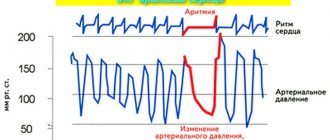
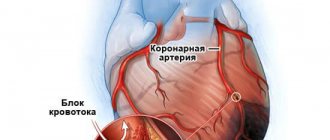
What is a stroke and why is it dangerous?
Stroke is a circulatory disorder in the brain [1]. It can occur due to a ruptured vessel or blockage by a blood clot. In this case, the nerve cells do not receive the required amount of oxygen, glucose and other nutrients, which can lead to their death.
There are several factors that increase the risk of stroke, including: excess weight, high cholesterol, diabetes, hypertension, alcohol and drug use, and smoking. In addition, doctors take into account genetic predisposition and age: the disease most often affects those over 45 years old.
Stroke can be ischemic or hemorrhagic. Subarachnoid hemorrhage is also isolated, which is rare, but in 50% of cases is accompanied by death. He is characterized by acute pain in the back of the head, convulsions, vomiting and loss of consciousness are possible.
Ischemic stroke, or cerebral infarction, is the most common type of cerebrovascular accident. The immediate cause of ischemic stroke is blockage of a vessel supplying the brain. This may occur due to the formation of a blood clot or its entry into the lumen of the vessel. People with atherosclerosis, cardiac arrhythmias, or heart valve disease have an increased risk of developing blood clots. Ischemic stroke can occur when you take medications on your own without a doctor's prescription (for example, diuretics or combined oral contraceptives).
Symptoms of an ischemic stroke develop over a short period of time and are not accompanied by headaches, since there are no pain receptors in the brain. Most often this happens at night when a person is sleeping, and in the morning when waking up he discovers that an arm or leg is not working or speech is impaired.
In a hemorrhagic stroke, the wall of a vessel ruptures and blood permeates the brain tissue. Frequent causes of hemorrhagic stroke are increased blood pressure, taking drugs that reduce blood clotting, disruption of the structure of the vessel wall (aneurysm) or congenital abnormalities of the vascular bed - arteriovenous malformations. Hemorrhagic stroke develops quickly and is often accompanied by headache. If blood soaks into the choroid of the brain, where there are pain receptors, a person may lose consciousness. This subtype of stroke has a high rate of death, but if the person survives, he recovers well.
First aid for stroke
It is advisable that a person with a stroke be taken to hospital as soon as possible - within three hours of the onset of the first symptoms. Therefore, it is important to properly organize assistance for a person with suspected stroke.
- Call an ambulance. If you experience symptoms of a stroke, ask for help and have someone else call the doctor. Provide brief information about the patient (age, what happened). Leave your contact information so we can contact you. Be prepared to meet the physician and provide access to the patient.
- Help the patient find a safe position: it is best to lie on his side with his head slightly elevated.
- While you are waiting for an ambulance, try to find out from the patient when the symptoms began, what chronic diseases does he suffer from and what medications does he take? This information will save doctors time and allow them to quickly make decisions.
- If a person is unconscious and not breathing, cardiopulmonary resuscitation must be performed. However, to properly provide it, it is necessary to undergo specialized training courses [2], [3].
- If the patient has difficulty breathing, remove restrictive clothing (tight collar, tie or scarf) and open the windows.
- If a person is cold, cover him with a warm blanket.
- While the ambulance is traveling, do not under any circumstances try to give the patient something to drink, feed, or force him to stand up. The person may have difficulty swallowing and may choke. And when trying to stand up due to high blood pressure or lack of coordination, there is a high risk of falling and receiving additional injuries.
- Monitor the person closely for any changes in their condition. Be prepared to tell the emergency operator or doctor about their symptoms and when they started. Be sure to indicate whether the person fell or hit their head.
- In some cases, it is advisable to transport the patient to the nearest hospital yourself if you are not confident in the efficiency of the team. Discuss this decision with the emergency operator.
It is good if several people provide assistance. For example, one will be responsible for resuscitation, the second will monitor pulse and blood pressure, and the third will talk on the phone with doctors. Call neighbors and others for help if the sick person is on the street or in a public institution.
Signs and symptoms of stroke
Depending on the severity of the stroke, symptoms may be mild or severe. You need to know what to look for. To check for warning signs of a stroke, you can use the Western mnemonic FAST, which means [4]:
F - face - “face”
A - arm - “hand”
S - speech - “speech”
T - time - “time”
The first symptom is facial asymmetry. If you ask a person to smile, he will not be able to do it; one corner of his mouth will remain downturned. When the patient sticks out his tongue, it may deviate to one side. As soon as you have performed a small operational test, you must immediately call an ambulance. Often the victim does not respond to requests, cannot speak coherently and cannot raise both hands at the same time; sometimes he is in a state of disorientation, the pupils are dilated or there is no reaction to light.
Transient ischemic attack can be difficult to identify based on symptoms alone [5]. They resolve completely within 24 hours and often last less than five minutes. The attack causes temporary circulatory failure and may be followed by a more severe stroke, so it is important to see a doctor as soon as possible.
However, it is worth remembering that only a small part of the brain is responsible for movement and sensitivity, therefore, if blood circulation is disrupted in other parts of the brain, a variety of symptoms may occur: impaired speech, swallowing, vision, dizziness, lack of coordination, confusion and loss of consciousness, epileptic seizures, sudden memory loss or inappropriate behavior of the patient and others. The main task is to call a doctor if someone feels unwell: unusual symptoms appear that were not there before. It’s better to be on the safe side than to miss time, which is the most important factor determining the prognosis for a stroke.
What is a stroke
The essence of a stroke is the cessation of blood supply and functioning of a part of the brain as a result of damage to a vessel.
