AUTHORS: Daniel London, Oded Nahlieli
Keywords:
sonography (ultrasound), salivary glands, parotid gland, submandibular gland, sublingual gland, stones, tumor, inflammation
Key points
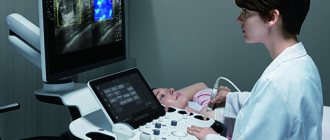
- The salivary glands are superficial and can therefore be examined in detail using ultrasonography.
- It is important to scan each gland sequentially according to the protocol.
- The salivary glands can be affected by inflammatory, benign and malignant pathology, which can be detected sonographically.
- The salivary glands may have congenital anatomical abnormalities and may contain calculi, which are also detected sonographically.
- The purpose of the article is to gain in-depth knowledge about the structure of healthy glands, available sonography techniques, pathological changes and differential diagnosis of diseases.
Physical basis and equipment
Ultrasound is a high-frequency acoustic wave that uses a frequency outside the normal hearing range (20 Hz-20 kHz). Most head and neck and maxillofacial equipment are tuned to 8 MHz (8 million cycles per second) or higher. This is in contrast to ultrasound diagnostic devices used in general surgery or obstetrics, which typically operate at a frequency of 5-6 MHz, which provides greater tissue penetration but reduces image resolution. Sensors generating frequencies up to 20 MHz and, in the case of ultrasound biometry, up to 50 MHz, are now also used for imaging the salivary glands. This allows very small structures to be distinguished.
The three major salivary glands (parotid gland, submandibular gland and sublingual gland) are paired and are easily accessible due to their superficial location for sonographic diagnosis using high-frequency linear transducers (8-18 MHz).
Nowadays, the use of high-performance ultrasound devices generates a sonographic image like an anatomy book, even using smartphone ultrasound. The resolution and penetration depth of ultrasound depend on the specified frequency. The higher the frequency, the better the resolution, but the penetration is worse. For visualization of the salivary glands, linear probes with a frequency of 7.5 MHz (5.0-13.5 MHz) are most effective. Box 1 shows the scanning sequence.
| Box 1 Scan sequence
|
Under normal conditions, the three major salivary glands have a similar homogeneous intermediate echogenicity with sharp boundaries. Small salivary glands become accessible for sonographic diagnosis only in the presence of pathological changes (for example, enlargement due to a tumor or neoplastic process). Indications for sonographic examination include swelling or increased volume in the area of the salivary glands and pain. Ultrasound examination (Box 2) allows the doctor to clarify the localization, namely: whether the formation is located in the gland, or is simply adjacent to the contour of the salivary gland. This differential diagnosis often cannot be made solely on the basis of clinical examination.
| Box 2 Ultrasound Components
|
HOW TO SCAN (PROTOCOLS)
Parotid gland
The parotid gland can be easily examined with the patient's head turned to the side and in a hyperextension position. A summary of the scanning procedure is provided in Box 3.
| Box 3 Parotid gland scanning procedure
|
First, the gland is scanned in cross section, starting from the angle of the jaw to a point slightly above the tragus. Then the longitudinal projection is scanned. The ultrasound probe must be adequately applied to the surface of the skin, using a sufficient amount of gel, especially in the area of the angle of the jaw.
Submandibular gland
If the patient's head is moderately extended, the submandibular gland can be examined ultrasonographically without any problems. First of all, along the midline of the neck, the ultrasound sensor moves in the transverse direction from the hyoid bone to the horizontal branch of the mandible. Sometimes both submandibular glands may be visible at the same time. Then, by moving the transducer sideways, parallel to the horizontal ramus of the mandible, a clear image of the corresponding submandibular gland can be obtained. Here it is necessary to ensure good contact of the gel with the sensor on the skin.
Sublingual gland
The sublingual gland examination does not have significant differences in procedure compared to the submandibular gland examination. The transducer is placed on the skin in a transverse plane in the midline just below the mandible, allowing visualization of both sublingual glands. It is important to note that all averaged structures must be within 0.2 mm of each other, and any outliers are carefully assessed and discarded and, if necessary, reanalyzed.
