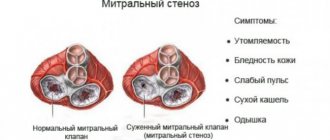
Sudden death
Definition
. Sudden cardiac death (SCD) is defined as: “natural death due to cardiac causes, characterized by sudden loss of consciousness within one hour of the onset of symptoms; the presence of heart disease may be known, but the timing and mechanism of death is unpredictable.” The key concepts guiding the definition of sudden death are that the cause is non-traumatic and that the onset of death is immediate and unpredictable. When considering the problem of sudden death within heart diseases, the word “cardiac” was introduced into the term.
Causes
Epidemiology
. One of the leading causes of death in the adult population of developed countries is SCD due to coronary heart disease. In patients with sudden cardiovascular collapse, the rhythm of ventricular fibrillation is most often determined on the ECG (in 75-80% of cases), while bradyarrhythmias are the cause of SCD in a minimal number of patients. In 5-10% of cases of sudden cardiac death, patients do not have coronary heart disease or congestive heart failure. According to statistical data obtained annually in Western countries, the incidence of SCD varies from 0.6 – 1.28 per 1000 people per year. These studies only include data on those killed or resuscitated by emergency medical services; thus, official data are lower than the actual number of SCD cases in the general population.
Prevention of sudden cardiac death: general population and high-risk group. Among the adult population, the incidence of SCD is 1 in 1000 per year. Prophylactic interventions to reduce the risk of sudden cardiac death in this population appear to be neither practical nor cost-effective, since the costs include the remaining 999 per 1000 people per year who are not at risk for SCD. Thus, general principles of a healthy lifestyle are recommended in the general population.
Subgroups in which the annual risk of sudden cardiac death progressively increases are relatively few. It follows from this that promoting a healthy lifestyle among the population will naturally lead to a decrease in the number of patients with coronary heart disease, which in turn will reduce the number of cases of sudden cardiac death.
What is an implantable defibrillator?
An implantable defibrillator is a device similar to a pacemaker (artificial pacemaker) that has been used since the early 90s. It is small in size - no larger than a pager - and is implanted under the skin of the upper chest. The device contains a battery and a microcomputer necessary to correct your rhythm. An implantable defibrillator is connected to the heart by thin, insulated wires called electrodes. If the device detects that your heart rhythm is abnormal, it sends electrical signals to restore it. Most implantable defibrillators last 5-7 years before needing to be replaced.
Risk factors for sudden cardiac death in the population
| Non-modifiable risk factors | Modifiable risk factors |
| Age | Smoking |
| Male | Hypertension |
| Family history of coronary heart disease | Elevated LDL levels |
| Genetic factors | Diabetes |
| Obesity |
Prevention of SCD: recommendations of the European Society of Cardiology
The European Society of Cardiology Specialist Group on Sudden Cardiac Death presents recommendations aimed at reducing the incidence of SCD. The recommendations are presented in tables and distributed as follows:
Class I:
Reliable evidence and/or consensus among experts that a given procedure or treatment is appropriate, beneficial and effective.
Class II:
Conflicting evidence and/or differences in expert opinion about the benefit/effectiveness of a procedure or treatment.
Class IIa:
evidence and/or expert opinion for benefit/effectiveness predominates.
Class IIb
: Benefit/effectiveness is not well supported by evidence and/or expert opinion.
In these guidelines, the terms “primary” and “secondary” prevention are used primarily in the context of ventricular arrhythmia. Therapy prescribed to prevent the development of sustained ventricular arrhythmias in patients without a history of episodes of life-threatening ventricular arrhythmias, but classified as at high risk for their development, refers to “primary” prevention. The therapy recommended for patients with cardiac arrest and syncope/hypotension secondary to paroxysmal ventricular tachycardia is “secondary” prevention.
Main types of cessation of cardiac activity and mechanisms of their development
The causes of cardiac arrest according to the developmental mechanism are hidden in a sharp violation of its functional abilities, especially excitability, automatism and conductivity. The types of cardiac arrest depend on them. Cardiac activity can stop in two ways:
- asystole (in 5% of patients);
- fibrillation (in 90% of cases).
Asystole is a complete cessation of ventricular contraction in the diastole phase (during relaxation), rarely in systole. An “order” to stop can come to the heart from other organs reflexively, for example, during operations on the gall bladder, stomach, and intestines.
With reflex asystole, the myocardium is not damaged and has fairly good tone.
In this case, the role of the vagus and trigeminal nerves was proven.
Another option is asystole in the background:
- general oxygen deficiency (hypoxia);
- increased carbon dioxide content in the blood;
- shift of acid-base balance towards acidosis;
- altered electrolyte balance (increase in extracellular potassium, decrease in calcium).
These processes taken together negatively affect the properties of the myocardium. The process of depolarization, which is the basis of myocardial contractility, becomes impossible, even if conductivity is not impaired. Myocardial cells lose active myosin, which is necessary to obtain energy in the form of ATP.
With asystole, hypercalcemia is observed in the systole phase.
Cardiac fibrillation is an impaired communication between cardiomyocytes in coordinated actions to ensure overall myocardial contraction. Instead of synchronous work causing systolic contraction and diastole, many separate areas appear that contract on their own.
The contraction frequency reaches 600 per minute and above
In this case, the ejection of blood from the ventricles is affected.