The larger the affected area, the more severe the stroke. Necrosis of a portion of the brain substance is called an infarction [3]. There is a high risk of death in the first few hours, and then in the period up to 28 days after a vascular accident. The annual mortality rate from stroke in the Russian Federation is 374 cases per 100,000 [10]. In 2018, 35% of patients died in the acute period of stroke; by the end of the first year, this figure increases by 15%, and in general, in the first 5 years, the mortality rate of strokes is 44% [11]. The mortality rate from stroke was 92.9 per 100,000 population, and the hospital mortality rate was 19.1% [5].
Long-term disability is most likely for patients who have suffered a stroke. The prevalence of primary disability due to stroke in 2018 was 3.2 per 10 thousand population [2]. Of these, 31% need constant care, 20% have severe mobility limitations, and only 8% return to work [3]. The prevalence of recurrent strokes in 2014 was 0.79%, of which ischemic
strokes account for 87.5% [9].
Who is at risk
There are people who need to be especially wary of developing a stroke, as they are at risk.
Among them:
- Persons with hypertension.
- Patients with diabetes.
- Men and women over 65 years of age.
- People with abdominal obesity.
- Persons with a hereditary predisposition to vascular pathologies.
- Patients who have previously had a stroke or heart attack.
- Patients with diagnosed atherosclerosis.
- Women over 35 years of age taking oral contraceptives.
- Smokers.
- People suffering from heart rhythm disturbances.
- People with high cholesterol levels.
Most often, patients with the listed diagnoses are registered at the dispensary. Special mention should be made of people living in a state of chronic stress. Emotional stress negatively affects all systems of the body and can cause a stroke.
Causes of stroke
Depending on the cause of cerebrovascular accident, ischemic and hemorrhagic strokes are distinguished.
Ischemic stroke occurs as a result of blockage of cerebral vessels by a blood clot, when gradually less and less blood flows to an area of the brain. Hemorrhagic stroke develops as a result of rupture of a vessel and hemorrhage in the brain tissue, as a result of which the blood supply to its area abruptly stops. Hemorrhage can be into the subarachnoid space (SAS) or directly into the cerebral substance (ICH). The ratio of ischemic and hemorrhagic strokes is 4-5:1 [4].
Pathologically, a stroke can be cardioembolic, lacunar, atherothrombotic, or another, including unknown, etiology (TOAST classification) [10].
Predisposing factors:
- men from 45 to 59 years old;
- age 70 years and older (for both sexes) [4];
- arterial hypertension;
- atrial fibrillation;
- atherosclerosis of cerebral vessels;
- coagulopathy, thrombophilia, anemia;
- arteriovenous malformations;
- osteochondrosis with damage to the vertebral artery;
- brain tumors;
- dyslipoproteinemia;
- obesity;
- diabetes;
- intermittent claudication;
- mechanical prostheses of heart valves and blood vessels;
- IHD, myocardial infarction less than 6 months before the stroke;
- other cardiac diseases;
- smoking, alcoholism;
- family history of stroke;
- sedentary lifestyle;
- stress [1, 3].
The main thing is to see a doctor in time
The doctor who treats strokes is a neurologist. He takes part in the restoration of lost mental and physical functions. The main tasks of a specialist when working with patients who have already been discharged from the hospital are secondary prevention, which is aimed at preventing a recurrent attack, as well as drug treatment of the consequences of the “stroke”.
A modern method for diagnosing pathology is ultrasound duplex scanning of neck vessels. An image of the vessel is formed, its patency and structure are displayed. Diagnostics allows timely detection and prevention of vascular diseases, including stroke.
You need to undergo the study if:
- frequent fainting, headaches, dizziness;
- hypertension;
- arrhythmias;
- elevated cholesterol levels;
- traumatic brain injuries;
- sleep, vision and hearing disorders;
- weakened attention, memory loss.
The necessary studies are prescribed by a neurologist. Based on diagnostic data, treatment is prescribed, which varies depending on the type of stroke.
Our clinic address: St. Petersburg, st. Bolshaya Raznochinnaya, 27 metro station Chkalovskaya
Signs of an incipient stroke
The onset of a hemorrhagic stroke is characterized by the following symptoms:
- severe headache;
- increased blood pressure;
- vomit;
- dizziness;
- loss of consciousness;
- weakness in the limbs;
- visual impairment;
- seizures [1].
The onset of ischemic stroke is gradual; within an hour, some of the following symptoms appear:
- facial asymmetry, numbness;
- difficulty speaking – incoherent, impaired understanding;
- double vision, visual disturbances;
- headache;
- numbness, limited mobility in the limbs, often on one side;
- dizziness, imbalance, staggering, staggering gait;
- confusion with disorientation, subsequently there may be loss of consciousness [3].
If one or more of these signs appear, you should:
- Sit the patient down, providing access to fresh air.
- Call emergency medical help immediately.
- If the patient is conscious and able to chew and swallow, give him one aspirin tablet.
The patient must be hospitalized in a neurological or neurosurgical department, where stroke treatment will be carried out. The sooner the patient is in the hospital, the more effective the therapy.
Precursors of stroke
Symptoms before an attack appear within a few days. However, many do not pay attention to them, because the signs of an impending stroke disappear on their own.
How to recognize the proximity of a “blow”? The most important harbingers:
- headaches that appear suddenly and go away quickly;
- weakness unexpected for a person;
- causeless nausea;
- short-term dizziness;
- frequent mood changes.
You also need to pay attention to symptoms such as:
- visual and hearing impairments;
- slow pulse;
- numbness of the limb;
- flushes of blood to the face;
- disturbance of speech function or coordination of movements;
- severe sweating.
If you have these symptoms, you should immediately consult a doctor, as it is still possible to prevent a stroke.
Within 3 hours from the moment of formation of a brain lesion, acute manifestations of a close “impact” occur:
- difficulty swallowing;
- unbearable headache that leads to fainting;
- severe dizziness;
- vomit;
- convulsions;
- breathing problems;
- tachycardia.