ANATOMY
Update your anatomy knowledge
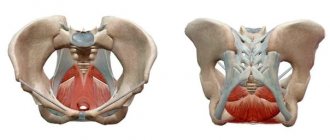
The parotid glands consist of a prismatic body and two elongated parts: the anterior part is located on the deep part of the masseter muscle, and the deeper elongated parts, which reach the lateral wall of the pharynx, pass between the prestyloid muscles and the stylomandibular ligament.
The submandibular glands are located in the submandibular space under the floor of the mouth and have a mesial extension called the “hook.” The excretory Wharton's duct arises from this expansion, which is located at the base of the frenulum of the tongue and opens into the sublingual papilla.
The sublingual glands are a group of glands located in the sublingual space, which are limited by the recess of the tongue, the floor of the mouth and the geniohyoid muscle.
NORMAL ULTRASONIC ANATOMY
Parotid glands
The parotid glands, which are the largest of the salivary glands, are enclosed in a separate fascia, which penetrates the glands, forming various lobules. In cross-section, the parotid gland is a sharply defined, homogeneous organ with intermediate echogenicity (Fig. 1).
Rice. 1. Normal parotid gland.
The gland can be clearly distinguished from subcutaneous adipose tissue. The anterior part of the gland sits on the masticatory muscle and can be differentiated from the buccal adipose tissue, which has lower echogenicity, by contraction and relaxation of the masticatory muscles. The posterior part of the gland is located in the retromandibular fossa and is clearly delimited anteriorly by the ascending ramus of the mandible, and posteriorly by the sternocleidomastoid muscle and the mastoid process. Mediocaudal to the inferior pole of the parotid gland, the posterior belly of the digastric muscle and the internal carotid artery can be distinguished. It is important to remember that a small portion of the parotid gland may be hidden by the acoustic shadow of the mandible.
In and around the gland, the internal jugular vein and the retromandibular vein can be found, which are located in the glandular parenchyma and can be visualized, especially in the longitudinal projection. In transverse views, distal to the retromandibular vein, the styloid process is projected onto the glandular parenchyma, which should not be confused with sialolithiasis. The facial nerve is usually not visible. However, with the use of modern high-resolution transducers, it is sometimes possible to obtain a sonographic image of the main outflow canal.
Submandibular gland
The submandibular gland extends cranial to the mandible and the geniohyoid muscle and has a close connection with the anterior belly of the digastric muscle. The submandibular gland forms an arch around the posterior border of the geniohyoid muscle and often reaches ventromedial to the submandibular gland. Echogenic structures with an element of acoustic shadowing are often projected in the area of the gate of the submandibular gland. In this area, it is necessary to carry out differential diagnosis between the elements of the hyoid bone and the sialoliths of the submandibular gland, which may have comparable characteristics on imaging [2,7]. Sonographic imaging characteristics of the submandibular gland include an intermediate echogenic structure with a regular echo pattern corresponding to the echo pattern of the parotid gland parenchyma (Fig. 2).
Rice. 2. Normal submandibular gland.
In and around the gland, the facial artery and facial vein, which pass through the gland, are easily distinguished sonographically. The path of the efferent duct can sometimes be visualized using high-resolution ultrasound probes, even in the absence of duct obstruction. If we are talking about differentiation of the elements of the hyoid bone, then during swallowing movements its displacements are observed.
Sublingual gland
Visualization of the sublingual gland can sometimes be problematic. The sublingual gland is located under the mucous membrane in the oral cavity, lower in the projection of the tip of the tongue, next to the frenulum of the tongue. The dorsal part of the glands often touches the surface of the submandibular gland.
The gland is bounded ventrally and medially by the geniohyoid and genioglossus muscles, and caudally by the mandible. Short excretory ducts usually cannot be visualized. Accumulation of saliva may be found in and around the sublingual gland, which forms the ranula (Figure 3).
Rice. 3. Sublingual ranula.
Treatment of salivary gland cancer
Fighting a life-threatening tumor is not an easy task. To solve it, the participation of many different specialists is necessary: oncologist, surgeon, chemotherapist, radiologist and others. It is extremely important that they all work together and exchange information in a timely manner, since only this approach allows taking into account all the characteristics of the patient.
