of antiseptics may be different, depending on the main active ingredient.
Classification of antiseptics
Halides (halogens and halogen-containing compounds) Chlorine or iodine compounds (antiformin, iodoform, iodinol, Lugol's solution, chloramine B, chlorhexidine).
The bactericidal effect is based on the fact that upon contact with organic substrates, these products release active halogens - chlorine and iodine, which destroy the proteins of microorganisms. Due to their high bactericidal activity, they are widely used both in medical institutions and at home. Oxidizing agents (hydrogen peroxide, potassium permanganate, hydroperite). In contact with tissues, they release active oxygen, which creates unfavorable conditions for the development of anaerobic and putrefactive microbes. They are used to a limited extent due to their moderate bactericidal activity and short shelf life. Acids (salicylic, boric). A shift in pH to the acidic side leads to denaturation of the protoplasmic protein of the bacterial cell. Salicylic acid has a weak antiseptic effect, and boric acid has a large number of side effects associated with toxicity. Currently, antiseptics for treating skin are practically not used as antiseptics. Alkalies (ammonia, sodium tetraborate). Currently, drugs are practically not used as antiseptics due to their low antiseptic activity. Aldehydes (formalin, lysoform). Penetrating inside the microbial cell, they come into contact with the amino groups of proteins, which leads to cell death. The same effect explains the strong irritant effect on human mucous membranes and skin. Currently, they are used more for disinfecting surfaces in medical institutions. Alcohols (ethyl). They dehydrate tissues and irreversibly coagulate the proteins of microorganisms. They are used quite widely and have a pronounced antiseptic effect. In 2006, the WHO declared alcohol-based hand sanitizers to be the gold standard for hand sanitizers. Cationic antiseptics (benzyldimethyl-myristoylamino-propylammonium). The active substance acts on the membranes of microorganisms, leading to their death. It has a very wide spectrum of antimicrobial action, stimulates the immune system, and accelerates the healing process of wounds. Widely used in surgery, obstetrics, gynecology, traumatology, burn therapy, otorhinolaryngology and other fields of medicine. Salts of heavy metals (preparations of mercury, silver, copper, zinc, lead). The antimicrobial effect is associated with blocking the sulfhydryl groups of microbial enzymes. Use is limited due to toxicity. Dyes (methylene blue, brilliant green, fucorcin). They are active against gram-positive bacteria and cocci. Methylene blue has a very weak antiseptic effect and is practically not used. Herbal antibacterial drugs (urzaline, calendula tincture, imanin and others). Weak antiseptic properties. Rarely used. All these substances have different degrees of activity, antimicrobial spectrum and toxicity. To understand how to choose the right antiseptic, you need to be guided by all these characteristics in accordance with the intended purpose: primary wound treatment, treatment of festering wounds, or treatment of damaged mucous membranes or intact skin/mucous membranes. When choosing which antiseptic to treat a particular wound, you must also follow the instructions in order to avoid side effects, as well as determine the dosage required in a particular case. Let's take a closer look at the most popular antiseptics.
Causes of non-healing wounds
The immediate cause of non-healing wounds is insufficient activity of restoration processes in the body, slow tissue regeneration. Moreover, the conditions under which regeneration slows down can be varied.
Among the general factors (i.e., affecting the state of the body as a whole), the following can be identified:
• weakened immunity due to concomitant disease or chronic immunodeficiency state;
• chronic intoxication of the body;
• metabolic disease;
• diabetes; this condition can be considered a severe form of metabolic disorder, namely glucose metabolism. Disturbances in the normal absorption of glucose lead to increased tissue fragility and a slowdown in the regeneration process;
• circulatory disorders - both general and local. The cause may be atherosclerosis, deformation of vascular walls, and diseases of the cardiovascular system. Local circulatory disorders can be caused by prolonged compression of tissues and pinching of small blood vessels (an example of a chronic wound against the background of constant compression of tissues - bedsores);
• hypo- or avitaminosis of vitamins A, C, K and group B, which play an important role in the process of tissue regeneration;
• lack of calcium or zinc in the body;
• exhaustion – nutritional (due to insufficient or malnutrition) or senile;
• presence of cancer.
A specific factor in the appearance of chronic wounds is poor circulation in the legs, most often due to varicose veins. Against the background of impaired blood circulation, trophic ulcers develop on the legs (usually in the shins) - difficult-to-heal tissue defects.
Local factors affecting the wound itself and the area around it include:
• infection;
• the presence of necrotic tissue in the wound (they increase the risk of suppuration and, accordingly, the duration of healing);
• presence of foreign bodies in the wound;
• the presence of bleeding in the wound (also increases the risk of infection);
• repeated damage to an unhealed wound.
The risk of a wound becoming chronic increases if, in addition to the skin, other tissues are damaged - subcutaneous tissue, nerves, muscles, tendons, bones.
Hydrogen peroxide
Only a 3% solution is used to treat wounds (a higher concentration can cause a chemical burn). It is also used as a hemostatic agent. Hydrogen peroxide is an excellent remedy for primary wound treatment (washing), as it has great cleaning ability - dirt particles and damaged cells are mechanically removed with the resulting foam. You can treat wounds both on the surface of the skin and on the mucous membranes. Hydrogen peroxide is generally not used on healing wounds, as it prolongs the period of complete healing. It is also not used for deep wounds and is not injected into body cavities. When stored in light, it loses its active properties. Open packaging is stored for about a month, closed - 2 years.
How to apply a tourniquet correctly
Applying a tourniquet is a last resort measure to stop bleeding, which can only be used for blood loss from the brachial or femoral artery. It is applied at a distance of 5 centimeters from the wound towards the heart. It is prohibited to apply a tourniquet to the lower third of the thigh or middle third of the shoulder. The duration of use of the tourniquet is no more than 45 minutes in summer and 30 minutes in winter.
A gauze or cloth bandage must be applied to the body under the tourniquet. Next, the limb with a tourniquet must be thermally insulated and immobilized until doctors arrive.