Energy expenditure is significantly higher than normal, and effective reduction does not occur.
If fibrillation affects only the atria, then individual impulses reach the ventricles and blood circulation is maintained at a sufficient level. Attacks of short-term fibrillation can end on their own. But such ventricular tension cannot provide hemodynamics for a long time, energy reserves are depleted and cardiac arrest occurs.
I. Myocardial infarction and heart failure
A. Risk stratification
Both non-invasive and invasive tests are used to determine the risk of SCD in patients with a history of myocardial infarction.
Risk stratification in patients who have had myocardial infarction
with/without development of HF
| Class | I | IIa | IIb |
| Demographic variability LVEF HR or BR sensitivity LV volume | ES unstable VT resting heart rate | Late potentials EPI Dynamics h. T Patency of the infarct-dependent artery |
LVEF – left ventricular ejection fraction; HR – rhythm variability
BR – baroreflex; ES – extrasystole; VT – ventricular tachycardia
HR – heart rate; h. T – T wave
B. Primary and secondary prevention of SCD in patients with a history of MI
Sudden cardiac death occurs most often among patients who have had a myocardial infarction. In this group, primary prevention includes drug treatment with beta blockers, aspirin, ACE inhibitors and cholesterol-lowering drugs. In patients with documented sustained VT or VF, the alternative is an implantable cardioverter-defibrillator (ICD) or amiodarone, and in selected cases, ablation or surgery. In patients with a history of myocardial infarction, a decrease in LVEF less than or equal to 40% (less than or equal to 5%) and clinically symptomatic paroxysms of non-sustained VT, or induced sustained or non-sustained VT by programmed electrical stimulation (EPS), the recommended treatment is CD implantation. For secondary prevention of SCD, the use of CD is recommended for those resuscitated after VF and patients with hemodynamically symptomatic VT paroxysms.
Primary prevention in patients who have had a myocardial infarction with/without the development of HF
| Class | I | IIa | IIb |
| History of MI | Beta blockers ACE inhibitors Cholesterol-lowering drugs Aspirin | Polyunsaturated fatty acids Amiodarone | |
| MI + LV dysfunction | Beta blockers ACE inhibitors Aldosterone receptor blockers | Amiodarone | |
| Hemodynamically asymptomatic VTs | Amiodarone Beta blockers | CD Ablation Surgical treatment | |
| LVEF less than or equal to 40% + paroxysms of non-sustained VT + inducible sustained VT with EPI | KD |
Secondary prevention in patients who have had a myocardial infarction with/without the development of HF
| Class | I | IIa | IIb |
| VF | KD | ||
| Hemodynamically symptomatic sustained VT | KD | Amiodarone Beta blockers |
II. Cardiomyopathies
Hypertrophic cardiomyopathy (HCM)
HCM is a relatively common cardiac disorder (incidence in adults approximately 1:500) in which sudden cardiac death is the most likely outcome at any age, but is most common in young, often asymptomatic patients. Implantation of a CD for the prevention of sudden cardiac death is strongly justified in patients who survive cardiac arrest (secondary prevention). Prophylactic use of KD is also possible in patients with two or more risk factors.
Hypertrophic cardiomyopathy
| Class | I | IIa | IIb |
| Risk stratification | Sustained VT VF | Family history of SCD Syncope LV hypertrophy (VSD greater than cm) Unsustained VT Hypotension during exercise stress test | High risk of mutations |
| Primary prevention | KD | Amiodarone | |
| Secondary prevention | KD |
VSD – thickness of the interventricular septum
Arrhythmogenic right ventricular dysplasia (ARVD)
ARVD is one of the main causes of sudden cardiac death in the “pre-coronary” age group. Although the predisposing factors for SCD have not yet been sufficiently studied in large prospective studies, sudden cardiac death occurs more often in patients with significant changes in the right ventricle, as well as in those with LV involvement. In those resuscitated after SCD (secondary prevention), in patients with sustained VT and ineffective antiarrhythmic therapy, and in high-risk patients with documented paroxysms of VT, the most adequate treatment is CD implantation.
Arrhythmogenic right ventricular dysplasia
| Class | I | IIa | IIb |
| Risk stratification | Sustained VT/VF Dilation of the RV RV dysfunction Inducible VT/VF with EPI | Family history of SCD Late potentials + LV dysfunction VT Inducible VT/VF with EPS | |
| Primary prevention | KD | Antiarrhythmic drugs | |
| Secondary prevention | KD |
RV – right ventricle; EPI – electrophysiological study
Dilated cardiomyopathy (DCM)
SCD is one of the most common mechanisms of death in DCM, especially in the early stages of the disease. Ejection fraction (EF) has been shown to be the most accurate predictor of outcome for both sudden cardiac death and death in advanced HF. The frequency of syncopal episodes is also considered one of the reliable risk factors for sudden cardiac death.
General therapeutic strategies aimed at reducing the risk of SCD in patients with DCM include the use of ACE inhibitors, beta blockers and aldosterone receptor antagonists, while amiodarone and CD implantation are used in individual cases. Several studies examining the role of antiarrhythmic drugs in patients with DCM have provided evidence (not statistically proven) that drug treatment recommended for patients who have had an MI with development of HF is equally effective in patients with DCM. The use of CDs for secondary prevention is considered acceptable; implantation of CDs is also recommended in high-risk patients for the primary prevention of sudden cardiac death.