The oncology department has a whole team of professionals with extensive experience in the diagnosis and treatment of any type of cancer. Our doctors are candidates and doctors of medical sciences, constantly improving their knowledge and skills. We use only the most modern equipment and original drugs that give predictable results. Our clinic’s specialists offer each patient individual treatment and draw up a clear plan, following which you can get the best possible result.
Several methods are used to combat this type of tumor. Surgery is often the main one.
. With the help of surgery, it is possible to completely remove tumors that have not seriously damaged nearby structures. The success of the procedure is largely determined by the experience and skills of the doctor, including because the nerves responsible for tongue movements, control of facial muscles and taste sensations pass near the salivary glands. During the procedure, the organ and surrounding healthy tissue are removed so that not a single altered cell remains in the body. In some cases, lymph nodes also have to be removed.
Radiation therapy
– destruction of cancer cells using radiation. The method can be applied:
- Alone or in combination with chemotherapy for some forms of tumors that cannot be treated with surgery alone.
- After surgery, possibly simultaneously with “chemistry” - to destroy any remaining changed cells and reduce the likelihood of recurrence of the disease.
- As palliative treatment in the final stages to relieve symptoms - reduce pain, eliminate bleeding or difficulty swallowing.
Chemotherapy
– destruction of abnormal cells with special drugs that are injected into blood vessels or taken like regular tablets. They enter the blood and spread throughout the body, thanks to which they work against all foci of the disease. Most often, such drugs are prescribed for patients with metastases - additional tumors in distant organs. Chemistry can reduce the tumor, but it cannot cure this type of cancer on its own. Some substances increase the effectiveness of radiation therapy and make it easier for radiation to destroy damaged cells. Such therapy is prescribed in courses, which are necessarily followed by a period of rest, allowing the body to recover. Typically, such cycles last from 3 to 4 weeks. To combat salivary gland cancer, drugs such as Cisplatin, Carboplatin, Doxorubicin, 5-fluorouracil, Cyclophosphamide, Paclitaxel, Docetaxel, Vinorelbine and Methotrexate are usually used.
PATHOLOGICAL RESULTS
Box 4 contains a short list of variants of salivary gland pathology.
| Box 4 Variants of pathology of the salivary glands
|
Acute sialadenitis
Since we have to deal with paired organs, it is important to compare both glands in one picture. Characteristic findings are explained by inflammatory edema and an increase in fluid content in the parenchyma, which is transformed during inflammation. Typically we see the following:
- Diffuse expansion of the entire affected gland.
- The organ can be clearly demarcated from adjacent structures.
- The structure of the parenchyma appears loose, heterogeneous, coarsely textured and more hypoechoic.
- Limited hypoechoic formations can be detected as a concomitant inflammatory reaction of the intraglandular lymph nodes.
- Zones of liquefaction (as signs of abscess formation) are visualized as hypoechoic with a hyperechoic surrounding wall and pronounced distal signal enhancement.
- Coarsely structured hyperechoic echoes at the center of such liquefaction lesions may correspond to areas of necrotic tissue.
Chronic sialadenitis
Sonographic imaging is highly dependent on the duration and degree of inflammation of the glandular parenchyma. As in the case of acute sialadenitis, a conclusive differential diagnosis between the various pathogenic forms of chronic sialadenitis cannot be made using sonography alone. Typically we see the following:
- A clear increase in the unevenness of the echo texture.
- The internal structure has a heterogeneous pattern, most likely due to fibrotic changes in the parenchyma.
- Small cystic echo lesions are formed, which correspond to limited ductal ectasia (Fig. 4).
- Sometimes stones within the gland are identified as echogenic structures with a distal acoustic shadow.
Rice. 4. (A) Chronic sialadenitis of the parotid gland. (B) Sialocele of the parotid gland. (C) Dilatation of Stenson's duct (arrows).
Differential diagnosis is important in the following situations:
- Patients suffering from Gougerot-Sjögren syndrome have sonographic signs of enlarged, heterogeneously structured, hypoechoic salivary glands. Numerous limited hypoechoic formations are found inside the parenchyma, which may be associated with cystic dilatation of the ducts, on the one hand, or with enlargement of intraglandular lymph nodes, on the other hand. Sonographically, the structure of the salivary glands looks like a “cloud”.