At this stage, the victim requires urgent hospitalization. With timely provision of first aid, the likelihood of severe complications will be reduced.
Symptoms of a stroke
Stroke leads to various brain injuries, depending on the location of the lesion and the pathological type of cerebrovascular accident:
- disturbances of movement in the limbs: from restrictions (paresis) to complete paralysis. When the lesion is localized on the right, the left limbs suffer; with a left-sided lesion, right hemiparesis is formed; in some cases, movements in all limbs may stop (tetraparesis or double hemiparesis);
- sensory disturbances on one or both sides;
- speech disorders (dysarthria - poor articulation; aphasia - inability to pronounce and understand words, write and read);
- ataxia (impaired coordination of movements, “overshooting”, unsteadiness, imbalance, tremor);
- visual impairment: from blindness to double vision and gaze paresis;
- hearing impairment and dizziness;
- violation of mental functions (consciousness, thinking, attention, memory, will, behavior);
- paresis of the soft palate and pharynx, swallowing disorders;
- disorders of urination and defecation;
- depression of respiration and vascular tone;
- increased intracranial pressure;
- patients complain of headaches, vomiting, hiccups, yawning, shoulder pain;
- consciousness is gradually depressed to the point of coma [1, 3].
Causes of death may include cerebral edema, pneumonia, heart failure, and recurrent stroke. In severe cases, “locked-in syndrome” may develop: the patient is conscious, but cannot move, swallow or speak [3].
Content
What is a stroke?
Complications after a stroke
- Paralysis
- Coma
- Brain swelling
- Aphasia
- Loss of coordination
- Apraxia of walking
- Relapse of the disease - why does it happen?
Who can have a stroke? Predisposing factors
- The main distinguishing features of female attacks
- In men
Precursors of stroke
The main thing is to see a doctor in time
Drugs for stroke
Consequences of a stroke
There are transient ischemic attack (less than a day), minor stroke (from 1 day to 3 weeks) and stroke with persistent residual effects. The consequences of a stroke are expressed mainly in motor and sensory disorders, the formation of muscle contractures (pronounced constant restriction of movements in the joints), speech and swallowing disorders. General symptoms may also remain, including confusion, disturbances in thinking, will, and emotional regulation. Complications can develop: from epilepsy to bedsores, encephalopathy and anxiety-depressive syndrome [1, 3].
Classification of strokes
Strokes are classified according to the causes of circulatory disorders and the duration of neurological symptoms. At the Yusupov Hospital, the patient will undergo a diagnostic examination, which will allow the type of stroke and the area of brain damage to be very quickly and accurately determined. When a patient is admitted to the clinic, a number of studies are carried out as prescribed by the doctor:
- MRI – magnetic resonance imaging;
- CT – computed tomography;
- Doppler ultrasound;
- cerebral angiography.
Classification of ischemic stroke (infarction) of the brain:
- hemorheological blockage of cerebral vessels. This condition develops with increased blood clotting and platelet aggregation;
- embolic stroke. Occurs in 20% of cases of ischemic stroke, develops when an artery is blocked by emboli (intravascular substrates) that enter small vessels from larger blood vessels;
- atherothrombotic stroke. Found in 50% of patients with ischemic stroke. A blood clot forms at the site of the atherosclerotic plaque, leading to blockage of the vessel;
- lacunar stroke. Arterial hypertension leads to the development of atherosclerosis, which causes narrowing of small arteries and reduced blood flow to areas of the brain. Occurs in 25% of cases;
- hemodynamic stroke. The pathological condition is caused by a sharp narrowing of a large vessel in the brain due to a drop in blood pressure during heart failure. Blood flow to a part of the brain stops, and an ischemic stroke develops.
Classification of hemorrhagic strokes:
- an outpouring of blood when a vessel ruptures in the brain tissue - parenchymal hemorrhage;
- formation of hematoma in the ventricles of the brain - intraventricular hemorrhage;
- hemorrhage into the cavity between the pia mater and the arachnoid membrane is called subarachnoid;
- Epidural, subdural and mixed forms of hemorrhages are quite rare.
Classification according to the duration of neurological symptoms:
- minor stroke – symptoms manifest from one day to three weeks. Recovery from one day to three weeks;
- transient ischemic attack - symptoms last for about a day, recovery within a day;
- Completed ischemic stroke – symptoms of the disease have been observed for more than three weeks, recovery does not occur for more than three weeks.
Diagnosis of strokes
First of all, it is necessary to conduct a detailed neurological examination. Instrumental diagnostic studies and laboratory tests are also prescribed. In case of a stroke, in the first hours, an MRI or CT scan of the brain is performed, if necessary, CT or MR angiography, color Doppler mapping of blood flow, ECG or Holter monitoring, echocardiography as indicated, monitoring of blood pressure, saturation, assessment of the risk of developing bedsores, assessment of swallowing function [ 1, 3, 6].
Tests for stroke
- Complete clinical blood test, including erythrocyte sedimentation rate (ESR).
- Biochemical blood test with determination of C-reactive protein and homocysteine, glucose level, platelet count, activated partial thromboplastin time, INR.
- Interleukin 10.
- Extended coagulogram.
- Determination of acid-base status.
- General urine analysis.
To prepare for neurosurgical intervention, a blood test is additionally performed for hepatitis, syphilis, HIV, blood group and Rh factor determination.
Diagnostic methods
It is important to quickly distinguish a stroke from other diseases that can lead to the development of similar symptoms. It is almost impossible to do this on your own, as well as to determine the type of vascular accident.
The main difference between an ischemic stroke is a gradual increase in symptoms that do not lead to loss of consciousness. With hemorrhagic hemorrhage, the patient passes out quickly. However, stroke does not always have a classic course. The disease may begin and progress atypically.