Dilated cardiomyopathy
Class
| I | IIa | IIb | |
| Risk stratification | Sustained VT VF | Syncopations | Decreased EF Unsustained VT |
| Primary prevention | ACE inhibitors Beta blockers | KD Aldosterone receptor blockers | Amiodarone |
| Secondary prevention | KD ACE inhibitors Beta blockers | Aldosterone receptor blockers | Amiodarone |
What happens during the implantation procedure?
Typically, the implantation procedure is performed quickly, safely, and usually under local anesthesia. It does not require open heart surgery, and most patients return home within 24 hours. The following section is a general description of what happens during the implantation procedure. Your case may be different, you can discuss all the details with your doctor.
During implantation.
Typically, patients are sedated before the procedure and do not feel any pain. Your doctor will make a small incision in your upper chest and place electrodes through a vein into your heart. The doctor will then connect the electrodes to the implantable defibrillator and program the device. Next, an implantable defibrillator will be placed under the skin and the incision will be sutured. The doctor will check to see if the implantable defibrillator is working properly.
After the procedure.
After implantation of the device, the patient usually spends the night in the ward and can return home in the morning. You may feel a small bump under the skin where the device is located; this area may be sensitive. It is usually recommended to limit movement of the arm on the implanted side for 2-6 weeks. You can obtain more detailed care instructions from your doctor. However, you can expect a quick return to your previous activities after surgery. If you have any questions, please ask your doctor or nurse.
Starting life with an implantable defibrillator: the first six weeks.
It's time to start living a full life again. We hope it will be filled with hope and confidence. Of course, until healing occurs, you may experience some discomfort. Also, in order not to cause displacement of the electrodes, you may have to slightly limit the movements of your left hand. Typically these restrictions are recommended for 2-6 weeks. Your doctor will tell you in more detail what movements and strains you should avoid. If you have questions about what you can or cannot do before you recover, don't hesitate to ask your doctor or nurse. Your family and friends will be interested in hearing about your implantable defibrillator. You may want to show the implantation site and talk about the operation. Tell everyone how glad you are to feel recovered from your illness. Now is the time to tell your friends and family about what you are planning to do soon. Choose one of your favorite activities and make plans, think about how you will do it again. Believing in yourself and doing enjoyable, enjoyable things makes a big contribution to the healing process.
Living with Success: Achieving the Confidence You Need.
A new device for your heart will help you feel calm and confident. It is always on alert, constantly taking care of your heart 24 hours a day. If your implantable defibrillator detects a rhythm disorder, it sends an electrical impulse to restore it. You can imagine that this is an ambulance that is always nearby. And very soon you will feel the contribution of these positive effects in your everyday life. Remember that you will still need to continue taking your medications and have your device checked periodically by your cardiologist and electrophysiologist (heart rhythm specialist). Either way, your life is in your hands, so enjoy it. Keep making plans. Tell everyone how good you feel, what you have achieved thanks to this, and what you are going to do. For a high quality of life, identify what you enjoy doing and return to an active lifestyle. Always remember that if you have questions about any special activities, such as driving or returning to work, you should consult your doctor.
What happens after the shock: Have a plan.
If your implantable defibrillator detects an abnormal rhythm in your heart, it will automatically deliver therapy—a high-energy shock. Patients who have undergone such therapy describe this discharge as a sudden feeling of discomfort, sometimes even painful, but quickly passing. It also means that the implantable defibrillator has done its job and may have saved your life. Your doctor will give you specific instructions about what to do after the shock. Together with them, develop an action plan that suits you. This plan may include what you will immediately need to do and some of your favorite activities that you can continue to do after the discharge. Keep the plan in a convenient place so you can refer to it. Also, be sure to tell your loved ones and those who care about you about this plan so that they can understand how to help you. It is important to understand that what you were doing during the discharge did not cause it. Typically, you will be able to continue enjoying your favorite activities. Talk with your doctor about when you can return to your activities and whether any changes need to be made. Although the discharge may make you feel temporarily uneasy, it is important to return to your daily activities and focus on the things you love.
You create your own life.
Life is made up of moments, so the more pleasure we get from them, the more fruitful our life becomes. An implantable defibrillator can help you enjoy life more so you can look forward to the future that means so much to you. These can be simple, “earthly” joys, such as walks in the park, working in the garden, or communicating with your loved ones. The important thing is that these moments often make life richer, so hurry up to enjoy them.
III. Genetic pathology of ion channels
QT prolongation
Long QT syndrome is associated with a high risk of sudden cardiac death. Risk stratification is mainly based on the presence of syncope, Torsades de Pointe (VT) and a history of cardiac arrest. Primary prevention of SCD is generally based on treatment with beta blockers. CD implantation is recommended for secondary prevention, as well as in patients with VT/VF with a history of adequate treatment with beta blockers.