Iodine/povidone-iodine
Used in an alcohol solution (the so-called “tincture of iodine”) or in Lugol’s solution. Only the edges of the wound are treated with iodine so as not to cause soft tissue burns. The great advantage of iodine is its wide spectrum of antimicrobial activity: it kills all major pathogens and, with prolonged exposure, even spores - the most resistant forms of microorganisms. The use of large amounts of iodine is contraindicated in cases of hypersensitivity to it, hyperfunction of the thyroid gland, thyroid formations, dermatitis, and kidney diseases. Application to mucous membranes is not advisable, especially in children.
Examples of the most common injuries
The skin here is very soft and sensitive, so it is most susceptible to bruises and abrasions. First of all, you need to wash the wound with plenty of clean running water. If necessary, apply ice or a cold object - this will help quickly stop the bleeding. Next, apply a clean cotton swab or gauze bandage to the wound. For several days you need to wash the wound with chamomile decoction, you can use furatsilin. If the wound is serious enough, then it is necessary to show the child to a surgeon.
Another common childhood injury is head trauma. Such injuries are divided into open and closed. If the wound is open, then, as a rule, the soft tissues of the head are damaged and the wound bleeds. In this case, you should immediately call an ambulance. If the injury is closed, it may be accompanied by swelling, swelling, and sometimes scratches and abrasions. In this case, the mother should apply a cold object to the child’s head - ice, a cold compress. It is worth paying attention if the child becomes sleepy after a bruise and shows signs of nausea and dizziness. Such symptoms accompany concussions of varying severity. In this case, you should immediately contact a specialized institution.
A common childhood injury is nasal injury. Children's cartilage is still quite soft, so it does not break. And yet it is quite possible to get a slight displacement or abrasion. Having assessed the severity of the injury, the mother should decide whether to show the child to an otolaryngologist in order to avoid future problems with the nasal septum.
Children often cut their eyebrows. In this case, such an injury is accompanied by severe bleeding. In this case, you should also stop the bleeding by applying a cold compress or ice. Next, treat the wound with brilliant green and apply a bactericidal patch.
Children can often lose a tooth in children's games. If a child has lost a baby tooth, rinse the mouth with plenty of water. If a molar tooth has fallen out, you need to find it, wash the tooth with cold water and contact the dentist for tooth reimplantation.
The cheeks can also be frequently injured in children. With such an injury, the degree of injury should be assessed; if the soft tissues inside the cheeks are damaged, they should be treated with chamomile decoctions or disinfectant solutions. Parents cannot always protect their baby from injury. But knowing the first rules of necessary assistance in case of injury, you can significantly alleviate the baby’s suffering, and for any minor bruises or wounds, you can always use Lekker products.
When we were children, our parents usually treated any bruise or abrasion with iodine or brilliant green.
These are two completely different in properties and composition of the means, the result of the use of which has always had the maximum impact on the injury. Times are changing and now you can use both iodine and brilliant green in a convenient and economical form from the Lekker company.
Chlorhexidine bigluconate
Belongs to the group of halogens. Typically used in concentrations of 0.5–4.0%. At lower concentrations, the bactericidal activity of chlorhexidine decreases, therefore, as an antiseptic in this case, it is used only in an alcohol solution. Chlorhexidine has bacteriostatic, fungicidal, antiviral properties. However, 1% chlorhexidine against fungi and mycobacteria tuberculosis has a weaker effect compared to povidone-iodine. The drug can be used for the initial treatment of injured skin areas, as well as to accelerate the healing of purulent wounds and for the treatment of damaged mucous membranes. In most cases it is well tolerated. There are no age restrictions for use - a good antiseptic option for children. It is not recommended to use together with iodine preparations (often skin irritation).
How to speed up healing
The speed of wound healing varies. It depends on the nature of the injury and the individual characteristics of the patient, such as age, nutrition, and medications taken.
To speed up healing, it is necessary to provide optimal conditions for tissue regeneration at each stage. This role is fulfilled by therapeutic dressings designed for each stage of healing.
The method of hydrotherapy has a positive effect. Its essence consists in the sequential use of two dressings HydroClean and HydroTac. Using the first, the wound is cleaned, and then a second is applied, creating optimal conditions for granulation and epithelization.
Benzyldimethylmyristoylaminopropylammonium
It is used as a solution for washing wounds or as an ointment for application to purulent wounds. It is active against viruses, bacteria, fungi, and protozoa, but has virtually no effect on human cell membranes, unlike chlorhexidine. It has an antiseptic, immunostimulating and wound-healing effect. The immunostimulating effect is associated with the ability of the drug to increase the activity of phagocytes and macrophages. The positive effect on wound healing is explained by the fact that the active substance absorbs pus and fluid released during inflammation of wounds. At the same time, the product does not irritate healthy tissues and does not interfere with the growth of new tissues. The main indication for use is the prevention of suppuration and treatment of purulent wounds. Can be applied to mucous membranes. Can be used to treat wounds for children over 3 years of age.
Types of injuries differentiated by other criteria
If we consider tissue damage according to the degree of penetration, we can distinguish the following types of wounds:
- superficial;
- tangents;
- deep;
- end-to-end;
- blind.
Superficial wounds affect only the skin or mucous membranes, without disturbing the integrity of the soft tissues underneath - for example, abrasions or light scratches.
Tangential wounds pass by vital organs or bones without touching them, but can be quite deep and are accompanied by bleeding.
Deep wounds are injuries in which the integrity of bones, organs and internal tissues of the body is disrupted.
Penetrating wounds always have two holes - the place of entry and exit of a wounding object, for example, a bullet or a dagger.
As for blind wounds, they always require the intervention of doctors, since in this case part of the object that struck the person remains in the body, and it must be removed from the tissues or organs.