- Sialadenitis of epithelioid cells (Heerford syndrome) is sonographically characterized by a rich echo pattern interrupted by numerous enlarged lymph nodes that appear as hypoechoic masses.
- Kütner's tumor of the submandibular gland is visualized as a formation with an indistinct echo signal in a certain part of the submandibular gland, which is easily mistaken for an adenoma.
- Ultrasound helps detect changes after radiation therapy. The echohomogeneous pattern disappears after irradiation, with a more hypoechoic and sometimes irregular pattern being a sign of loss of function.
- Other secondary pathological changes (edema, infections and soft tissue tumors) around the salivary glands are easily distinguished from primary salivary gland pathology.
Parotid abscess
The evolution of the inflammatory process is characterized by a hypo-, anechoic lesion with irregular edges. Typically we see the following:
- Hypo-, anechoic lesion with irregular edges.
- Peripheral hypervascularization, which is determined by color Doppler scanning.
- In the case of partial necrotic changes, lymph nodes with anechoic areas of necrosis are identified.
- In the case of fistula formation, a fistula is defined that reaches the skin surrounded by edematous tissue.
An important initial sign of an abscess is the appearance of vessels with a linear and fairly regular direction, which subsequently changes to a more irregular one, and is characterized by numerous anastomoses, which can be determined by an increase in the intensity of the color Doppler signal. In abscesses, the color Doppler signal has a peripheral structure because in this case the vessels are intertwined along the periphery of the abscess.
Enlarged lymph nodes
Lymph nodes may be found inside the parotid gland. However, only around the submandibular gland, due to the characteristics of embryological development. In the parotid gland, a group of small lymph nodes (3-5 mm) is located along the retromandibular vein. These lymph nodes carry out lymph drainage from the Eustachian tube, external auditory canal and deep areas of the face. Intraglandular and extraglandular lymph nodes normally do not exceed 9 mm in diameter.
Ultrasound imaging of otherwise unremarkable glandular parenchyma may reveal predominantly multiple hypoechoic lesions that often lack any distal signal enhancement. Sonographically, as a rule, it is impossible to obtain reliable signs that would allow a definitive differential diagnosis between benign and malignant enlarged lymph nodes.
Reliable differential diagnosis between reactive lymphadenitis (Fig. 5), non-Hodgkin's lymphoma (Fig. 6), MALT lymphoma, or intraglandular metastatic spread is not possible on the basis of sonographic findings alone.
Rice. 5. Pathological lymph node.
Rice. 6. Primary lymphoma of the parotid gland.
Clinical signs, number, location, and sometimes texture of nodes can lead to diagnosis, but do not replace histological analysis. As with enlarged lymph nodes of the neck, some authors mention the so-called “hilus” (gate) as a sign of reactive lymphadenitis.
Cystic tumors
Congenital or acquired salivary gland cysts are usually filled with clear fluid. We usually see an echo-negative tumor with clear borders and distal signal enhancement (Fig. 7).
Rice. 7. Salivary gland cyst (arrows indicate parotid gland, arrowheads indicate cyst).
It is important to note that if cystic tumors are detected sonographically in both parotid glands, and if there is a relevant medical history, then lymphoepithelial cysts caused by HIV infection should be suspected.
Sialolithiasis
Although the sign of a distal acoustic shadow is usually detected, the signal reflection can sometimes be unclear or insufficient. This phenomenon is the result of a reflected ultrasonic component that does not reach the transducer but is scattered out of the image plane. Typically, we see an echo-opaque object with a clear sign of a distal acoustic shadow (Fig. 8) and dilatation of the excretory ducts.
Fig.8. Intraglandular sialolithiasis of the submandibular gland.
Parotid duct stones contain organic components and are visualized with great effort. Sometimes only a distinct echo-opaque object without a distal acoustic shadow may be detected. However, in many of these cases, dilatation of the efferent ducts of the salivary glands can be considered as another indirect sign of the development of sialolithiasis, if the stone cannot be clearly identified. However, dilation of the duct can also be caused by scar changes in the connective tissue (for example, the situation after an inadequately performed incision of the duct or after acute inflammation). Stones with a diameter of 1.5 to 2 mm or more, located in the area of the large salivary glands, can be reliably detected during sonography.