QT prolongation
| Class | I | IIa | IIb |
| Risk stratification | Torsade de pointes/VF/cardiac arrest Syncope Jervell–Lange-Nielsen syndrome QT prolongation | QT greater than 600 ms Development of VT/VF in childhood Prolongation of QT + AV block Macroscopically dynamic T waves Female gender Postpartum period | Family history of SCD Increased QT interval dispersion |
| Primary prevention | Avoid drugs that prolong the QT interval Beta blockers Avoid strenuous exercise | Sympathetic denervation of the LV pacemaker | |
| Secondary prevention | KD + beta blockers + avoid drugs that prolong the QT interval Avoid intense exercise |
ECS - electrical pacemaker
Brugada syndrome
Diagnosis of Brugada syndrome (BS) is based on the presence of spontaneous or inducible ST segment elevation in leads V1-V with or without right bundle branch block (RBBB). Risk stratification is still poorly defined, and the role of EPS in identifying patients with high-risk factors is debated. In survivors of cardiac arrest, CD implantation is recommended. Prophylactic use of KD in high-risk populations is strongly recommended, but this approach is limited by the lack of clearly defined risk criteria.
Brugada syndrome
| Class | I | IIa | IIb |
| Risk stratification | Sustained VT VF | Syncope Family history of SCD | Inducible VT/VF during EPI |
| Primary prevention | CD in patients with syncope/VT | KD in asymptomatic patients with VT induced by EPI | |
| Secondary prevention | KD |
Catecholaminergic polymorphic ventricular tachycardia
To date, there is no precise definition of catecholaminergic polymorphic ventricular tachycardia (CPVT), since large-scale studies are not possible. This disease is associated with a high risk of sudden cardiac death at a young age, but criteria for stratification are lacking. Prevention of sudden cardiac death is based on the use of beta blockers; KDs are recommended for secondary prevention, since the significance of KDs for primary prevention has not been determined.
Catecholaminergic polymorphic ventricular tachycardia
| Class | I | IIa | IIb |
| Risk stratification | VF | Family history of SCD Unsustained VT/syncope in childhood | Syncopations |
| Primary prevention | Beta blockers | KD | |
| Secondary prevention | KD + beta blockers | Beta blockers |
Sudden cardiac arrest associated with early repolarization
METHODS. We reviewed data from 206 patients at 22 centers who were resuscitated from cardiac arrest due to idiopathic ventricular fibrillation and assessed the prevalence of electrocardiographic early repolarization. The latter was defined as an increase in the QRS-ST junction of at least 0.1 mV from baseline in the inferior or lateral lead, manifested as a QRS wander or notch. The control group included 412 patients without heart disease who were matched for age, sex, race, and physical activity level. Follow-up data, which included implantable defibrillator monitoring results, were obtained for all patients.
RESULTS. Early repolarization was more common in subjects with idiopathic ventricular fibrillation than in control subjects (31% vs. 5%, p < 0.001). Among study subjects, those with early repolarization were more likely to be male and have a history of syncope (fainting) or sudden cardiac arrest during sleep than patients without early repolarization. In eight subjects, the origin of ectopia, which initiated ventricular arrhythmias, was located in areas corresponding to the localization of repolarization anomalies. During a mean (±SD) follow-up of 61±50 months, defibrillator monitoring showed a higher rate of recurrent ventricular fibrillation in patients with repolarization abnormality than in patients without such pathology (odds ratio, 2.1, 95% confidence interval, 1. 2 to 3.5, P = 0.008).
CONCLUSIONS. Among patients with a history of idiopathic ventricular fibrillation, there is an increased prevalence of early repolarization.
Sudden cardiac arrest remains . A major public health problem that accounts for approximately 350,000 deaths annually in the United States. Despite advances in emergency medical care, only 3-10% of patients who experience cardiac arrest outside of hospital are successfully resuscitated. Most of these sudden cardiac arrests are caused by ventricular tachyarrhythmias, which occur in 6% to 14% of cases in individuals without structural heart disease. Some of the latter cases are associated with well-recognized electrocardiographic abnormalities that affect ventricular repolarization (eg, long or short QT intervals or Brugada syndrome), while other cases with no signs during sinus rhythm are described as idiopathic ventricular fibrillation. Early repolarization is a common electrocardiographic finding that affects 1 to 5% of people. Although this condition is generally considered benign, its potential arrhythmogenicity has been suggested by experimental studies. However, there is no supporting clinical evidence. We conducted a case-control study of 206 patients with idiopathic ventricular fibrillation to assess the prevalence of early repolarization and assess its potential association with any observed arrhythmias and subsequent outcome monitored by implantable defibrillators.
Methodology.
POPULATION STUDY. Cases of the disease in people under the age of 60 were recorded in 22 territorial centers dealing with arrhythmias. All patients diagnosed with idiopathic ventricular fibrillation in this age group were selected from databases of patients who had received an implantable defibrillator; All patients aged 60 years or older were excluded to minimize the risk of subclinical structural heart disease. Verbal informed consent was obtained from all enrolled patients.
We assessed baseline electrocardiograms for the presence of early repolarization, which was defined as an increase in the QRS-ST junction (J point) in at least two leads during defibrillator implantation. The J-point height amplitude had to be at least 1 mm (0.1 mV) above baseline, either as a QRS blur (a smooth transition from the QRS segment to the ST segment) or a notch (a positive J deflection inscribed on the S wave ) in the inferior lead (II, III and aVF), lateral lead (I, aVL and V4 to V6) or both. Anterior chest leads (V1 to V3) were excluded from the analysis to avoid inclusion of patients with right ventricular dysplasia or Brugada syndrome.