Brilliant green solution
Everyone's favorite "green". Available in the form of alcohol solutions and pencils. It has a moderate antiseptic effect and is effective against gram-positive bacteria. Only the edges of the wounds are treated with the solution, without going into damaged tissue. Has a drying effect. It is used until the period when fresh granulation tissue begins to appear in the wound, since long-term use prevents adequate healing of the wound edges. Can be used as a children's antiseptic.
Treatment of non-healing wounds taking into account their cause
When starting to treat injuries of this kind, it is necessary to understand the cause of their occurrence. Further actions will depend on this.
1. First of all, it is necessary to examine the wound for foreign bodies, necrotic tissue, and bleeding and, if necessary, clean it. Please note that it is strongly recommended not to remove foreign bodies yourself! Such attempts may cause additional tissue damage and increase the risk of infection. You need to seek help from a doctor.
2. If local blood circulation is impaired, it is necessary to eliminate the source of pressure on the tissue (change the position of the patient’s body with bedsores, wear looser clothes/shoes for “diabetic” wounds).
3. When treating trophic ulcers on the legs, it is necessary to use compression stockings or bandages - they will help “support” the blood vessels and normalize blood circulation, as well as “pull” the edges of the wound towards each other for faster healing.
4. In case of exhaustion and vitamin deficiencies, it is necessary to provide a normal balanced diet in order to provide the body with the necessary substances for tissue regeneration and the production of collagen - a substance that is actively involved in the early stages of the healing process and helps tighten the edges of the wound.
5.If you have diabetes (of any type), you need to monitor your blood glucose levels.
After creating optimal conditions for wound healing, you can begin to treat and treat it.
Fukortsin
Coloring antiseptic. A combination of fuchsin, boric acid, phenol, acetone, resorcinol and ethanol. Indications for the use of fucorcin are fungal and pustular skin diseases, abrasions, cracks, etc. Apply to the edges of wounds. Has less drying effect than brilliant green and iodine. It is used much less frequently in wound treatment. It is undesirable to use in children due to the boric acid and phenol contained in it, which have a large number of side effects. When applied to the skin, boric acid easily penetrates the blood (especially in children) and enters the internal organs and tissues, accumulating there. Therefore, long-term use can cause intoxication. This property forced us to sharply limit the use of boric acid, especially in childhood. Phenol also has the ability to easily penetrate the skin and lead to intoxication of internal organs.
Types of abrasions and wounds
We encounter cuts and all kinds of abrasions in everyday life. An abrasion is damage caused by mechanical friction against a rough and rough surface, often hard. This may be the result of a fall on asphalt or gravel.
The abrasion may be superficial, in which case only the epidermis is affected. The area turns red and swells a little. If the injury is deeper, then not only the epidermis is damaged, but also the capillaries, which leads to pinpoint bleeding, droplets of blood are released, but most importantly, the person experiences severe pain.
A cut is a shallow cut wound. With such an injury, either only the skin is damaged, or the layer of fatty tissue is affected. In such cases, bleeding occurs, the intensity of which will be determined by the depth of the cut and the number of damaged vessels.
Wounds can be superficial or deep, and large vessels can even be damaged. In this case, severe bleeding occurs. Wounds may be accompanied by bruises and bruises. In addition, dirt, various objects, earth, etc. often get into the wound.
Octenidine (octenidine dihydrochloride)
A cationic surfactant with antimicrobial activity against gram-positive and gram-negative bacteria, viruses, as well as against yeast-like fungi and dermatophytes (fungi that feed on keratin and cause dermatomycosis). Similar in action to quaternary ammonium compounds (QAC). The damaged surface is completely processed. Can be used on mucous membranes. The antiseptic has no age restrictions and is used for children. Currently, it is the drug of choice in Europe as an antiseptic due to its wide spectrum of action and maximum speed of achieving effect.
Table 1. Comparative characteristics of the main antiseptic agents
| Antiseptic | For leather processing | For treating wounds | For mucous membranes | Applicability for children |
| Ethanol | + | _ | _ | — |
| Hydrogen peroxide | + | + | + | + |
| Iodine | + | _ | — / + | — / + |
| Chlorhexidine | + | + | + | + |
| Potassium permanganate | + | _ | _ | + |
| Diamond green | + | _ | _ | + |
| Fukortsin | + | _ | _ | _ |
| Benzyldimethylmyristoylaminopropylammonium | + | + | + | + |
| Octenidine | + | + | + | + |
Principles (stages) of treatment
Actions when treating a wound depend not only on the conditions and causes of its appearance, but also on the stage at which the wound process has stopped in it.
The first stage of the wound process is acute. During it, vascular changes occur caused by a reaction to damage, and the process of blood clotting is actively underway. If the wound is infected, pus is formed and toxic substances are simultaneously absorbed into the tissue.
At this stage, it is necessary, first of all, to clean the wound - remove dead tissue from it, remove foreign bodies (with the help of a doctor), drain it - remove pus and exudate from the wound. It is also necessary to prevent infection from entering the wound. It is best to wash the affected area with saline solution, as caustic disinfectant liquids can harm surrounding healthy tissue.
The second stage of the wound process is granulation. At this stage, a thin layer of connective tissue begins to form on top of the wound. The edges of the wound begin to tighten, and it closes itself. The thinnest capillaries are formed in the connective tissue layer, providing nutrition to regenerating tissues. Often chronic wounds stop at this phase, and the healing process does not proceed further; This is most often what happens with trophic ulcers.
At the granulation stage, it is important, firstly, to protect the newly formed tissue from mechanical damage, secondly, to stimulate further regeneration, and thirdly, to prevent the development of the inflammatory process - despite the fact that the wound is closed, the risk of infection and inflammation remains. To stimulate tissue regeneration, methyluracil ointment is used (you can use a ready-made Voskopran dressing with methyluracil ointment); to protect the surface of the wound, atraumatic dressings should be used that do not stick to the wound surface and do not injure it.
We should not forget about maintaining a maintenance diet and sleep schedule - this will help speed up the healing process.
