How to get rid of fecal stones at home
Fecal stones (coprolites) are dense formations (sometimes very hard) that have formed in the colon during prolonged stagnation of intestinal contents. There can be one stone or many.
Sometimes they reach a diameter of 10-15 cm. The stones may be mixed with mucus and sometimes have a layered structure. The stones may consist solely of magnesium carbonate, or 80% lime carbonate or "fatty-waxy masses" formed from large consumption of very fatty foods that contain refractory fats of animal origin.
Stones can also form from accidentally swallowed berry seeds or animal bones, pills, poorly cooked food and hair. Sometimes large gallstones and urinary stones enter the intestines through fistulas. Fecal stones usually form in old age.
Causes
Most often, intestinal stones form in older people, whose intestinal system is subject to age-related changes. In addition, people with health problems are at risk:
- atony or hypotension of the rectum;
- Parkinson's disease;
- persons who abuse fatty foods.
The main causes of stones are:
- unbalanced diet, abundance of unhealthy foods, fast food, sweets;
- passive lifestyle;
- alcohol abuse and smoking;
- accidentally eaten bones of berries, fish or animals;
- undigested food remains;
- penetration of foreign objects, tablets, hairs into the colon.
It has been proven that coprolites are formed when antacid drugs are used in large doses. Under the influence of bacteria, residual particles undergo rotting for a long time and collect into lumps.
If fecal deposits are not removed in a timely manner, the process may worsen. This will lead to intestinal obstruction, which can only be cured by surgery.
Symptoms
The main symptoms of stone formation are:
- haemorrhoids;
- chronic constipation;
- fatigue and weakness;
- low performance;
- nausea;
- pain and discomfort in the epigastric region;
- bloating and flatulence after eating;
- heaviness in the stomach;
- heartburn;
- headache;
- dysbiosis.
Heavy coating of the intestinal walls with feces contributes to the formation of the so-called plug. This plug blocks the intestinal lumen and disrupts intestinal motility. As a result, unpleasant symptoms and discomfort appear. At the initial stage of the formation of stones in the lumen, a deterioration in the functioning of the gastrointestinal tract is observed, but when the formations become larger, they poison the body from the inside, having a negative effect on other internal organs.
Why cleanse your intestines?
Cleansing the body has a positive effect on the condition of human internal organs, and also significantly improves appearance. The skin becomes cleaner, fresher, rashes on the body and face disappear, and mental clarity is restored.
Poor nutrition and overeating cause great harm to the body. It is clear that the rhythm of life in which a person arrives today does not always work out; there are healthy products that are correctly combined with each other. But it is necessary to understand that with poor nutrition, there is an imbalance between energy expenditure and energy intake.
Harmful substances coming from food are deposited in the form of cholesterol plaques on the walls of blood vessels and settle in the intestines, joints and adipose tissue.
The cleansing technique involves a sequence due to which this process gives the best effect. It looks like this: first we cleanse the entire large intestine, then the liver, stomach, kidneys, blood vessels and joints.
There is a pattern - the greater the degree of contamination of the intestines, the more difficult the process of cleansing all other organs will be.
What is the danger?
Fecal stones lead to disruption of intestinal functions and slower intestinal motility.
This pathology leads to the development of the following complications:
- chronic constipation;
- autoimmune diseases;
- allergic reactions;
- general intoxication of the body;
- the appearance of malignant tumors localized in the rectum.
Among the most dangerous complications of fecal stones for the patient, doctors identify internal bleeding and intestinal obstruction.
1.General information
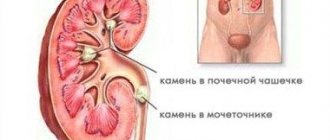
When applied to the human body, the word “stones” (calculi) means dense deposits in hollow organs or on hard surfaces, such as tooth enamel, which are formed as “sedimentary rock” and are a complex composite of various salts. Depending on where exactly calculus formation (the process of stone formation) starts, these can be salts of uric, oxalic, phosphoric, carbonic and other acids. The most common locations are the kidneys, urinary and gallbladder, corresponding ducts, and intestines.
Fecal stones, as the name implies, form in the large intestine, along the path of removing digestive waste from the body. Their composition and mechanism of formation are somewhat different from the composition and etiopathogenesis of, say, bladder stones, but problems can arise no less serious, including intestinal obstruction.