Based on published guidelines, patients were classified as having idiopathic ventricular fibrillation if they had no structural heart disease as demonstrated by normal echocardiographic biventricular dimensions and function, no evidence of ischemic coronary artery disease on coronary angiography or stress testing, and no evidence of any repolarization anomalies. Patients were excluded if they had a heart rate-corrected QT interval (QTc) of less than 340 ms (short QT interval) or more than 440 ms (long QT interval) at baseline and before the arrhythmia. Patients with Brugada syndrome, defined by right branch block and ST segment elevation (>0.2 mV) in precordial leads V1-V3 without intervention or after sodium channel blocker (antiarrhythmic) infusion, were also excluded. In addition, patients with catecholaminergic arrhythmias, defined as arrhythmias during catecholamine infusion or exercise testing, were excluded.
We assessed the prevalence and amplitude of early repolarization in a control group of 412 subjects. This group was composed of health care professionals with normal echocardiographic biventricular dimensions and function and no history of syncope (fainting). The following factors were used for matching (age, gender, race, and physical activity level).
Data collection.
We collected the following clinical data: history of syncope, sudden cardiac arrest, family history of sudden death (age <60 years), physical activity level (>10 hours or ≤10 hours of activity per week), averaged by electrocardiographic signals (both standard amplification and high amplification) and the results of pharmacological testing and invasive electrophysiological testing. Electrocardiographic parameters were measured using automated online software and verified manually. The QTc interval was calculated after heart rate correction using the Bazett formula.
ELECTROPHYSIOLOGICAL STUDY. We performed electrophysiological studies using multielectrode catheters inserted percutaneously through the femoral vessels. Programmed ventricular pacing was performed using a maximum of two or three ventricular extrastimulations from two separate ventricular sites. Ventricular fibrillation was considered inducible if it lasted more than 30 seconds or required electrical cardioversion. No patient had inducible monomorphic ventricular tachycardia.
For subjects with recurrent ventricular fibrillation despite administration of antiarrhythmic drugs, catheter ablation targeting the initiating ventricular ectopy was performed as previously described. Such ectopia was localized by mapping the earliest electrical activity, either Purkinje or myocardial, relative to the onset of the QRS complex. Ablation was performed using radiofrequency energy.
THERAPY AND FOLLOW-UP. All patients with episodes received an implantable defibrillator, which provided accurate information about the recurrence of ventricular fibrillation. Patients were followed regularly every 6–12 months for clinical examination and device testing or, as needed, in the event of symptoms or device battery depletion. In subjects with recurrent arrhythmias, the choice of antiarrhythmic drugs was made by the treating physicians.
STATISTICAL ANALYSIS. Continuous variables were reported as mean ± SD or median (with 25th and 75th percentiles), as appropriate. Comparisons between the two groups were performed with the Student's t test or nonparametric Wilcoxon test, as appropriate, and with the Student t test for paired data. Categorical variables were compared with Fisher's exact test. The prevalence of early repolarization was compared between study subjects and controls using logistic regression analysis (reported as odds ratios with 95% confidence intervals) and adjusted for matching variables. The number of recurrences of ventricular fibrillation was compared using the Wilcokinson test, and the recurrence rate was estimated using actuarial curves. Hazard ratios from Cox proportional hazard models were used to estimate the relative risk associated with early repolarization. All tests were two-sided, and a P value of less than 0.05 was considered statistically significant.
RESULTS.
EARLY REPOLARIZATION.
In the group of patients with idiopathic ventricular fibrillation, there were 123 men and 83 women with a mean age of 36 ± 11 years. The control group included 412 subjects who were matched for age (36 ± 12 years), sex (270 men and 142 women), race (380 whites, 27 Asians, and 5 blacks), and physical activity (44 subjects engaged in more than 10 hours of activity per week ).
Early repolarization occurred in 64 patients (31%) compared with 21 controls (5%, P < 0.001) and was greater in magnitude in study subjects than in control subjects (J-point Height 2.0 ± 0.9 mm vs. 1.2 ± 0.4 mm, P < 0.001). After adjusting for age, sex, race, and physical activity level, the odds ratio for the presence of early repolarization in study subjects compared with control subjects was 10.9 (95% confidence interval [CI], 6.3–18.9).
Cases with early repolarization were more likely to be male, had a history of unexplained syncope or sudden cardiac arrest during sleep, and had a shorter QTc interval than those without early repolarization.
At the initial stage, early repolarization was present in the anterior leads in 28 subjects, in the lateral leads in 6 subjects, and in the inferior and basal leads in 30 patients. This pattern was considered a repolarization rather than a late depolarization because of its slower recording, spontaneous fluctuation in morphologic pattern or amplitude before sustained QRS complexes, and amplitude varying concurrently with the ST segment. The absence of late potentials on high-amplification electrocardiography further supported the repolarization pattern. This pattern occurred in isolation or was accompanied by negative T-wave elevation or discrete ST-segment elevation (horizontal or upward curvature). Electrocardiograms that were obtained several weeks before sudden cardiac arrest were available for 22 subjects and showed a pattern of early repolarization (as described above).