In every first aid kit
So, what products can a pharmacy worker recommend to a buyer for a home first aid kit? First of all, these are benzyldimethyl-myristoylamino-propylammonium and octenidine, as the most universal and safe agents. These drugs are the drugs of choice and should be recommended first. Chlorhexidine is also quite versatile, which is used on intact tissues and for treating wounds, including mucous membranes. As for solutions of brilliant green and iodine, it is necessary to inform the buyer that these antiseptics are only suitable for treating wound edges and should not be used on mucous membranes. Thus, among the entire list of antiseptics presented on the pharmaceutical market, a fairly small number of drugs have universal application possibilities.
Sources
- Kharkevich D. A. Pharmacology. M. Geotar Medicine. 2010.
- Blatun L. A. Miramistin in a comprehensive program to combat hospital infections in a surgical hospital // Miramistin: application in surgery, traumatology and combustiology: collection of works / ed. Yu. S. Krivosheina. M., 2006.
- Carolin Fromm-Dornieden, Gorovtsov A. V., Nadine Schӓfer, Ewa K. Stuermer. Comparison of the rate of growth suppression of E. COLI, STAPHYLOCOCCUSAUREUS and PSEUDOMONASAERUGINOSA by modern antiseptics for the purpose of their use for infected wounds // Fundamental Research. — 2013. — No. 10–2.
The wound must be clean
In a purulent wound there may be scabs, necrosis, crusts, fibrin (this is yellow dense tissue on the wound), then such a wound must be cleaned. Cleansing can be achieved using Neofix FibroGel AG, IntraSite Gel and IntraSite Conformable hydrogels. The main purpose of these gels is to moisten necrosis and crusts, loosen them, which facilitates easier removal of necrosis during subsequent dressings. Hydrogels are applied directly to the wound in sufficient quantities so that the wound is completely covered with hydrogel; the hydrogel layer must be at least 5 mm. Next, the wound must be covered with a film dressing, for example OpSite Flexigrid, or one of the postoperative dressings OpSite Post-Op, PRIMAPORE, NEOFIX Post. On top of the gels, you can use absorbent dressings Allevyn Adhesive or Allevyn Sacrum, which are preferable and more convenient to use in the treatment of bedsores, since these dressings have a sticky edge and a soft spongy pad. After a maximum of three days, it is necessary to bandage, remove the hydrogel from the surface of the wound, and along with it the softened necrosis and crusts. If there are areas of necrosis or stupa remaining in the wound, then it is necessary to use the hydrogel more than once until the wound is completely cleansed. The advantage of using the antimicrobial hydrogel Neofix FibroGel AG for these purposes is that this hydrogel contains silver. This antimicrobial component fights any infectious agents in the wound. As a result of the use of hydrogels, the wound is cleaned. Dressings must be carried out at least once every 1-3 days, and preferably under the supervision of the attending physician.
The problem of wound infection has become extremely relevant in recent years. The number of infectious complications from surgical wounds has sharply increased, resulting in severe sepsis caused by gram-negative microorganisms, as well as microorganisms resistant to almost all modern antimicrobial drugs.
Among all surgical patients, wound infection occurs in 35-45%. The number of postoperative purulent-septic infections in 1998 increased to 39% [14].
Simultaneously with the increase in bacterial infections, the frequency of candida and aspergillus fungi increases, most often due to the widespread, irrational use of antibacterial, corticosteroid, cytostatic drugs, as well as the lack of the concept of simultaneous prescribing of antifungal drugs with antibiotics for prophylactic purposes. The problem of intrahospital spread of both aerobic and anaerobic (clostridial and non-clostridial) infections remains relevant.
The reasons for the increase in the frequency and severity of purulent infections in surgery are varied and include the following factors:
— increasing the volume of surgical interventions, especially in high-risk patients;
- widespread use of instrumental examination and treatment methods accompanied by infection of the patient (intravascular and urinary catheters, endoscopic and tracheostomy tubes, endoscopic manipulations, etc.);
- traditional long-term regimens of prescribing certain groups of antibiotics for therapeutic and prophylactic purposes without regular monitoring of the dynamics of resistance of hospital strains to these drugs.
Depending on the pathogens that have invaded and the changes that occur in the wound, nonspecific (purulent, anaerobic, putrefactive) and specific (wound diphtheria, wound scarlet fever) wound infections are distinguished. In addition, a number of infectious diseases that do not have the nature of a wound infection enter the body through a wound, i.e. not accompanied by noticeable disturbances in the wound process. Some of these common infectious diseases are necessarily associated with the invasion of a pathogen into a wound (tetanus, rabies, rat bite disease); in others, the wound is only one of the possible routes of penetration of microbes (syphilis, anthrax). In practice, it is advisable to focus on the distribution of patients with wound infection into groups, taking into account the etiological and clinicopathological features:
- acute purulent diseases of the skin and soft tissues (abscessing boil, carbuncle, hidradenitis, mastitis, etc.);
— purulent post-traumatic wounds of soft tissues (with or without bone damage, with long-term soft tissue crush syndrome);
— postoperative purulent wounds of soft tissues;
— chronic purulent diseases of soft tissues (trophic ulcers of various origins, bedsores, etc.);
- hematogenous, postoperative or post-traumatic osteomyelitis;
- surgical sepsis.
Regardless of the origin of the wound process, the species composition of the wound microflora, the main methods of treatment are surgical and active complex effects on the purulent process, aimed at eliminating the tissue defect, suppressing the growth of microflora vegetating in the wound or preventing suppuration.
Along with timely surgical intervention on a purulent focus, the outcome of the disease is largely determined by adequate systemic and local antibacterial therapy, strictly focused on the data of bacteriological studies.
Only local drug treatment that is carried out strictly in accordance with the pathogenesis of the wound process can be considered reasonable, i.e. taking into account the phase of its flow [15].