It is important to note that the precise determination of the position of sialoliths (intraglandular, extraglandular and intraductal) is of great importance. Differential diagnosis is important both in the presence of air inside the ducts and in the case of pneumoparotitis, foreign bodies, angiolithiasis and calcified lymph nodes or arteriovenous malformations (Fig. 9).
Rice. 9. Arteriovenous malformation of the salivary glands.
Remember, because of its limited sensitivity and limited negative predictive value, sonography does not reliably exclude small salivary gland calculi. Further diagnostic studies are needed to identify stones in patients with normal sonographic findings and suspected lithiasis.
Sialadenosis (sialosis)
All large salivary glands can be simultaneously affected by sialoadenosis. Sialadenosis is a non-inflammatory condition characterized by bilateral enlargement of the salivary glands, most commonly the parotid glands. Usually we see that the glands look indistinctly enlarged, are difficult to differentiate from surrounding structures, their echo structure looks homogeneously hyperechoic, and with sialoadenosis tumor-like lesions are not detected. In some cases, the parotid gland is so enlarged that ultrasound requires a low-frequency transducer to evaluate the deep part.
Benign epithelial tumors of the salivary glands
A well-defined boundary between the surrounding salivary gland tissue and the tumor itself is a characteristic feature of a benign salivary gland tumor. Because ultrasound is unable to visualize nerves, the relationship of parotid tumors to the facial nerve cannot be reliably determined.
Pleomorphic adenomas have a homogeneous/hypoechoic texture. However, sometimes heterogeneous structures with hard and cystic inclusions may be noticeable. In these cases, a characteristic feature is distal signal enhancement (Fig. 10).
Rice. 10. Pleomorphic adenoma of the parotid gland.
Monomorphic adenomas (adenolymphomas) may also appear sonographically homogeneous and hypoechoic, as is the case with pleomorphic adenomas. If the proportion of cystic structures is high, adenolymphoma may also present completely without echo with extensive distal enhancement. Occasionally, septae may be identified within the tumor.
The remaining less common types of benign salivary gland tumors (eg, basal cell adenomas, oncocytomas, lymphoepithelial lesions) also have similar nonspecific sonomorphological features.
Definitive sonographic identification and differential diagnosis between different types of benign salivary gland tumors is currently impossible, although significant cystic portions in the mass tend to indicate adenolymphoma, and the absence of cystic areas indicates pleomorphic adenoma. To a certain extent, parotid tumors can be classified as either the "superficial" or "deep" part of the gland.
Benign nonepithelial tumors of the salivary glands
Lymphangiomas and hemangiomas (Fig. 11 and 12) have similar sonomorphological characteristics, which makes differential diagnosis between them impossible.
Rice. 11. Intraglandular lymphangioma.
Rice. 12. Submandibular hemangioma.
During the study, loosely connected alveolar structural components, consisting partly of hypoechoic and hypergeogenic areas, can be detected. Sonographic examination allows us to assess the depth of penetration and spread of this tumor into the corresponding salivary gland and into the area of surrounding soft tissue.
Intraglandular and extraglandular lipomas (Fig. 13) appear as sharply demarcated, ovoid formations, with a hypoechoic and homogeneous signal reflection pattern.
Rice. 13. Well-defined lipoma.
Lipoma has a more characteristic hypoechoic reflection pattern than the rest of the salivary gland parenchyma, but its echo texture is more hyperechoic than other types of intraglandular tumors, and it also has a linear hyperechoic feathery texture.
Malignant tumors of the salivary glands
We typically see a fuzzy edge and a patchy echo texture. It is possible to describe the relationship between invasive tumor growth and surrounding tissue. It is impossible to detect involvement of the facial nerve in the malignant process. The most common malignant tumors of the salivary glands are mucoepidermoid carcinoma, adenoid cystic carcinoma, carcinoma arising in pleomorphic adenoma, and distant metastases (Fig. 14).
Rice. 14. Metastatic melanoma in the parotid gland (arrows indicate parotid glands, arrowheads indicate metastases).