Electrocardiography was performed during the arrhythmic period (including incidence of ventricular ectopy and episodes of ventricular fibrillation) in 18 subjects, all studies showing a consistent increase in early repolarization amplitude compared with baseline. J-point amplitude increased from 2.6 ± 1 mm to 4.1 ± 2 mm (P < 0.001). In most cases, ectopia had a positive QRS morphological pattern in leads V1 to V2, indicating origin from the left ventricle and a short interaction interval initiating ventricular fibrillation (mean, 326 ± 41 ms, range 260 to 400).
Exercise testing or isoproterenol infusion consistently reduced or eliminated early repolarization. Isoproterenol administered to two subjects during repeated episodes of ventricular fibrillation eliminated all arrhythmias when the sinus node heart rate was increased by more than 120 beats per minute. In contrast, beta blockers increased repolarization abnormalities. Their ineffectiveness has led to attempts at catheter ablation of ventricular premature contractions, which resulted in ventricular fibrillation in some subjects.
CORRECTION OF ECTOTIA IN EARLY REPOLLARIZATION. Mapping was performed in eight patients. In two cases, mapping of both ventricles showed no findings during ventricular depolarization that coincided with wide terminal QRS abnormalities, confirming that the latter was associated with repolarization. A total of 26 ectopic patterns were mapped to either ventricular myocardium (16 patterns) or Purkinje tissue (10 patterns). In six patients with early repolarization recorded only in the lower parts, the entire ectopia arose from the lower wall of the ventricle. In two patients with widespread early repolarization, which was recorded by both low and lateral lines, the ectopia arose from multiple regions. Catheter ablation eliminated all ectopia in five subjects and did not eliminate the condition in three subjects.
RELATIONSHIP OF SUBJECTS. Table 2 summarizes results over a mean period of 61 ± 50 months (median, 51 months; interquartile range, 19 to 90) after the initial event, with no subjects losing control. Arrhythmic relapses were more frequent in subjects with early repolarization than in subjects without such repolarization (41% vs. 23%). The hazard ratio for relapse was 2.1 (95% CI, 1.2 to 3.5; P = 0.008), even after adjustment for sex. The three patients with the highest J-point level (>5 mm) had more than 50 episodes of ventricular fibrillation, resulting in death in one case. Quinidine was prescribed to four patients with multiple episodes, which reduced repolarization abnormalities and eliminated recurrent arrhythmias.
DISCUSSION. Sudden cardiac arrest from arrhythmia can occur in individuals who do not have structural heart disease or obvious electrocardiographic abnormalities during sinus rhythm. In our study, such study subjects had a significantly higher prevalence of early repolarization than control subjects, whose prevalence was similar to that of healthy subjects in previously reported studies. In nearly a third of the patients, electrocardiograms obtained before cardiac arrest were available and showed early repolarization, which indicated that this abnormality could not be the result of trauma following sudden cardiac arrest, resuscitation, or the drugs used for resuscitation.
It is unlikely that this anomaly is more common among survivors of cardiac patients than among non-survivors, since the single most important factor determining successful resuscitation is access to rapid defibrillation. This electrocardiographic pattern has also been associated with an increased rate of recurrent ventricular arrhythmias during defibrillator monitoring.
Our results show an association between early repolarization and sudden cardiac arrest, a finding that contradicts the seemingly benign nature of this common phenomenon. First, this finding may be related to the definition of early repolarization, since we specifically included abnormalities in the inferolateral leads, whereas the broad traditional definition of early repolarization included electrocardiographic patterns of varying amplitude, configuration, and extent, most often in the right chest leads. Second, few of the study subjects in our study were from subgroups that have a high prevalence of early repolarization (eg, athletes and blacks), suggesting that cofactors influence the association with sudden cardiac arrest. Third, the beneficial nature of early repolarization is challenged by experimental evidence suggesting that a form of transmural electrical heterogeneity can be dramatically enhanced under certain conditions (use of specific drugs and varying levels of autonomic tone and electrolytes), leading to malignant arrhythmias. Potential arrhythmogenicity thus depends on defective modulation of repolarization, which corresponds to the dynamic changes temporally associated with the arrhythmias that we observed in our case.
The relationship between this electrocardiographic pattern and malignant arrhythmias is supported by increased repolarization before the onset of arrhythmia in study subjects and the occurrence of trigger contractions in the region of early repolarization. Quinidine, which has been shown to restore transmural electrical homogeneity and abolish arrhythmic activity in this condition, reduced the electrocardiographic pattern and eliminated recurrent arrhythmias in four subjects.
Finally, although to our knowledge no multicenter study has examined the association between early repolarization and sudden cardiac arrest, anecdotal reports (mostly from Southeast Asia) have described patients in whom sudden cardiac arrest was associated with abnormal J waves. A repolarization abnormality that is detected in the anterolateral region may be a marker of underlying electrical vulnerability that increases the risk of fatal arrhythmias in the conditions that need to be investigated. These conditions include the presence of genetic defects associated with cardiac ion channels, as evidenced by the fact that 10 of our patients had a family history of sudden cardiac arrest.
These results are potentially important for the evaluation of patients with syncope (fainting) or a family history of sudden death. Arrhythmias associated with repolarization abnormalities may be responsible for a proportion of unexplained deaths, predominantly in young men, as previously reported. Such arrhythmias may also be responsible for some undiagnosed causes of syncope, which have been reported to increase the risk of premature death.