Etiology of wound infections
In recent years, under the influence of various factors, primarily the powerful selective action of antibiotics, significant changes have occurred in the etiology of wound infections. Currently, the leading pathogens are:
— staphylococci (S. aureus, S. epidermidis);
- £, B, Y-hemolytic and non-hemolytic streptococci;
— representatives of the family Enterobacteriaceae (E. coli, Citrobacters
spp.,
Klebsiella
spp.,
Enterobacter
spp.,
Serratia
spp.,
Proteus
spp.,
Providencia
spp.);
- non-fermenting gram-negative bacteria (Pseudomonas
spp.,
Acinetobacter
spp.,
Moraxella
spp.,
Flavobacterium, Achromobacter).
The dependence of the species composition of wounds on their origin is clearly visible. So, for example, if in a group with acute purulent diseases staphylococcus in monoculture is detected in 69.5% of cases, then in patients with post-traumatic purulent wounds, chronic purulent diseases of the skin and soft tissues, as well as in patients with purulent wounds and developed sepsis, they are detected immediately several pathogenic microorganisms in 31.5, 48.8, 55.6% of cases, respectively. The rest are representatives of the family Enterobacteriaceae
in monoculture.
In recent years, fungi have begun to emerge from wounds much more often (9.9%), which is apparently due to insufficient attention to this problem and the lack of reliable prevention of fungal invasion (Table 1).
Obligate non-spore-forming anaerobic microorganisms, among which Bacteroides
spp.,
Fusobacterium, Peptococcus
spp.,
Peptostreptococcus
spp.,
F. nucleatum, P. melaninogenicus.
The proportion of pure non-clostridial and mixed aerobic-anaerobic microflora also depends on the location and origin of the purulent wound.
Currently, it is possible to significantly reduce the duration of systemic antibacterial therapy through the active introduction into practice of treating wounds under dressings with modern drugs focused not only on the phase of the wound process, but also on the species composition of wound microorganisms.
This tactic, with timely adequate surgical intervention and treatment with correctly selected drugs for local therapy, allows you to localize the purulent process and avoid generalization of the infectious process.
The use of modern drugs for local treatment of wounds at all stages of complex treatment makes it possible to reduce the time of systemic antimicrobial therapy, avoid the development of side effects, significantly reduce the cost of expensive antibacterial drugs, and avoid the formation of microflora resistance to the systemic antibiotics used.
Currently, several groups of drugs have been developed for local treatment of wounds in phases I and II of the wound process (Table 2).
The main groups of drugs are antiseptics, polyethylene glycol (PEG)-based ointments, modern biologically active dressings, enzyme preparations, and new antiseptics.
Antiseptics
When choosing antiseptics used for both preventive and therapeutic purposes, preference is given to drugs with a universal, broad spectrum of action, active against mixed microflora, and having a microbicidal or microbostatic effect.
Iodophors
In the practice of wound treatment, new complex compounds of iodine with polyvinylpyrrolidone (povidone-iodine, betadine, iodopirone, iodovidone, etc.), which have microbicidal and microbostatic effects, are widely used.
Drugs in this group suppress:
- gram-positive bacteria, including enterococci and mycobacteria;
- gram-negative bacteria, including pseudomonas, acinetobacter, Klebsiella, Proteus;
— bacterial spores, fungi, viruses, including hepatitis B and C viruses, entero- and adenoviruses, as well as anaerobic, spore-forming and asporogenic bacteria.
All pathogens of wound infections do not have either natural or acquired resistance to iodophors.
The activity of the complex with polyvinylpyrrolidone is not affected by the presence of blood, purulent discharge or necrotic tissue [4].
The most widely used in the practice of treating purulent-inflammatory processes are two dosage forms of complex compounds of iodine with polyvinylpyrrolidone - solution and ointment.
Ointments (1% iodopyrone ointment, povidone-iodine ointment) are used to treat purulent wounds with heavy exudation. Solutions (iodopirone, povidone-iodine) are used as antiseptics for prophylactic purposes for treating the surgical field, skin during punctures, closing surgical sutures, as well as for the treatment of wounds, trophic ulcers, bedsores, and diabetic foot syndrome in the absence of a large amount of wound separated.
Dioxidine
Dioxidin is one of two drugs derived from quinoxyline di-N-oxide, developed as a result of fundamental exploratory research in the period from 1960 to 1980 at the All-Union Scientific Research Chemical-Pharmaceutical Institute (currently the Center for the Chemistry of Medicines - TsKhLS VNIHFI , Moscow).
A number of drugs of this class of substances with high antimicrobial activity and a wide antimicrobial spectrum (quindoxine, mequidox, carbadox, temadox, olaquindox) have been developed abroad.
The drug is intended for the treatment of patients with wound infections caused by multidrug-resistant flora, Pseudomonas aeruginosa and non-clostridial anaerobic pathogens. This drug is most active against anaerobic bacteria (Clostridium
spp.,
Bacteroides
spp.,
P. melaninogenicus, Peptococcus
spp.,
Peptostreptococcus
spp., as well as aerobic gram-negative bacteria -
Ps.
aeruginosa, E. coli, Proteus spp.,
Klebsiella
spp.,
Serratia
spp.) [1-3].
It should be noted that strains of Pseudomonas aeruginosa, as well as gram-positive bacteria (staphylococci, streptococci), are more resistant to the drug. That is why, if the clinical situation allows, a 1% dioxidine solution without dilution is used for local treatment.
In the 70-90s, a solution of dioxidine in monotherapy and combination with other antibacterial drugs was considered as the drug of choice for the treatment of patients with sepsis, diffuse and local peritonitis, for the prevention and treatment of purulent-inflammatory processes in the liver and biliary tract, lungs, stomach, kidney allotransplantation, cardiac vascular prosthetics and coronary artery bypass grafting, under conditions of artificial circulation [11-13].