Diagnosis begins with examination of the patient. The doctor collects anamnesis and determines the presence of chronic diseases. Most often, you can get information not from the victim himself, but from his relatives. The doctor performs an ECG, determines the heart rate, takes a blood test, and measures blood pressure.
It is possible to make the correct diagnosis and obtain maximum information about the patient’s condition thanks to instrumental diagnostic methods. The best option is a CT scan of the brain. Performing an MRI is difficult because the procedure takes a long time. It takes about an hour. It is impossible to spend this amount of time diagnosing an acute stroke.
Computed tomography allows you to clarify the type of pathology, where it is concentrated, to understand how badly the brain is damaged, whether the ventricles are affected, etc. The main problem is that it is not always possible to perform a CT scan in the shortest possible time. In this case, doctors have to focus on the symptoms of the disease.
To determine the source of the stroke, the method of diffusion-weighted tomography (DWI) is used. The information will be received within a few minutes.
Other examination methods include:
- Lumbar puncture.
- Cerebral angiography.
- Magnetic resonance angiography. It is performed without the introduction of a contrast agent.
- Doppler ultrasound.
Once the diagnosis is made, the doctor will immediately begin treatment.
Stroke treatment
Treatment of stroke is regulated by relevant clinical guidelines and the Procedure for providing medical care to patients with acute cerebrovascular accident. In the first hours, thrombolytic therapy is carried out and subsequently - prevention of thrombus formation. For hemorrhagic stroke, neurosurgery may be performed. They normalize blood pressure, water-electrolyte balance, glucose levels in peripheral blood and urine, support the basic vital functions of the body and prevent complications. Drug therapy is also aimed at improving the affected functions of the nervous system [1, 3, 6].
Types of brain strokes
The most common ischemic stroke (infarction) of the brain - 85% of cases, hemorrhagic stroke occurs in 15% of cases. Strokes can be caused by several reasons:
- formation of thromboembolism in heart diseases;
- acute circulatory disorders in the cervical and large cerebral arteries;
- disturbance of blood circulation in the small arteries of the brain during the acute course of the process.
Stroke rehabilitation
Stroke is a disease in which rehabilitation and care are of the utmost importance.
Recovery from a stroke begins in intensive care, from the moment vital functions are stabilized. A multidisciplinary rehabilitation team works with the patient, which includes a rehabilitation doctor, physical therapist or exercise therapy instructor, speech therapist, massage nurse, physiotherapist and physical therapy nurse, psychologist, occupational therapist, guard and rehabilitation nurse. Diagnosis is carried out using special scales that reflect the degree of dysfunction and limitations in the patient’s activity, the influence of environmental factors on the rehabilitation potential. The rehabilitation process continues throughout the entire period of hospitalization. At the second stage, patients with serious disabilities who are unable to move independently are sent to rehabilitation departments or specialized hospitals. Those who can walk independently or with support are rehabilitated in outpatient centers based in clinics and sanatoriums.
The rehabilitation process should not be interrupted, so classes must be continued at home. Of course, there are no high-tech robotic complexes or physiotherapeutic equipment at home, but exercise therapy, massage, and work with a psychologist, speech therapist and occupational therapist are possible. For this purpose, telemedicine technologies are used and visits to rehabilitation specialists are organized.
The individual rehabilitation program includes not only a referral for rehabilitation treatment, but also technical means of rehabilitation. However, usually relatives also have to devote significant physical and financial resources to achieve the best effect [7].
Ischemic stroke (cerebral infarction) - symptoms and treatment
General events
When treating ischemic stroke, it is customary not to reduce blood pressure quickly if it is high, especially in the first days of the disease.
Low blood pressure should be increased - this is done by doctors; do not give the patient any medications on your own. Uncontrollable, severe vomiting is a common problem in the period immediately after a stroke, especially when the basilar artery is affected. This creates problems in the patient's nutrition. If vomiting does not stop, or there is dysphagia, then a feeding tube is inserted. The lack of electrolytes is compensated for by infusion therapy. The airway should be closely monitored.
Thrombolytic therapy
Thrombolytic therapy is the only therapy for acute ischemic stroke whose effectiveness has been proven in large studies.
No more than 4.5 hours should pass from the onset of the first symptoms of a stroke to the administration of a thrombolytic, so prompt hospitalization is important.
Vascular occlusion occurs in the arterial or venous bed. Thrombotic medications dissolve the clot, but the drug must be delivered to the thrombotic area.
Thrombolytic agents first appeared in the 1940s. The active development of drugs in this group has led to the fact that there are currently five generations of thrombolytics:
- The first thrombolytics are natural substances that convert plasmagen into plasmin, thereby causing active bleeding. These ingredients are isolated from the blood. This group of drugs is rarely used, as severe bleeding is possible. This generation includes: Fibrinolysin, Streptokinase, Urokinase, Streptodecase, Thromboflux.
- The second generation are substances obtained based on the achievements of genetic engineering using bacteria. This generation of drugs has been well studied and has virtually no side effects. Act directly on blood clots. This generation includes: Alteplase, Actilyse, Prourokinase, Gemaz. Purolase, Metalise.
- Third generation - these drugs are able to quickly find a blood clot and act on it for a longer period of time. Most effective in the first three hours: Reteplase, Tenecteplase, Lanoteplase, Antistreplase, Antistreptolase.
- Fourth generation - these drugs are in development and are characterized by a rapid and intense effect on the blood clot. Insufficiently studied.
- The fifth generation is a combination of natural and recombinant active substances.
In the recovery phase, when the patient’s condition almost always improves to one degree or another, speech therapy assistance, as well as occupational therapy and exercise therapy, are important.
Infusion therapy
Anticoagulants (heparin and indirect anticoagulants) are prescribed only when the doctor’s instructions will be followed and it is possible to monitor blood clotting [8].