The results of our study, which require confirmation by other researchers, have several limitations. Although the cohort included subjects with well-defined common features, data collection was uneven among centers. In our study population, we did not have subjects with structural heart disease and did not have many athletes or blacks, so the results may not apply to these subgroups. Most importantly, although our results suggest that early repolarization is a marker of malignant arrhythmia disorder, studies predict a favorable course for most of these patients. Further research is needed to identify factors that modulate underlying arrhythmogenicity and predict which patients are at risk.
In conclusion, this multicenter study showed a higher than expected prevalence of early repolarization in patients younger than 60 years of age who had idiopathic ventricular fibrillation that caused syncope and sudden cardiac arrest.
IV. Valve pathology
Aortic stenosis
Among patients whose cause of death is aortic stenosis (AS), about 20% are sudden cardiac death. In the absence of symptoms, the survival rate of patients with AS is high even without valve replacement. The prognostic value of various hemodynamic and electrophysiological studies is limited. Asymptomatic patients with hemodynamically severe aortic stenosis should be under constant observation and, if symptoms develop, undergo immediate surgery. In patients with documented sustained ventricular tachycardia, cardiac implantation should be considered.
Aortic stenosis
| Class | I | IIa | IIb |
| Risk stratification | Syncope Angina | VT, including those induced by EPS Decreased exercise tolerance | Significant stenosis |
| Primary prevention | Surgery | Amiodarone | |
| Secondary prevention | KD |
Mitral valve prolapse
Mitral valve prolapse (MVP) generally has a favorable prognosis; There are suggestions about the risk of sudden cardiac death, but there is no evidence. Most cases of SCD are described in patients who have previously suffered syncope or cardiac arrest, a family history of SCD at a young age, with severe prolapse or myxomatous changes in the mitral valve leaflets. For patients surviving cardiac arrest, CD implantation is recommended.
Mitral valve prolapse
Class
| I | IIa | IIb | |
| Risk stratification | Sustained VT VF | Family history of SCD Severe prolapse or myxomatous changes in the leaflets | QT prolongation Frequent/group ES Inducible VT/VF with EPS Mitral valve regurgitation Late potentials |
| Primary prevention | |||
| Secondary prevention | KD |
Diagnostic signs of cardiac arrest
Cardiac arrest syndrome includes early signs of clinical death. Since this phase is considered reversible with effective resuscitation measures, every adult should know the symptoms, since a few seconds are allotted for reflection:
- Complete loss of consciousness - the victim does not respond to shouting or braking. It is believed that the brain dies 7 minutes after cardiac arrest. This is an average figure, but the time can vary from two to eleven minutes. The brain is the first to suffer from oxygen deficiency; the cessation of metabolism causes cell death. Therefore, there is no time to speculate on how long the victim’s brain will live. The earlier resuscitation is started, the greater the chance of survival.
- Inability to detect pulsation in the carotid artery - this diagnostic sign depends on the practical experience of others. If it is absent, you can try to listen to heartbeats by placing your ear to your bare chest.
- Impaired breathing - accompanied by rare noisy breaths and intervals of up to two minutes.
- “Before our eyes” there is an increase in the change in skin color from pallor to blueness.
- The pupils dilate after 2 minutes of cessation of blood flow, there is no reaction to light (constriction from a bright beam).
- Manifestation of cramps in individual muscle groups.
If an ambulance arrives at the scene of the incident, then asystole can be confirmed by an electrocardiogram.
V. Pathology of the coronary arteries
Anomalous origin of the coronary arteries
SCD most often occurs in patients with an anomalous origin of the trunk of the left coronary artery from the right or non-coronary sinus of Valsalva. Therefore, special attention should be paid to young patients with chest pain similar in description to angina. Surgery is the most appropriate treatment option for patients at high risk of sudden cardiac death.
Anomalous origin of the coronary arteries
| Class | I | IIa | IIb |
| Risk stratification | VF | Young patients with angina or a positive stress test | |
| Primary prevention | Surgery | ||
| Secondary prevention | Surgery |
Myocardial bridges
The long-term prognosis for patients with the presence of myocardial bridges seems favorable, but in some cases this pathology can cause the development of tachyarrhythmias or sudden cardiac death. In symptomatic patients, quantitative coronary angiography, Doppler, and intravascular ultrasound are used to diagnose myocardial bridges. Drug treatment with beta blockers, surgery, angioplasty and coronary artery stenting are alternative treatments.
Myocardial bridges
| Class | I | IIa | IIb |
| Risk stratification | Symptomatic VT VF | Myocardial ischemia | |
| Primary prevention | Surgical treatment in patients with myocardial ischemia | Beta blockers | |
| Secondary prevention | Surgical treatment in patients with myocardial ischemia |
Negative effects of drugs
Medicines that cause cardiac arrest are used for treatment. In rare cases, deliberate overdose causes death. This must be proven to the judicial and investigative authorities. When prescribing medications, the doctor takes into account the patient’s age, weight, diagnosis, and warns about a possible reaction and the need to see a doctor again or call an ambulance.
Overdose occurs when:
- non-compliance with the regime (taking pills and alcohol);
- deliberately increasing the dose (“I forgot to drink this morning, so I’ll take two at once”);
- combination with traditional methods of treatment (St. John's wort, shepherd's ears, self-prepared tinctures of lily of the valley, foxglove, adonis);
- carrying out general anesthesia against the background of continuous medication use.