Currently, in Russian clinics for more than 25 years, various dosage forms of dioxidine have been used to treat various forms of purulent infection:
a) for local treatment
— 5% ointment, “Dioksikol” ointment containing 1% dioxidine, dioxidine aerosol (“Dioxisol”), polymer compositions with dioxidine (“Diovin”, “Diotevin”, Anilodiotevin”, “Colladiasob”, “Digispon A”, suture material ;
b) for introduction into cavities, for ultrasonic inhalations
— 1% aqueous solution in ampoules;
c) for intravenous administration
— 0.5% aqueous solution in ampoules.
Intravenous administration of dioxidine is carried out for health reasons. When justifying and determining the indications for the intravenous administration of dioxidine from the “benefit-risk” perspective, it should be taken into account that over the past 15-20 years, highly effective antibacterial agents have been created that have advantages over dioxidine in terms of toxicological properties. Therefore, dioxidin is prescribed intravenously only if other chemotherapeutic agents are ineffective or intolerable, strictly observing the recommended doses for the drug and the duration of each infusion.
Dioxidin is well compatible with other antimicrobial drugs. The clinical capabilities of dioxidin are expanded due to its ability to penetrate the blood-brain barrier, which makes it possible to use it in the treatment of patients with meningitis, brain abscesses and purulent cranial wounds.
Miramistin
The domestic antiseptic Miramistin belongs to quaternary ammonium compounds (cationic surfactants). Preclinical and clinical studies have shown that Miramistin has a pronounced antimicrobial effect against gram-positive and gram-negative, aerobic and anaerobic, spore-forming and asporogenic bacteria in the form of monocultures and microbial associations, including antibiotic-resistant hospital strains. The drug is most effective against hospital strains of staphylococcus and streptococcus. The drug has a detrimental effect on fungi, viruses, and protozoa.
Miramistin has been introduced into clinical practice since the early 90s of the last century. Currently, the drug is widely used in the complex treatment of purulent wounds and accompanying inflammatory complications in the bronchopulmonary system in the form of ultrasonic inhalations and the genitourinary system in the form of bladder instillations [5].
Lavasept
An antiseptic drug, the main active ingredient of which is polyhexanide, considered by experts as the drug of choice for the treatment of contaminated and infected wounds [16]. Polyhexanide belongs to the group of positively charged (cationic) polymers and contains surfactants, which reduce surface tension, which ensures easier removal of microbial biofilms.
Lavasept has a broad-spectrum bactericidal effect, is active against gram-positive and gram-negative bacteria (including Pseudomonas aeruginosa
), fungi, and MRSA.
Prontosan
A particular danger for the patient is a “dormant” infection, the aggressiveness of which is determined by the variability of the microflora, the reactivity of the body, the loss of activity of traditional systemic antibiotics and drugs for local medicinal treatment of wounds. This threat persists to a particular extent if the patient has foreign bodies, implanted devices, in patients with long-term non-healing wounds, trophic ulcers, diabetic foot syndrome, with post-traumatic and postoperative osteomyelitis, chronic post-traumatic and postoperative wounds.
It has been established that microorganisms and fungi, when they remain in a wound for a long time, thanks to the polymers they secrete, form a thin layer - a biofilm. Biofilm formed by bacteria and fungi provides reliable protection for pathogens from ultraviolet radiation, antibiotics, phagocytosis and other factors of the body’s immune system. Microbes in the biofilm can withstand concentrations of antibiotics 100-1000 times more than suppressive planktonic cells. Therapeutic effects on biofilms can be aimed at the mechanisms of initial adhesion of bacteria to the surface, blocking synthesis or destruction of the polymer matrix.
Currently, the attention of researchers on this problem is drawn to the possibility of using various medications that destroy the biofilm formed by bacteria and fungi. One of these drugs is prontosan, which contains polyhexanide, a polymerized biguanide derivative that acts as a local cationic antiseptic. The antimicrobial effect of polyhexanide is due to nonspecific affinity for the cell membranes of the microorganism, which contains a large amount of acidic phospholipids. Polyhexanide acts on bacterial cell membranes and increases their permeability.
Two dosage forms of Prontosan have been introduced into practice - 0.1%, 0.2% solution and gel, which contains 0.1% polyhexanide, 0.1% undecylenic amidopropyl betaine (surfactant), glycerol (humectant), hydroxyethylcellulose ( gelling agent), water.
PEG-based sorbents and ointments
It should be remembered that with abundant purulent exudation, the use of antiseptic solutions for local treatment of wounds in the form of gauze tampons is considered a flawed method, since tampons placed in the wound dry out quickly and do not have the long-term osmotic activity necessary to remove pus. In extreme cases, the wound can be filled with a combined tampon - a silicone tube is placed in the center of the gauze tampon, through which 10-20 ml of antiseptic is injected into the wound with a syringe 3-6 times a day.
For the treatment of superficial infected, purulent and purulent-necrotic wounds of various etiologies in the inflammatory phase, biologically active draining sorbents (anilovine, diovin, anilodiovin, diotevin, anilodyotevin, collasorb, colladiasorb), the main component of which is helevin, are successfully used. Dioxidin is used as an antimicrobial drug. The proteolytic effect of sorbents is due to the introduction of proteolytic enzymes into their composition (terrylitin, collagenase from hydrobionts). The analgesic effect is achieved due to the presence of a local anesthetic, anilocaine, in the composition [11].
Targeted use of biologically active dressings with a differentiated effect on the wound process, taking into account its phase and characteristics of the course, providing for sorption-application therapy in phase I of the wound process using biologically active sorbents or gel dressings with antimicrobial, analgesic and proteolytic effects, followed by wound treatment in phases II and III of the wound process with biologically active stimulating coatings with a specific effect on the processes of regeneration and epithelization.
In recent years, it has become possible to more successfully treat wounds using a new combination drug Baneocin, containing two highly active bactericidal components - bacitracin (a polypeptide antibiotic that inhibits the synthesis of bacterial cell walls) and neomycin (an aminoglycoside that inhibits protein synthesis), between which there is synergy. The results of numerous studies indicate the high activity of baneocin against gram-negative, gram-positive flora, aerobes and anaerobes. The components of the drug exhibit synergism against highly resistant hospital strains of Ps. aeruginosa, E. coli, S. aureus.