There are practically no statistical data on the prevalence of this phenomenon; Available sources only agree that the probability of colonic stone formation is in direct correlation with age, i.e. As we grow up and age, tissue wear and tear and the accumulation of various types of pathological changes, more and more favorable conditions are created for the formation of fecal stones.
A must read! Help with treatment and hospitalization!
How to cleanse the intestines of fecal stones?
For small-sized fecal stones, doctors prefer to use conservative treatment methods.
For these purposes, the following therapeutic techniques are used:
- Siphon enemas.
- Taking laxatives (used only periodically to avoid addiction).
- Cleansing enemas that improve intestinal permeability. Microenemas and enemas with decoctions of such medicinal herbs as motherwort, linden blossom, and chamomile have a good effect. It is recommended to do enemas daily for a week, then take a week break and repeat the treatment course again.
Such an effective procedure as hydrocolonoscopy deserves special attention, it promotes the maximum passage of feces from the intestinal walls and allows you to cleanse the intestines. The use of glycerin suppositories has a good effect. This method of treatment is especially recommended in the presence of fecal stones in young patients.
How to remove coprolite
A proctologist will help you get rid of discomfort in one visit. The procedure is quick and rarely requires pain relief. The doctor works carefully with his finger or auxiliary instruments. Removal steps:
- The patient undresses below the waist and lies sideways on the couch.
- The proctologist generously applies a special lubricant to the anus area.
- The doctor puts on gloves, treats the finger with lubricant and carefully removes parts of the fecal stone. If necessary, he helps himself with a sterile instrument.
- After the procedure, the proctologist will make sure that the rectal mucosa is not damaged, there is no bleeding, and the patient feels well.
- A specialist will advise you on how to avoid relapse. If required, he will refer you to a gastroenterologist and nutritionist.
Enemas
You can eliminate feces in the intestines using folk remedies. An enema is one of the accessible and simple ways to remove accumulated toxins yourself.
- Ognev's enema. The cleaning method was invented by the domestic doctor Ognev. To prepare, you will need a glass of hydrogen peroxide 3%, a glass of glycerin, 200 g of soap and ½ glass of dry wine. After douching, the patient remains in a lying position for a quarter of an hour. During the cleansing process, a burning sensation may occur. This method is prohibited for inflammatory processes in the colon, as well as for diseases of the sigmoid and colon.
- An enema based on pumpkin honey provides gentle and gentle cleaning. First, you should cleanse with a regular enema consisting of water. Then prepare a mixture consisting of 300 g of honey and a glass of warm water. The resulting solution is injected into the rectum and left for 30 minutes. The procedure is carried out over 5-7 days. This method can painlessly remove seals, as well as cure some skin pathologies and papillomas.
- Cleaning based on olive and sea buckthorn oils, as well as using Vaseline, vegetable or hemp oils. Oils are used separately, not in combination with each other. The procedure will require about 100 g of the ingredient, warmed to room temperature. This enema has an enveloping effect on stones, facilitates their easy removal, and does not have an irritating effect on the intestines. The patient must remain in a lying position for 30 minutes.
Constipation in children
If a child experiences constipation, especially chronic constipation, treatment should never be delayed. Prolonged bowel retention only aggravates the problem. The feces become dense and damage the intestinal mucosa, which leads to painful bowel movements - as a result, the child endures and deliberately avoids going to the toilet. Accumulating feces stretch the ampulla of the rectum, and encopresis (fecal incontinence) may subsequently form.
Parents are often interested in what to do if a child is constipated at 1 or 2 years old. The situation with stool retention in a newborn, one-month-old baby or infant becomes even more difficult for mothers and fathers. Young children are scared to use laxatives, especially since many of them are contraindicated at an early age.
To eliminate acute stool retention in a child from the neonatal period, MICROLAX® can be used: it has no age restrictions, and is also approved for infants. If constipation occurs, therapy should be supplemented with other measures - diet, increased fluid intake, increased physical activity.
For newborns and infants who receive only mother's milk, the diet must be followed by a nursing woman. When feeding with formulas, it is recommended to use special nutrition. Infants over 4 months of age need to introduce vegetable and fruit complementary foods in a timely manner.
Up to contents
Siphon enema
This type of enema involves the use of a large amount of liquid at a relatively fast pace for emergency lavage of the colon according to the following indications:
- Ineffectiveness of a standard enema.