Indications for sonographic examination are sometimes absent, since at the preoperative stage it is impossible to identify with complete certainty the benign or malignant nature of tumor development. If a malignant process is suspected, ultrasound-guided fine-needle aspiration biopsy can be a useful tool to more accurately classify the tumor at a preoperative stage.
It is important to note that if tumor margins cannot be accurately imaged by sonographic examination, especially when the tumor extends to osseous or deep structures, the patient's diagnostic imaging should be extended in any case to computed tomography and/or magnetic resonance imaging.
Gougerot-Sjögren syndrome
Gougerot-Sjögren syndrome occurs when lymphocytes invade and destroy the exocrine gland. It is the second most common autoimmune syndrome after rheumatoid arthritis, affecting the salivary glands in 40-80% of cases. This results in a higher incidence of parotid lymphomas and salivary stone disease. Typically we see the following:
- At an early stage, sonography is normal.
- Later, the glands become enlarged and large-scale structural damage occurs.
- The gland is heterogeneous.
- At a later stage, sonographic examination reveals sialoectasia and marked hypervascularization on color Doppler ultrasonography of the salivary glands.
The intraoperative role of sonography has become important since the introduction of minimally invasive surgical techniques in salivary gland surgery. During surgery, if endoscopic observation of the surgical field is not possible, sonographic guidance can be used to:
|
Rice. 15. Minimally invasive procedures under ultrasound guidance.
Rice. 16. Therapeutic intraglandular injection of Botox.
Color Doppler ultrasonography of the salivary glands
The standard B-scan is a well-established tool for diagnosing salivary gland diseases. For tumors located in the salivary glands, there is increasing interest in non-invasive collection of clinical information such as growth and invasiveness, as well as making an accurate diagnosis before surgery. Before the benefits of sophisticated ultrasonography became available, standard testing was performed by correlating simple sonomorphological criteria, such as anechoic areas, with specific histological features. This can be easily achieved even if you buy a portable ultrasound machine .
Over the past few years, color Doppler sonography has become well established as an integral part of head and neck, ENT and maxillofacial surgery, especially as part of the preoperative evaluation of tumors and cervical lymph nodes.
Color duplex sonography
Color duplex sonography (Box 5) is a combination of B-mode sonography, pulsed Doppler sonography, and color coding of perfusion areas. The basic principle of color duplex sonography is the frequency shift of the transmitted signal, which is caused by reflection from moving red blood cells. The speed and direction in which red blood cells approach and move away from the transducer provide the information needed to perform duplex sonography.
| Box 5 Color duplex sonography
|
The ability to use Doppler signal amplifiers to achieve improved visualization of tumor vascularization has provided new opportunities for tumor characterization. Analysis of microvascularization and time-dependent changes after Doppler amplifier insertion, as well as elastography, are promising new tools for identifying features that help determine whether specific changes are typical for certain types of salivary gland tumors (Fig. 17).
Rice. 17. Study of the salivary glands using power Dopplerography.
The diagnostician should know the following:
|
Stages of salivary gland cancer
After identifying cancer, doctors determine its stage - find out how far the changed cells have spread throughout the body and what tissues have been damaged. Such information is necessary for specialists to understand the patient's approximate prognosis and draw up an individual treatment plan that is best suited in each specific case.
Staging is carried out according to the international TNM system, each letter of which has its own meaning:
- " T
" describes the size of the main tumor and its growth into the tissues closest to it; - using “ N
” indicate the number of lymph nodes affected by cancer; - “ M
” is used to indicate the presence (M1) or absence (M0) of metastases - additional foci of disease in other organs located far from the salivary glands.
Stage 0
, carcinoma in situ: altered cells are present only in the tissue lining the salivary ducts, through which the secretions of the glands exit into the oral cavity.
Stage I
: tumor size does not exceed 2 centimeters.
Stage II
: neoplasm with a diameter of 2 to 4 cm.
Other organs are healthy. Stage III
: the tumor is larger than 4 cm and/or it has managed to damage the soft tissue located next to it;
or a lesion of any size, and its cells have damaged 1 lymph node located on the same side of the head or neck. Stage IV
:
- a neoplasm of any size has grown into the nearest structures - jaw bone, skin, ear canal or facial nerve, and has damaged 1 lymph node, increasing to no more than 3 cm;
- or tumors up to 6 cm in size were found in 1 or more lymph nodes.