Anticoagulants
Anticoagulants prevent the formation of fibrin threads and thrombus formation, help stop the growth of already formed blood clots, as well as the effect of endogenous fibrinolytic enzymes on blood clots [11].
Anticoagulant treatment can be started only after intracerebral bleeding has been ruled out.
Direct coagulants : heparin and its derivatives, direct thrombin inhibitors, as well as selective inhibitors of factor X (Stewart-Prower Factor - one of the blood clotting factors).
Indirect anticoagulants:
- Vitamin K antagonists: phenindione (Phenilin), warfarin (Warfarex), acenocoumarol (Sincumar);
- Heparin and its derivatives: heparin, antithrombin III, dalteparin (Fragmin), enoxaparin (Anfibra, hemapaxan, Clexane, Enixum), nadroparin (Fraxiparin), parnaparin (Fluxum), sulodexide (Angioflux, Vessel Due F), bemiparin (Cibor);
- Direct thrombin inhibitors: bivalirudin (Angiox), dabigatran etexilate (Pradaxa);
- Selective factor X inhibitors: apixaban (Eliquis), fondaparinux (Arixtra), rivaroxaban (Xarelto).
Antiplatelet agents
The administration of antiplatelet agents improves the passage of fluid in the brain tissue and prevents the development of acute disruption of the blood supply to the brain [6].
Antiplatelet agents prevent platelets from sticking together, thereby preventing the formation of blood clots.
Classification of antiplatelet agents by mechanism of action:
- aspirin, indobufen, trifluse (stop the action of cyclooxygenase-1, COX-1);
- ticlopidine, clopidogrel, prasugrel, ticagrelor, cangrelor (stop the functioning of the ADP receptor P2Y12 on platelet membranes);
- abciximab, monofram, eptifibatide, tirofiban; xymelofiban, orbofiban, sibrafiban, lotrafiban and others (glycoprotein (GP) Iib/IIIa antagonists);
- dipyridamole and triflusal (cAMP phosphodiesterase inhibitors);
- iloprost (adenylate cyclase enhancer);
- ifetroban, sulotroban and others (suppress the TXA2/PGH2 receptor);
- atopaxar, vorapaxar (antagonize the AR receptor (protease activated receptors) of thrombin).
Aspirin is a commonly used drug in this group. If anticoagulants are contraindicated, then antiplatelet agents can be used.
Surgery
Carotid endarterectomy is a prophylactic surgical procedure performed to remove atherosclerotic plaque from the arteria carotis communis (common carotid artery).
When a cerebellar stroke develops with compression of the brain stem, in order to save the patient’s life, a surgical operation is performed to relieve intracranial pressure in the posterior cranial fossa.
Decongestant therapy
There are different and quite opposite opinions regarding the use of corticosteroids for ischemic stroke, but doctors still actively use them to reduce cerebral edema: they prescribe dexamethasone 10 mg intravenously or intramuscularly, then 4 mg intravenously or intramuscularly every 4-6 hours.
Osmotic agents . Mannitol - increases plasma osmolarity, thereby fluid from tissues, including from the brain, moves into the bloodstream, creating a pronounced diuretic effect, and a large amount of fluid is removed from the body. Cancellation can have a rebound effect.
Anticonvulsants
They must be prescribed for the development of ischemic stroke with epileptic seizures.
Rehabilitation after stroke
Rehabilitation measures begin in the early period of the disease and continue after discharge from the hospital. They include not only drug treatment, massage, physical therapy, speech therapy classes, but also require the involvement of other specialists in psychological, social and labor rehabilitation.
Along with the restoration of impaired functions, rehabilitation includes:
- prevention of post-stroke complications;
- prevention of recurrent strokes.
Basic principles of rehabilitation after stroke:
- early start of rehabilitation measures;
- systematicity and duration, which is possible with a well-organized step-by-step construction of rehabilitation;
- inclusion of specialists of various profiles in the rehabilitation process, individualization of rehabilitation programs;
- active participation in the rehabilitation process of the patient himself, his relatives and friends.
The duration of rehabilitation is determined by the timing of restoration of impaired functions. Recovery of motor functions occurs mainly in the first 6 months after a stroke. During this period, intensive motor rehabilitation is most effective. Rehabilitation treatment for patients with aphasia should be longer and carried out during the first 2-3 years after a stroke.
The complexity of rehabilitation consists of using not one, but several methods aimed at overcoming the defect.
For movement disorders, the rehabilitation complex includes:
- methods of kinesiotherapy (passive and active gymnastics, training in walking and self-care skills);
- correction of motor dysfunction using biofeedback and electrical stimulation using feedback;
- methods of overcoming spasticity and treatment of arthropathy.
For speech disorders, the main thing is regular classes with a specialist in the restoration of speech, reading and writing (speech therapist-aphasiologist or neuropsychologist).
The following model of staged rehabilitation after a stroke is most optimal:
Stage 1 - rehabilitation begins in the angioneurological department (or in the regular neurological department of a clinical hospital), where the patient is delivered by ambulance;
Stage 2 - at the end of the acute period (the first 3-4 weeks), the following options for referring patients are possible:
- 1st option - the patient with complete restoration of impaired functions is discharged for outpatient follow-up treatment or transferred to a sanatorium;
- 2nd option - a patient with a pronounced motor deficit, who by the end of the acute period is still unable to move independently or moves with great difficulty, and needs outside help with self-care, is transferred to the rehabilitation department of the hospital where he was taken by ambulance;
- Option 3 - patients with moderate and mild motor defects, who can move independently within the hospital and provide basic self-care, are transferred to a rehabilitation center. Patients who, during their stay in the rehabilitation department of the hospital (2nd option) have learned to walk independently and simply take care of themselves in everyday life, are also transferred to the rehabilitation center.
Stage 3 - outpatient rehabilitation: rehabilitation in special rehabilitation sanatoriums and at home.