- Intestinal obstruction.
- Emergency removal of toxins.
Technique:
Water is poured in 1 - 2 liters at a time; you will need a ladle of the appropriate size. A glass mug requires no less volume. The patient takes the desired position (for example, on the right side with his knees tucked), the doctor inserts a tip lubricated with Vaseline to a sufficient depth. The literature gives a value of 30-40 cm; it is necessary to take into account the anatomical features of the person for obvious reasons.
Excluding the ingress of air, the volume of the ladle is pumped into the colon. Then the mug is lowered, the contents need to be poured into a collection container. The procedure is repeated 10-12 times. The number of repetitions should be maintained, even if the wash water is clean. For the most part, the procedure eliminates constipation.
Folk remedies
Traditional medicine, more than ever, has its own approach to getting rid of fecal stones at home.
- Castor oil . To prepare a cleanser, you should take castor oil at the rate of 1 gram per 1 kilogram of human weight. Heat the oil using steam. Squeeze lemon juice in an amount of 2 parts juice to 1 part oil. Quickly drink warm oil and wash it down with lemon juice. Do not eat or drink anything for 12 hours after taking the medicine. It is better to carry out the procedure at night; in case of severe nausea, you can chew a little raisins. Cleansing begins after 2 hours, and removal of toxins after 12 hours.
- Vodka with oil . Combine 40 milliliters of unrefined sunflower oil and 20-40 milliliters of vodka in a tightly closed container. Close the container tightly and shake by shaking for 5 minutes. Open and drink everything as quickly as possible. This mixture should be drunk 3 times a day 30 minutes before meals. Try to alternate applications at equal intervals. Use the mixture for medicinal purposes for 10 days in a row. Take a break for 5 days and repeat the oil-vodka course again. After the third course, take a break for 2 weeks. If necessary, repeat this treatment circle for up to 2-3 years.
- Oatmeal and rice porridge . Take equal amounts of rice and oats. Boil both cereals in salted water. You need to eat this porridge in the morning and evening for a week. This medicinal porridge removes the remains of undigested food, fecal stones, heals cracks in the intestinal mucosa, perfectly cleanses this organ, and increases its tone.
- Glycerin suppositories . You can cope with coprolites without an enema by using glycerin suppositories. These are rectal suppositories, thanks to which you can delicately cleanse the intestines of stones. They soften stones, eliminate painful bowel movements, and improve intestinal function. The use of glycerin suppositories is contraindicated for anal fissures and exacerbation of hemorrhoids.
- Prune infusion . Wash 100 g of prunes, pour 0.5 liters of boiling water over them, let it brew. Drink a glass of infusion 3 times a day. Prunes perfectly cleanse the intestines, fight constipation, remove discomfort in the stomach, and normalize metabolism.
The main complication of fecal stones is the occurrence of intestinal obstruction (partial or complete).
Irritable bowel syndrome
The human intestine is a corrugated tube, 7-8 m long. It is divided into two sections - the small and large intestine. The small intestine (its length ranges from 5 to 6 m) connects the stomach with the large intestine. The main function of the small intestine is to digest food from the stomach and absorb the nutrients the body needs. The large intestine, up to 1.5 m long, ends with the rectum and anus. The main purpose of the large intestine is to absorb water and form feces.
Irritable bowel syndrome is an overly sensitive gut that reacts painfully to the most ordinary life situations, such as breakfast, getting ready for work, an upcoming date, not to mention events such as a holiday dinner, a call to the boss, a quarrel with loved ones.
How does increased intestinal sensitivity manifest itself? First of all, by disrupting the progression of content along its logical path from top to bottom. The bolus of food either moves faster than normal, making pendulum-like movements, or remains in some segment of the intestine, or even moves in the opposite direction.
Irritable bowel syndrome is different from stomach ulcers, pneumonia and osteochondrosis.
The main difference is the absence of a morphological basis for the disease. What does this mean? It is well known that, for example, with a peptic ulcer there is a defect in the mucous membrane of the stomach or duodenum, with pneumonia there is an area of compaction of the lung tissue, with osteochondrosis there is a decrease in the height of the intervertebral space. That is, in all of the above examples there is a so-called substrate of the disease - something that causes complaints. With irritable bowel syndrome, there are complaints, but there is no substrate, at least not determined by modern diagnostic studies.