IVB stage
:
- 1 or more lymph nodes larger than 6 cm in size have been affected by cancer, or the tumor has spread beyond their limits;
- or the disease has spread to other structures, such as the base of the skull and other nearby bones, or has grown around the carotid artery, a vessel that supplies blood flow to the brain.
IVС stage
: A tumor of any size has created metastases - additional foci of disease in organs or tissues located far from the salivary glands - for example, in the lungs.
Summary
Ultrasonography has established itself as the primary imaging technique in the diagnosis of salivary gland diseases. Sonographic examination is usually sufficient to diagnose sialolithiasis. If chronic sialoadenitis or sialoadenosis is suspected, and sonographic data are insufficient, standard sialography may be required in some cases. A histological examination is necessary as soon as the diagnosis of a neoplasm is established. If the tumor's enlargement and connection with surrounding tissues cannot be determined sonographically, subsequent computed tomography or magnetic resonance imaging should be performed. To conduct research, we recommend using a device from GE Voluson E8 .
Diagnosis of salivary gland cancer
An examination is a very important moment for any patient, since during it doctors do not just detect a disease. They find out how far the altered cells have spread throughout the body, what tissues have been damaged, and what treatment is best for each individual person.
Lapino-2 specialists carry out full diagnostics and any treatment for salivary gland cancer without queues or delays. We have a whole team of professionals with extensive experience in identifying and combating oncology. We carry out all the necessary studies with high quality and analyze their results, and our patients do not have to waste time visiting various medical organizations and retaking tests.
The examination begins with a survey about well-being, symptoms, the time of their onset, as well as risk factors - the presence of relatives with cancer or work in hazardous industries. Then a thorough examination of the mouth, face, neck and jaw is carried out, after which a number of studies are prescribed:
- X-ray
: allows you to see damage to the jaw, teeth and lungs. - Computed tomography
- creates a clear image of internal tissues to assess the size, shape and location of the tumor, as well as search for changed cells in the lymph nodes. - Magnetic resonance imaging, MRI
- obtaining a detailed “picture” of tissue using radio waves and strong magnets. The method helps determine the location and exact dimensions of the tumor, and identify damage to the lymph nodes or other organs. - Positron emission tomography, PET
: used to detect clusters of cancer cells throughout the body. Before the test, a person takes a special substance – radioactive sugar, which accumulates in the altered cells. A PET scan does not create the very clear images of tissue obtained during a CT or MRI, but thanks to it, a specialist can notice all the foci of cancer in the body. This procedure is usually prescribed when there is a suspicion of the presence of metastases - additional tumors in other tissues located far from the salivary glands. - Symptoms and examination results can strongly indicate the presence of a disease, but the actual diagnosis is made only by the results of a biopsy
- the removal of a small amount of altered tissue. As a rule, samples are collected using a thin needle, which is inserted directly into the tumor after preliminary anesthesia. If this method does not produce enough cells, the surgeon makes a small cut with a scalpel and removes a tiny area of the tumor. The material is sent to the laboratory, where a specialist carefully examines the cells and determines whether they are cancerous. Unfortunately, even a biopsy cannot always give a clear answer as to whether a patient has cancer. In such cases, the doctor can perform an operation to completely remove the suspicious lesion and confirm or refute the correctness of his conclusions after the intervention. - Blood, urine
and
stool
: are prescribed not to identify life-threatening neoplasms, but to assess the condition of the patient’s body and the quality of the functioning of its organs.
During a laboratory study, the degree of differentiation of the tumor
– the difference between its cells and healthy ones.
Such data allows specialists to imagine the possible speed of development of a neoplasm and the complexity of its treatment: G1
is highly differentiated: its cells are very similar to healthy ones, they grow slowly and respond well to therapy.
G2
– moderately differentiated: they are noticeably different from normal.
G3
– poorly differentiated: cells do not look like healthy ones, multiply quickly, spread throughout the body and respond poorly to treatment.