Baneocin is characterized by the ability to create high bactericidal concentrations in a purulent focus and not have a systemic effect. Numerous studies have shown that when treating wounds under bandages with Baneocin, complete eradication of pathogenic pathogens and reliable prevention of reinfection of the wound surface by hospital microorganisms is achieved in a short time without the traditional systemic antimicrobial therapy in such cases, prescribed for both therapeutic and prophylactic purposes.
The drug Baneocin is available in two dosage forms, focused on the phases of the wound process. For example, for the treatment of purulent wounds in the first phase of the wound process, Baneocin powder is used, which actively absorbs wound discharge within 5 hours.
For the treatment of wounds in the II phase of the wound process, Baneocin ointment is used, which exhibits a local bactericidal effect necessary to prevent reinfection of granulating wounds with hospital strains. The resulting thin film of the drug protects the thin layer of young epithelium from damaging factors.
The positive properties of two dosage forms of Baneocin - powder and ointment - are successfully implemented both at the outpatient and inpatient stages of complex treatment of patients of different groups:
- with focal skin infections (hidradenitis suppurativa, paronychia, boil, carbuncle);
- with burns, frostbite;
- with trophic ulcers;
- for the prevention of suppuration of household, sports and industrial wounds, abrasions (violations of the integrity of the skin);
— to prevent the development of an infectious process in the area of donor wounds when collecting skin grafts in traumatology, surgery, and cosmetology.
Painless and non-traumatic application, deep penetration into tissue, and good tolerability of Baneocin make it possible to successfully treat patients with trophic ulcers even in cases of aggravated allergic history (intolerance to traditional local drugs) or the identification of highly resistant strains of Ps. aeruginosa
[6].
For the treatment of extensive and deep wounds with a purulent process in the first phase
over the past 25-30 years, PEG-based ointments have been successfully used (levosin, levomekol, 5% dioxidine ointment, dioxykol, 1% iodopyrone ointment, 1% povidone-iodine ointment, 0.5% miramistin ointment, iodometricylene, nitacid, streptonitol , 10% mafenide acetate ointment, streptolaven, stallanin-PEG 3%, oflomelide, etc.). The listed drugs have different osmotic activity for the differentiated treatment of wounds in the first phase of the wound process with copious or moderate amounts of wound discharge (boils, carbuncles, hidradenitis, mastitis, abscesses, phlegmons, suppurating lipomas, atheromas, purulent postoperative and post-traumatic purulent wounds, venous trophic ulcers , “diabetic foot” with a local purulent-necrotic process, etc.
These drugs have a fairly wide spectrum of activity against both aerobic and non-spore-forming anaerobic microorganisms.
Despite many years of intensive use of ointments containing chloramphenicol or dioxidin, their high antimicrobial activity remains against the main causative agents of surgical infection.
If there are gram-negative bacteria in the wound, in particular Pseudomonas aeruginosa, it is recommended to use 10% mafenide acetate ointment, 5% dioxidine ointment, dioxicol ointment, nitacid ointment.
For the treatment of non-sporogenous anaerobic infection in combination with aerobic infection, it is advisable to use the following drugs:
- with nitazol (Streptonitol and Nitacid ointments);
— foaming aerosol Nitazol;
- 5% dioxidine ointment, dioxikol ointment.
When using PEG-based ointments, side effects (clinically significant) are observed in 0.7% of cases, clinically insignificant - in 2.3% of cases. Most often they manifest themselves in the form of local symptoms of drug-induced dermatitis. In cases of intolerance to chloramphenicol, dioxidin, treatment can be carried out with oflomelid ointment or 5% miramistin ointment, which has not only a wide spectrum of antimicrobial activity, but also antiviral and antifungal effects, which is extremely important in the treatment of patients with trophic and long-term non-healing wounds.
Of the new ointments, the domestic drug streptolaven deserves special attention, which includes an enzyme of microbial origin (streptolysin), an antimicrobial drug miramistin and a base balanced in osmotic action that does not cause drying of wound tissue. This is the only ointment in the country with a necrolytic effect and is currently successfully used in the treatment of patients with diabetic foot syndrome, extensive burns, trophic ulcers, and bedsores [9].
The possibilities for successful treatment of patients with purulent wounds, trophic ulcers, bedsores, infected burns have significantly expanded with the advent of the new ointment Stellanin-PEG 3%, containing 1,3-diethylbenzimidazolium triiodide, low molecular weight polyvinylpyrrolidonium, dimexide, polyethylene oxide 400 and 1500. The bactericidal effect of the drug is due to the incoming it contains active iodine [9].
As can be seen from table. 3,
Stellanin-PEG ointment 3% is not inferior in antimicrobial activity to well-known drugs (levomekol, 5% dioxidine ointment).
Stellanin-PEG has high antimicrobial activity against both gram-positive and gram-negative microorganisms, including methicillin-resistant staphylococci (MRSA), E. faecalis, E. faecium,
as well as
E. coli
and
Klebsiella
spp., producing extended-spectrum beta-lactamases, and is also able to suppress the vital activity of fungi
(C. albicans).
In the treatment of wounds and trophic ulcers with severe pain, a high clinical effect is achieved using the new PEG-based ointment oflomelid, which contains lidocaine as an analgesic component and ofloxacin as an antimicrobial component.
Particular severity of the wound process occurs when the patient develops a polyvalent allergy. The solution in such clinical situations is the use of drugs containing silver (Argosulfan ointment - for light wound discharge) or Actisorb Plus dressings (non-woven nylon fiber with activated carbon and silver ions).
For the treatment of wounds with a moderate amount of wound discharge and a slow regeneration process (long-term non-healing wounds, trophic ulcers, diabetic foot syndrome, bedsores, etc.), the use of the original domestic drug 15% Dimephosphone, which has membrane-stabilizing, anti-acidotic, antimicrobial, anti-inflammatory activity, is indicated [10 ].