For irritable bowel syndrome, there are diagnostic criteria, the so-called “Rome criteria”, which got their name due to the fact that they were first published in Rome. According to the Rome Criteria, for 12 weeks over the past year (not necessarily consecutive) you may experience abdominal pain or discomfort or bloating, which is relieved after a bowel movement, associated with a change in stool frequency or consistency. The pain can vary from a feeling of mild discomfort to unbearable, may not have a clear localization, spreading throughout the abdomen, or occur at different times in different areas of the abdomen. The pain can be very different - burning, dull, aching, cutting, bursting, squeezing, etc. It usually gets worse after eating. A very important point is the absence of pain at night. You don't wake up in pain.
However, if your sleep is disturbed and you wake up during the night, pain may immediately occur. Bloating usually increases during the day, reaching a maximum in the evening, and is noticeably worse after eating (most often after lunch).
Stools are most often observed in the morning, after breakfast, the number of bowel movements ranges from 2 to 5, with short time intervals. Urge to defecate may occur after every meal. The urge to defecate is also typical in situations where it is not possible - meetings, trips on the subway, commuter trains, in stressful situations. Quite often, due to an urgent urge to defecate, you refuse to visit theaters, cinemas and other public places. However, diarrhea never occurs at night. In addition, stool weight remains normal and, as a rule, does not exceed 200 g per day.
Quite often there is a feeling of incomplete bowel movement. There may be mucus and undigested pieces of food in the stool, but never blood or pus. Immediately before the act of defecation, there is an increase in pain and a significant decrease in pain after it. Most often, the stool is “sheep”, i.e. consisting of small dense fragments, “cork-shaped” - i.e. The first portions of feces are denser than the subsequent ones; there may also be pencil-shaped stools - narrow, long ribbons. So-called constipative diarrhea may occur - loose stools after several days of delay.
You may be plagued by a host of other problems, such as a feeling of a lump in the throat when swallowing, pain in the epigastric region, a feeling of rapid satiety, nausea and pain in the right hypochondrium, pain in the left half of the chest, pain in the muscles, joints, back, headaches , palpitations, a feeling of interruptions in the work of the heart, the inability to sleep on the left side, a feeling of incomplete inspiration, internal trembling, increased urination, weight loss, tinnitus, a feeling of weakness, a feeling of “hot flashes” and dry mouth.
The prevalence of this disease among the population varies in different countries from 9 to 48%. However, due to the rather delicate nature of the complaints, only 14-66% of patients consult a doctor. Most often, urban residents aged 30 to 40 years are affected, with women 3-4 times more likely than men. Most often, irritable bowel syndrome develops after traumatic situations, such as divorce, bereavement, loss of a job or other significant incidents, much less often after a foodborne illness; a hereditary predisposition is also possible. Some scientists are of the opinion that eating chocolate, coffee, alcohol, lentils, beans, dairy products, as well as rich food, changing the usual eating pattern during business trips and travel can be a trigger for the onset of symptoms of the disease.
What to do if you have all or part of the above symptoms? It is imperative to consult a doctor. Firstly, in order to confirm the diagnosis. Unfortunately, there are various conditions in which the clinical picture of the disease partially or even almost completely corresponds to that described above, but the diagnosis is ultimately made differently, the treatment required is completely different, and sometimes urgent. Secondly, in the case of a confirmed diagnosis, treatment must be selected by a specialist, taking into account many factors.
The life prognosis for this disease is favorable. Irritable bowel syndrome does not lead to the development of bowel cancer or diseases such as ulcerative colitis or Crohn's disease. However, it is advisable to be under the supervision of a doctor in whose competence you are confident, whom you completely trust and can tell about the most minor changes in your well-being and the reasons that, in your opinion, caused them. You need to pay attention to how you eat. It is completely unacceptable to eat 1-2 times a day and in large quantities. This diet will undoubtedly cause abdominal pain, bloating, and bowel dysfunction. Eating more than 4-5 times a day and in small portions will make you feel better. In some patients, a certain set of foods leads to increased symptoms, so it is advisable to keep a so-called “food diary” in order to identify foods that may cause a worsening of the condition. It is necessary to write down what foods you consumed during the day, and what unpleasant sensations arose. A fragment of the “food diary” is presented below.
| Product | Symptom |
| rice | – |
| coffee | twice loose stool with mucus |
| Boiled potatoes | bloating, excess gas |
There is no cure for irritable bowel syndrome. There are only medications that relieve the symptoms of the disease. They are quite effective and, for the most part, do not cause side effects. The choice of a particular drug depends on which symptom of the disease is currently bothering you the most. For abdominal pain, medications that weaken intestinal motility can be prescribed; for diarrhea, constipating medications can be prescribed; for constipation, laxatives; and for bloating, medications that reduce gas formation.