Outpatient rehabilitation is carried out on the basis of rehabilitation departments of clinics or recovery rooms or in the form of a “day hospital” at rehabilitation departments of hospitals and rehabilitation centers. In rehabilitation sanatoriums there can be patients who can fully care for themselves and move independently not only indoors, but also outside. For those patients who cannot independently get to a clinic or day hospital, rehabilitation assistance (classes with a physical therapy methodologist and classes on speech restoration) is provided at home, with the obligatory training of relatives.
Contraindications and limitations to active rehabilitation
The following concomitant diseases limit or prevent active motor rehabilitation:
- frequent attacks of angina pectoris;
- heart failure;
- high and poorly controlled blood pressure;
- chronic pulmonary diseases: bronchial asthma with frequent attacks, obstructive bronchitis;
- severe forms of diabetes mellitus;
- cancer;
- acute inflammatory diseases;
- some diseases and pathologies of the musculoskeletal system: severe arthritis and arthrosis, amputated limbs.
Psychoses and severe cognitive impairment (dementia) are limitations for carrying out not only motor, but also speech rehabilitation.
There are limitations for rehabilitation treatment in conventional rehabilitation centers: extremely limited mobility of patients (lack of independent movement and self-care), impaired control of the functions of the pelvic organs, and impaired swallowing. Rehabilitation of such patients, as well as patients with severe cardiac and pulmonary pathologies, is carried out in rehabilitation departments located on the basis of large clinical multidisciplinary hospitals, according to special rehabilitation programs.
Prevention of strokes
Hereditary predisposition to stroke, the presence of cardiac diseases, pathology of blood vessels and blood composition, age over 40 years, obesity and diabetes require a number of preventive measures:
- Maintaining normal blood pressure, taking antihypertensive drugs as prescribed by a doctor, monitoring blood pressure.
- Maintaining a normal level of physical activity, exercise, walking 30-40 minutes a day (for example, walking the dog).
- Conducting preventive examinations, including a standard set of laboratory parameters. During a preventive examination, the following tests are additionally required: gene diagnosis of CADASIL syndrome using the PCR method, plasma factors of the blood coagulation system, antibodies to prothrombin of the IgG and IgM classes to determine the risk of thrombosis, determination of polymorphisms associated with the risk of arterial hypertension, diabetes mellitus, lipid disorders exchange, in order to identify a predisposition to diseases that increase the risk of stroke, von Willebrand factor (a glycoprotein that ensures the formation of blood clots), complex laboratory tests for preclinical diagnosis of cardiovascular diseases are offered (“ELI-ANKOR-Test-12”, “Cardiorisk”).
- Avoiding chronic and acute stress, maintaining mental hygiene.
- Normalization of weight (BMI <25 kg/m2).
- Healthy eating (for example, Mediterranean diet, limiting salt to 5 5 g/day).
- Quitting smoking and taking psychoactive substances.
- Treatment of diseases that are a risk factor for stroke [8, 11].
Features of stroke in older people
Age is one of the significant factors in the development of acute vascular pathologies of the brain that impair blood circulation. Diseases of the blood vessels in older people are much more severe than in young people. This is due to physiological changes in the body, and in particular in the central nervous system, such as:
- reduction in brain volume and weight;
- thinning of the leptomeningeal membranes;
- senile neuronal atrophy;
- degenerative changes in white matter;
- decreased functional activity of neurons;
- neuronal death caused by electrolyte imbalance;
- reduction of the blood-brain barrier;
- pathological changes in the cerebral ventricles.
About 80% of stroke cases are diagnosed in people over 70 years of age. And, unfortunately, the prognosis for recovery is very often unfavorable. The consequences of stroke in older people are difficult to predict, since it is difficult for such patients to choose effective therapy.
Causes of stroke in older people
Among the causes of stroke in older people, etiological factors and risk factors are distinguished. The former cause the disease itself, while the latter increase the likelihood of pathology occurring. The main causes of acute disorders of blood flow in the brain include:
- arterial hypertension;
- vasculitis and angiopathy;
- improper use of drugs that affect blood clotting;
- neoplasms in the cells of nerve or connective tissues;
- changes in heart rate;
- atherosclerosis of the carotid arteries;
- hormonal imbalance, which increases the risk of blood clots.
The main risk factors for stroke in older people include:
- gender (statistically, men are more susceptible to extensive bleeding into the brain);
- presence of cardiovascular diseases;
- increased cholesterol levels in the blood;
- history of micro-strokes.
As a rule, a stroke is preceded by certain vascular and cardiac diseases. Some of them are systemic atherosclerosis and atrial fibrillation, which develop at the age of 85 years.
Systemic vascular atherosclerosis
This disease is heterogeneous plaques that form in medium and large arteries, including the brain. Elderly and senile age are the main risk factors for the development of atherosclerosis.
Frequent atrial fibrillation after 85 years
Heart rhythm disturbances that lead to an irregular heartbeat indicate the presence of atrial fibrillation. The sinus node cannot cope with the coordination of the heart rhythm, which is why the upper chambers flicker chaotically. As a result, insufficient blood enters the ventricles. The main symptoms of atrial fibrillation are:
- trembling in the chest;
- cardiopalmus;
- irregular heart rhythm;
- dyspnea;
- pain in the chest;
- dizziness;
- fatigue, drowsiness;
- increased anxiety and restlessness.
Many people live with this disease for decades. It is not a direct threat to life, but when a person reaches old age it leads to a number of complications, including stroke.
Stroke in people over 70 years of age
With age, cerebral circulation deteriorates. These disorders are explained by natural aging changes, due to which the body's compensatory reserves decrease. As a result, the walls of blood vessels become brittle, the inner lining of the arteries is affected by atherosclerotic plaques, and cases of sudden jumps in blood pressure become more frequent.