Treatment of wounds in phase II of the wound process
For the treatment of moderately or slightly exuding purulent wounds in the stage of transition to phase II of the wound process, as well as in the treatment of donor wounds during free skin grafting with autodermograft, the use of biologically active gel dressings Apollo PAK and Apollo PAA, which include iodovidone or miramistin, is indicated. also local anesthetic anilocaine. The hydrogel is based on a copolymer of acrylamide and acrylic acid.
If signs of a regenerative process are detected in the absence of profuse suppuration and mild symptoms of inflammation remain, it is possible to treat wounds under bandages using iodine-containing solutions: 10% Iodopirone, 1% Iodovidone, 1% povidone-iodine, Sulyodopirone.
After the acute purulent process has stopped and symptoms of intoxication have disappeared, confirmed by both clinical and laboratory tests, it is possible to cancel general antibacterial therapy. In these cases, local treatment of wounds at the stage of preparation for final closure with sutures or plastic surgery is carried out under bandages with drugs:
- biologically active stimulating wound coverings with antimicrobial and local anesthetic effects (Digispon-A, Algikol-FA, Kollakhit-FA, Anishispon);
— collagen-containing wound coverings (Gentatsikol);
— wound coverings based on alginates (Algipor, Algimaf);
— wound covering with silver based on collagen and regenerated cellulose (Promogran-Prisma);
— foaming aerosols (dioxysol, gentazol, nitazol);
- ointments with slight osmotic activity (Methyldioxylin, Argosulfan, Fuzimet, Streptonitol, Biopin 5%, 10%; Baneocin);
- oils (Miliacyl, sea buckthorn oil, rosehip oil).
The appearance in hospitals of a new Fuzimet ointment (a combination of fusidine sodium with methyluracil) makes it possible to successfully treat patients with methicillin-resistant S. aureus
(MRSA), without including vancomycin or linezolid in complex therapy [7, 8].
Prevention and treatment of fungal infections during systemic and local antimicrobial therapy of wound infections
Excessive enthusiasm for various antibacterial drugs in the treatment of infectious processes without mandatory simultaneously prescribed antifungal therapy has led to the fact that the problem of deep mycoses in recent years has become extremely urgent and difficult to solve. For example, the mortality rate for candidal pneumonia is 65-70%.
Disseminated candidiasis accounts for up to 10-15% of all nosocomial blood infections. With disseminated candidiasis, fungal infection of the skin is possible with the formation of subcutaneous abscesses, cellulite or individual muscle groups (candidal myositis). Fungal infections of the kidneys and lungs, nervous system, heart, spine, costal and sternoclavicular cartilages, stomach, intestines and bile ducts are extremely difficult to treat.
Candidaemia can be the direct cause of death in 75% of cases, and candidal sepsis as a cause of death can reach 88%.
Diabetes mellitus, antibiotic treatment, the presence of indwelling catheters, and severe neutropenia predispose to colonization of a fungal infection. Disseminated candidiasis is possible as a result of infection during surgical operations, invasive diagnostic procedures (puncture, biopsy, endoscopy), hemodialysis and peritoneal dialysis. Up to 40.2% of medical personnel may be carriers of Candida
spp., with 31.3% of them in association with
S. aureus,
43.7% with coagulase-negative staphylococci, and 25% in monoculture.
Prevalence of oropharyngeal carriage of fungi of the genus Candida
spp. among the medical staff of the general surgery department is 61.5%.
According to a study carried out at the Institute of Surgery named after. A.V. Vishnevsky, frequency of Candida albicans
from various biological media and catheters was detected in 8.6-12% of cases. The most dangerous source of the spread of fungi was a solution of furatsilin, from which fungi were detected in 58.8% of cases.
Traditionally, to prevent fungal infection, along with antibacterial drugs in such cases, ketoconazole or (in case of generalized infection) fluconazole, flucytosine or amphotericin B are prescribed. In case of generalized fungal infection, the duration of etiotropic therapy usually ranges from several weeks to a year.
Timely abandonment of long-term systemic antibacterial therapy, abandonment of traditional antiseptics (furatsilin solution), traditional absolutely ineffective fat-based ointments and active use of drugs such as 1% povidone-iodine solution, solutions of Prontosan, Lavasept (0.1%, 0. 2%) or 0.5% Miramistin ointment allows not only to avoid serious complications of the wound process, but also to successfully combat fungal invasion without resorting to systemic antifungal therapy.
Thus, the pharmaceutical industry currently has the opportunity to produce a fairly complete range of modern, highly effective drugs for successful local medicinal treatment of wounds, trophic ulcers, bedsores of various locations and origins. Timely active introduction of these drugs into the daily practice of practical healthcare can significantly reduce the cost of purchasing systemic expensive foreign drugs (there are no domestic drugs).
However, I would like to draw the attention of leading pharmaceutical manufacturers to the unacceptable cessation of production of such drugs as 5% dioxidine ointment, dioxicol, nitacid, streptonitol, 1% iodopyrone ointment, 0.5% quinifuril ointment, foaming aerosols (dioxysol, gentazol, nitazol, domestic hydrocolloids galagran and galactone, collagen coating with gentamicin gentacycol, wound dressings containing sodium alginate (algipor, algimaf).
The current situation requires an active position of all specialists involved in the treatment of surgical infections. It is extremely important to review the standards of wound treatment using modern drugs, since from the standpoint of evidence-based medicine, such standards can reduce mortality in patients with sepsis to an average of 26.5%, which is of extreme social significance.
Timely equipping of emergency medical teams, teams providing assistance to victims of natural and man-made disasters, military conflicts, outpatient clinic doctors, trauma centers and hospitals, specialized purulent surgery departments with modern drugs for local treatment of wounds will undoubtedly help reduce the development of severe purulent wounds. complications and diseases, will reduce the cost of antibacterial drugs by 2-3 times.