Remember! The choice of drug or combination of drugs and the duration of the course of treatment are determined by the doctor!
Unfortunately, the effect of the prescribed treatment is sometimes insufficient, sometimes short-lived, and in some cases completely absent, which is due to the fact that all of the above groups of drugs act only on intestinal functions, without affecting other factors that contribute to the symptoms of the disease.
The mechanism of development of clinical signs (symptoms) of irritable bowel syndrome can be represented as follows: under the influence of psychological stress or a chronic traumatic situation; much less often - intestinal infection; in some people, to which you belong, the intestine becomes overly sensitive.
Firstly, the threshold for pain perception decreases and, secondly, the intensity of pain perception becomes inadequate to the stimulus that causes it. Painful impulses from the intestines come to the brain. Since the brain receives an excessively strong impulse, the response signal sent to the intestine is also excessive. In response to the strong impulse received, a disturbance in the motor activity of the intestines occurs, which you feel as abdominal pain, bloating, diarrhea or constipation.
Can we influence the intensity of the impulse going from the gut to the brain or in the opposite direction? Theoretically we can, but in practice it is quite difficult. Just as the waters of many streams, flowing into a river that carries them to the ocean, become indistinguishable, so the signals from many organs that follow in the interweaving of nerve fibers to the brain are practically inseparable, and it is possible to single out a “path” along which information from the gut follows almost impossible. Can we influence the intensity of the impulse formed in the brain? Yes, and quite effectively.
The effectiveness of both medicinal and non-medicinal methods of influence is recognized throughout the world. Non-drug methods include, for example, individual and group psychotherapy, hypnotherapy; for medications - the use of tricyclic antidepressants, selective serotonin reuptake inhibitors.
Remember! The choice of treatment method is determined by the doctor!
Irritable bowel syndrome does not predispose you to the development of tumors or inflammatory bowel disease. However, in order to live a full life, you must try to avoid overwork, stressful situations, and eating foods that lead to symptoms of the disease; and if you feel worse or if new symptoms appear, visit your doctor.
Honored Health Worker of the Republic of Tatarstan, general practitioner of the highest category, Doctor of Medical Sciences, Professor
F.I. Mukhutdinova
Medicinal colon cleansing
Cleansing the intestines from fecal stones using medications can be done in any specialized medical institution where it is possible to carry out this procedure in a hospital setting under the supervision of a competent doctor. For this purpose, ordinary boiled water is used, introduced into the anus through an enema.
It should be noted that doctors resort to this procedure only in the most extreme cases, when the problem that has arisen has to be solved against the background of intoxication of the body. It is also necessary to take into account the fact that enemas wash out beneficial microorganisms from the intestinal microflora along with toxins, which carry the function of processing and assimilation of food.
Even if instead of boiled water, decoctions of medicinal plants or boiled oil are used. This method is not suitable for people who have undergone intestinal surgery or suffer from bleeding of internal organs or hemorrhoids. After the intestines are washed, you should think about restoring its microflora, for which it is recommended to take drugs such as Bifidumbacterin or Linex.
The most gentle method of intestinal cleansing is the use of laxatives, which are produced today in a wide variety in the form of suspensions, mixtures, suppositories, and tablets. The principle of action of all laxatives is based on enveloping the intestinal walls with a film that prevents the absorption of fluid. The result of this process is spontaneous liquefaction of stool, followed by its removal from the body, 6-7 hours after taking the laxative.
However, we should not forget that medications with a laxative effect contribute to the leaching of potassium from the body, which is necessary for the full functioning of the heart muscle. This should be kept in mind by persons suffering from cardiovascular insufficiency, and bowel cleansing should be carried out in this way only if there is no other way to get rid of constipation and restore full bowel function.
Treatment
Both chronic and acute constipation must be treated to alleviate your condition and avoid complications.
Proper use of laxatives
Regardless of the reasons, treatment of constipation with stool retention for 3 days or more requires preliminary cleansing of the intestines.