The consequences of a stroke in elderly patients (over 70 years of age) are very life-threatening and radically change it. The first episode of cerebral vessel rupture leads to coma in more than half of the cases. The recovery process after an acute cerebral circulatory disorder is difficult and lengthy.
Signs of stroke in older people
In most cases, the disease manifests itself almost immediately. Deprived of normal blood supply, brain cells die, which is accompanied by the following symptoms:
- severe headache;
- dizziness;
- fainting, short-term loss of consciousness;
- impaired coordination of movements;
- deterioration of speech and pronunciation (slowness, deterioration of diction, inability to reproduce sounds);
- decreased vision, darkening of the eyes, blurred and unclear images;
- confusion, absent-mindedness;
- disorientation in space.
Signs of stroke in older people have some peculiarities. A vascular accident in the brain occurs regardless of the time of day, but more often develops in the early morning or evening. In older patients, the condition often worsens gradually over several days. This is due to the fact that cerebral hemorrhage occurs quite slowly.
Bibliography
- Hemorrhagic stroke in adults: clinical recommendations of the Ministry of Health of the Russian Federation, 2021. Developers: Association of Neurosurgeons of Russia. - Electronic text. - URB: (access date 08/18/2020).
- Efremova M.D. Stroke as an urgent socio-psychological problem / M.D. Efremova – electronic text//Skif. Questions of student science.- 2021 - No. 2(24) URB: (date of access 08/17/2021) Access mode: Cyberleninka electronic library system. — Text: electronic.
- Ischemic stroke and transient ischemic attack in adults: clinical recommendations of the Ministry of Health of the Russian Federation, 2021 developers: All-Russian Society of Neurologists, National Association against Stroke, Association of Neurosurgeons of Russia, Association of Neuroanesthesiologists and Neuroreanimatologists, Union of Rehabilitologists of Russia. - Electronic text. - URB: ( access date 08/18/2020).
- Machinsky P.A. Comparative characteristics of incidence rates of ischemic and hemorrhagic stroke in Russia / P.A. Machinsky, N.A. Plotnikova, V.E. Ulyankin [and others] – Direct text.// News of higher educational institutions. Volga region. Medical Sciences.- 2021.- “2(50)-P.112 – 132 DOI 10.21685/2072-3032-2019-2-11.
- Monitoring the implementation of the federal project “Combating Cardiovascular Diseases” - Presentation Department of Organization of Medical Care and Sanatorium Affairs of the Ministry of Health of the Russian Federation URB: (date of access 08/17/2021).
- Order of the Ministry of Health of the Russian Federation dated November 15, 2012 N 928n “On approval of the Procedure for providing medical care to patients with acute cerebrovascular accidents.” — URB: (access date 08/17/2021) Access mode: Electronic library system “Garant”. — Text: electronic.
- Order of the Ministry of Health of the Russian Federation dated July 31, 2021 No. 788n “On approval of the Procedure for organizing medical rehabilitation of adults.” – URB: (date of access 08.17.2021).- Access mode: Electronic library system “Garant”. — Text: electronic.
- Prevention of cerebrovascular accidents: textbook. manual / Compiled by: L.B. Novikova, A.P. Akopyan. – Ufa: Publishing house of the State Budgetary Educational Institution of Higher Professional Education BSMU of the Ministry of Health of Russia, 2015.-58 p.
- Stakhovskaya L.V. Analysis of epidemiological indicators of recurrent strokes in the regions of the Russian Federation (based on the results of the territorial-population register 2009-2014) / L.V. Stakhovskaya, O.A. Klochikhina, M.D., Bogatyreva, etc.]. CONSILIUM MEDICUM, 2021, vol. 5, no. 9, p. 8-11.
- Shamalov N. A. Analysis of the dynamics of the main types of stroke and pathogenetic variants of ischemic stroke / N. A Shamalov, L. V Stakhovskaya, O. A Klochikhina [and others]. Direct text. // Journal of Neurology and Psychiatry named after. S.S. Korsakov. Special issues. 2019;119(3-2):5-10. doi.org/10.17116/jnevro20191190325.
- 1RRE Electronic edition. Updated daily Stroke Day is celebrated on October 29, 2021 URB: (accessed 08/17/2021).
Author:
Pugonina Tatyana Alekseevna, Therapist
Treatment and rehabilitation
The patient receives treatment in a hospital. All patients with suspected stroke are hospitalized on an emergency basis. The optimal period for providing medical care is the first 3 hours after a brain accident has occurred. The person is placed in the intensive care unit of a neurological hospital. After the acute period has been overcome, he is transferred to the early rehabilitation unit.
Until the diagnosis is established, basic therapy is carried out. The patient’s blood pressure is adjusted, the heart rate is normalized, and the required blood pH level is maintained. To reduce cerebral edema, diuretics and corticosteroids are prescribed. Craniotomy is possible to reduce the degree of compression. If necessary, the patient is connected to an artificial respiration apparatus.
Be sure to direct efforts to eliminate the symptoms of stroke and alleviate the patient’s condition. He is prescribed medications to lower body temperature, anticonvulsants, and antiemetics. Medicines that have a neuroprotective effect are used.
Pathogenetic therapy is based on the type of stroke. In case of ischemic brain damage, it is necessary to restore nutrition to the affected area as quickly as possible. To do this, the patient is prescribed drugs that resolve blood clots. It is possible to remove them mechanically. When thrombolysis fails, the patient is prescribed Acetylsalicylic acid and vasoactive drugs.
In case of a stroke, it is extremely important to provide timely treatment to the damaged areas of the brain. A course of use of the drug accelerates the process of recovery of brain cells after a stroke, even in cases of impaired blood circulation or hypoxia. This allows for rapid restoration of memory, thinking, speech, swallowing reflex and restoration of other functions of daily activities. Gliatilin has a positive effect on the transmission of nerve impulses, protects brain cells from repeated damage, which prevents the risk of recurrent stroke.