The use of St. John's wort herb should be very limited; its potency is comparable to antitumor cytostatics
The most common causes of cardiac arrest are:
- sleeping pills from the group of barbiturates;
- narcotic drugs for pain relief;
- groups of β-blockers for hypertension;
- medicines from the group of phenothiazines prescribed by a psychiatrist as a sedative;
- tablets or drops of cardiac glycosides, which are used to treat arrhythmias and decompensated heart failure.
It is estimated that 2% of asystole cases are drug related.
Only a specialist can determine which medications have the most optimal indications and have the least accumulation and addiction properties. You should not do this on the advice of friends or on your own.
VI. Wolff-Parkinson-White syndrome (WPW)
According to modern research, in patients with WPW syndrome, the incidence of sudden cardiac death is 0.15% per year. The main cause of SCD is the transition of atrial fibrillation with a rapid ventricular response to ventricular fibrillation. Survivors of resuscitation for sudden cardiac death are typically characterized by the absence of symptoms, shortened RR intervals (less than 250 ms) during paroxysmal atrial fibrillation, and the presence of multiple or posteroseptal accessory pathways. Electrophysiological study with atrial excitation and determination of RR intervals between preexcited QRS complexes has high sensitivity, but specificity and significance in determining a positive predictor are limited. In patients at high risk for SCD, catheter ablation is recommended, particularly in those resuscitated from ventricular fibrillation or in patients with symptomatic episodes of atrial fibrillation with a rapid ventricular response.
Wolff-Parkinson-White syndrome
| Class | I | IIa | IIb |
| Risk stratification | less than 250 ms cycle duration in AF less than 270 ms anterograde refractory period of additional pathways Multiple additional pathways | Cessation of pre-excitation during treatment with ajmaline | |
| Primary prevention | Ablation for atrial fibrillation and the presence of rapid conduction through accessory pathways | Ablation in asymptomatic patients with – family history of SCD – athletes | Amiodarone Antiarrhythmic drugs classes Ia and Ic |
| Secondary prevention | Ablation |
VII. Bradyarrhythmias
It has been established that bradyarrhythmias are the cause of sudden cardiac death in 15-20% of cases. Risk factors for bradyarrhythmic death include high-degree AV block with intraventricular conduction disturbances, but in the presence of structural changes in the heart, these factors may predispose to the development of tachyarrhythmias. Pacing is the treatment of choice in high-risk patients with bradyarrhythmia: it relieves symptoms and may reduce mortality.
Risk stratification for cardiac conduction disorders
| Class | I | IIa | IIb |
| Profound AV block | AV block III degree AV block II degree, type II Syncope Combination of heart disease with CHF | ||
| Congenital AV block of the third degree | Syncope QT prolongation Congenital heart disease | ||
| Chronic two- or three-fascicle blockade | Combination of heart disease with CHF | Syncope Conduction from the Hiss bundle to the ventricles 100 ms (HV interval 100 ms) Intraventricular blocks Blocks induced during EPI |
What are the consequences of cardiac arrest?
The consequences of circulatory arrest depend on the speed and correctness of emergency care. Long-term oxygen deficiency of organs causes:
- irreversible foci of ischemia in the brain;
- affects the kidneys and liver;
- With vigorous massage in elderly people and children, fractures of the ribs, sternum, and the development of pneumothorax are possible.
The mass of the brain and spinal cord together constitutes only about 3% of the total body mass. And for their full functioning, up to 15% of the total cardiac output is required. Good compensatory capabilities make it possible to preserve the functions of nerve centers when the level of blood circulation decreases to 25% of normal. However, even chest compressions can only maintain 5% of normal blood flow.
Consequences from the brain can be:
- partial or complete memory impairment (the patient forgets about the injury itself, but remembers what happened before it);
- blindness is accompanied by irreversible changes in the visual nuclei, vision is rarely restored;
- paroxysmal spasms in the arms and legs, chewing movements;
- different types of hallucinations (auditory, visual).
Out-of-hospital resuscitation
Survival after cardiac arrest varies from 5% to 60% depending on the characteristics of the cardiac arrest (ie, cardiac etiology or not; verified or not; ventricular fibrillation or not). The outcome of cardiopulmonary resuscitation (CPR) is influenced not only by the success of its implementation, but also by the patient’s condition before the start of CPR.
It is now generally accepted that time to electrical defibrillation is the single most significant determinant of survival after cardiac arrest.
The instructions for the automatic external defibrillator allow defibrillation in cases of out-of-hospital ventricular fibrillation or ventricular tachycardia to people of non-medical professions, often many minutes before the arrival of the ambulance team. This strategy is known in the West as “first responder defibrillation,” based on the principle of mutual aid.
What happens during cardiac arrest
After a few seconds from its beginning, the following develops:
- weakness and dizziness;
- after 10-20 seconds - loss of consciousness;
- after another 15-30 seconds, so-called tonic-clonic convulsions develop, breathing is rare and agonal;
- at 2 minutes clinical death occurs;
- pupils dilate and stop responding to light;
- the skin turns pale or takes on a bluish tint (cyanosis).
The chances of survival are slim. If the patient is lucky and there is a person nearby who can perform chest compressions, the likelihood of surviving sudden cardiac arrest syndrome increases. But for this it is necessary to “start” the heart no later than 5-7 minutes after it stops.