For this purpose, the following are most often used:
- laxatives,
- suppositories with glycerin,
- cleansing enemas.
What to do if you have severe constipation? Taking laxatives by mouth (oral) helps very slowly and unpredictably. Moreover, unpleasant side effects may occur, such as increased gas formation, rumbling and cramping abdominal pain. But some oral medications are well suited for the complex treatment of chronic conditions and the prevention of constipation.
The best option for cleansing the intestines during acute, including long-term and severe, stool retention is the drug MICROLAX®, produced in the form of microenemas. Compared to oral laxatives, it can take 5–15 minutes to work1. Other advantages of MICROLAX® include a high safety profile when following the instructions for medical use of the drug (it has no age restrictions or special contraindications) and a convenient release form - microenemas in individual single-use packaging. With the help of MICROLAX® it is very easy to get rid of constipation at home - administering a microenema does not require special skills. It is enough to simply insert the tip into the rectum, after squeezing out a drop of MICROLAX® to lubricate the tip (for a child under 3 years of age, insert the tip only halfway, up to the mark on it, or use MICROLAX® for children) and completely squeeze out the contents of the tube, then remove the tip , still lightly squeezing the tube.
Severe constipation is a common occurrence in hospital patients, especially those who have undergone surgery, and in pregnant women during their stay in the maternity hospital. Problems with bowel movements can also occur on the road (long train trips, business trips). In such situations, MICROLAX® can also help you - it can be used in the postoperative period and during pregnancy, and thanks to its convenient format it is very simple.
MICROLAX® has no restrictions on the duration of use and is suitable for the treatment of chronic constipation. In this case, a complex treatment therapy must be selected by a doctor.
Compliance with diet and drinking regime
To normalize stool, the use of laxatives alone is not enough. Nutrition is of great importance. Activation of intestinal motility, softening of feces and growth of beneficial microflora is promoted by dietary fiber: pectin, lactulose and coarse plant fiber. They are found in large quantities in fresh vegetables, fruits, berries, and grain shells (whole flour, bran, muesli).
Including fermented milk products in the diet - low in fat and fresh, additionally enriched with representatives of normal intestinal microflora (lacto-, bifidobacteria) - helps to get rid of constipation.
To normalize stools, it is imperative to increase fluid intake, in the form of bottled or boiled water.
Increasing physical activity
Regular exercises - gymnastics, swimming, running - contribute to timely cleansing of the intestines.
Solving psychological problems
Psychological problems and stress are common causes of constipation. For a young child, a change of environment, including entering a kindergarten or school, will be stressful. Children are often embarrassed to go to a public toilet and systematically hold back their stool. As a result, the feces become denser, the ampulla of the rectum expands, which leads to painful bowel movements, which is why the child is increasingly afraid to go to the toilet and a vicious circle is formed. Failure to treat this condition in children can lead to the development of serious complications in the future, such as stool, megacolon, rectocele, etc.
In case of constipation in adults, nervous overstrain and chronic stress also play an important role, therefore, in case of chronic problems with stool, the help of a psychologist and training in relaxation techniques would be useful.
Normalization of the daily routine
A normal daily routine is not only about adequate sleep and rest. This also includes achieving regular, daily (and preferably at the same time) bowel movements. The formation of a bowel rhythm is helped by the use of MICROLAX® in the initial stages of treatment - the use of a microenema in the morning helps to develop and strengthen the habit of going to the toilet at this time of the day.
Treatment of the underlying disease
If any disease is the cause of constipation, then to eliminate problems with stool, you must first begin treatment. In case of organic pathology (tumor, diverticula, congenital intestinal anomalies), surgical intervention may be required.
Up to contents
Prevention
Having been freed from coprolites and accompanying symptoms, a person should feel better and the functioning of internal organs should improve. From now on, it is necessary to adhere to certain rules in order to avoid the recurrence of the disease. Preventive measures look like this:
- limiting the consumption of fatty, spicy, salty foods that cause constipation;
- drinking at least 2 liters of liquid per day (boiled water, juices, green tea, compotes);
- rejection of bad habits;
- maintaining an active lifestyle, performing moderate physical activity;
- regulation of nutrition - adherence to the regime and measures in food;
- including more fresh fruits and vegetables in the diet;
- tracking bowel regularity.
If you experience intestinal bleeding or prolonged constipation, you should consult a doctor.