The drug is well tolerated by patients; it is contraindicated for use by pregnant, lactating women and people with hypersensitivity to choline alfoscerate.
Courses will need to be taken regularly. You definitely need to do physical therapy, undergo physical therapy, and visit a massage therapist. After a stroke, many patients have to restore motor skills over a long period of time and learn to care for themselves independently.
Relatives and friends should provide support to the patient and not leave him alone with the problem. Psychologists are involved in the work. Sessions with a speech therapist are often required.
Diagnostic methods
It is important to quickly distinguish a stroke from other diseases that can lead to the development of similar symptoms. It is almost impossible to do this on your own, as well as to determine the type of vascular accident.
The main difference between an ischemic stroke is a gradual increase in symptoms that do not lead to loss of consciousness. With hemorrhagic hemorrhage, the patient passes out quickly. However, stroke does not always have a classic course. The disease may begin and progress atypically.
Diagnosis begins with examination of the patient. The doctor collects anamnesis and determines the presence of chronic diseases. Most often, you can get information not from the victim himself, but from his relatives. The doctor performs an ECG, determines the heart rate, takes a blood test, and measures blood pressure.
It is possible to make the correct diagnosis and obtain maximum information about the patient’s condition thanks to instrumental diagnostic methods. The best option is a CT scan of the brain. Performing an MRI is difficult because the procedure takes a long time. It takes about an hour. It is impossible to spend this amount of time diagnosing an acute stroke.
Computed tomography allows you to clarify the type of pathology, where it is concentrated, to understand how badly the brain is damaged, whether the ventricles are affected, etc. The main problem is that it is not always possible to perform a CT scan in the shortest possible time. In this case, doctors have to focus on the symptoms of the disease.
To determine the source of the stroke, the method of diffusion-weighted tomography (DWI) is used. The information will be received within a few minutes.
Other examination methods include:
- Lumbar puncture.
- Cerebral angiography.
- Magnetic resonance angiography. It is performed without the introduction of a contrast agent.
- Doppler ultrasound.
Once the diagnosis is made, the doctor will immediately begin treatment.
Stroke test
There is a test called BE FAST, which is used in medicine to instantly diagnose a stroke attack. The abbreviation has its own meaning:
- B - balance. You need to watch how a person makes movements. Poor balance indicates an impending blow.
- E - eyes. Check the level of visual acuity - have the patient alternately close/open his eyes and tell what he sees in front of him.
- F - face. Ask to smile and stick out your tongue. During an attack, curvature occurs in one direction.
- A - arms. Have the victim raise both arms or shake their palms - one of the limbs will be weaker or will not rise.
- S - speech. Talk to the victim - if there is a lack of cerebral blood supply, speech is impaired.
- T - time. The patient denies the disorder.
If you discover at least one type of deviation, immediately contact the Yusupov Clinic, where experienced doctors will provide primary medical care, establish an accurate diagnosis, and prescribe therapeutic measures. For this purpose, innovative medical technologies of the European level, powerful equipment, and an individual approach are used. You can ask questions and get tested by calling the numbers provided.
Who is at risk
There are people who need to be especially wary of developing a stroke, as they are at risk.
Among them:
- Persons with hypertension.
- Patients with diabetes.
- Men and women over 65 years of age.
- People with abdominal obesity.
- Persons with a hereditary predisposition to vascular pathologies.
- Patients who have previously had a stroke or heart attack.
- Patients with diagnosed atherosclerosis.
- Women over 35 years of age taking oral contraceptives.
- Smokers.
- People suffering from heart rhythm disturbances.
- People with high cholesterol levels.
Most often, patients with the listed diagnoses are registered at the dispensary. Special mention should be made of people living in a state of chronic stress. Emotional stress negatively affects all systems of the body and can cause a stroke.
First aid
If the victim shows one or more of the above signs, then you need to call an ambulance. It is prohibited to give the victim any medications at this time. The man must be laid on a flat surface with his head slightly raised. A cold compress is applied to the back of the head, and a heating pad is applied to the lower extremities. It is important to ensure that the victim is in a state of complete rest, not allowing him to move or stand up abruptly. If a person is indoors, open the windows to allow fresh air to flow in. When vomiting occurs, tilt your head to the sides so that he does not choke. At the first signs of clinical death, artificial respiration and chest compressions are performed.
Possible consequences, complications
The main danger of a stroke is death. If a person survives, the disease will still make itself felt with certain complications.
Early consequences include:
- Brain swelling.
- Coma.
- Pneumonia.
- Paralysis. It can be partial or complete. Most often, one half of the body is affected.
- Repeated stroke.
- Bedsores.
- Mental disorders. They can manifest themselves in moodiness, irritability, aggression, and anxiety. Sometimes dementia develops.
- Sleep disorders.
- Myocardial infarction, gastric ulcer. These disorders develop against the background of increased levels of stress hormones.
After an ischemic stroke, death occurs in 15-25% of cases. Hemorrhagic damage to the blood vessels of the brain leads to the death of 50-60% of patients. The cause of death is precisely severe complications, for example, pneumonia or acute heart failure. The first 3 months after a stroke are considered the most dangerous.
Arms recover worse in patients than legs. A person's future health is determined by the severity of brain damage, the speed of medical care, his age and the presence of chronic diseases.
Long-term consequences include:
- Formation of blood clots in various parts of the body.
- Depression.
- Speech problems.
- Memory loss.
- Deterioration of intellectual abilities.
After a stroke, you have to deal with the consequences for many months. Sometimes a person never manages to fully recover. For rehabilitation to be as successful as possible, you must strictly follow all the doctor’s instructions.
Stroke is a serious pathology because it affects the brain. Therefore, even the slightest suspicion of a developing vascular accident is a reason to urgently seek medical help.