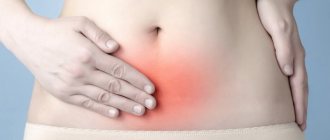
Symptoms of ovarian inflammation
Symptoms of this disease include:
- aching, nagging pain in the lower abdomen that occurs when the body is overcooled, as well as during menstruation;
- pain during sex.
Later, when the disease develops, the above symptoms are also added such as:
- chills;
- frequent urge to urinate;
- a sharp increase in body temperature to 38-39 ° C;
- intense pain radiating to the lower back;
- copious vaginal discharge that appears clear.
In particularly severe cases, nausea and vomiting may also occur. Chronic inflammation of the appendages contributes to increased pain sensations, as well as their range. Therefore, symptoms of adnexitis (inflammation of the ovaries) may include pain in the lower abdomen, groin, sacrum and vagina.
Chronic inflammation can be accompanied by sexual dysfunction, menstrual disorders, miscarriages and the development of ectopic pregnancy.
Classification
Inflammation of the appendages is classified as follows:
| By localization | With the flow | By pathogen type |
| Left-handed | Acute – abrupt onset, severe symptoms. Recovery in a few days | Bacterial – caused by different groups of bacteria |
| Right-handed | Subacute – lasts several days or months | Fungal – the cause is a fungal infection |
| Two-way | Chronic – occurs if acute inflammation is not treated. Characterized by an undulating course, unexpressed symptoms |
Causes of this disease
The infection can enter the body through sexual intercourse (during sexual intercourse from an infected partner). In this case, microorganisms enter the appendages, after which they cause an inflammatory process. This could be chlamydia, gonococci, mycoplasma or trichomonas. Those women who are promiscuous, as well as those who continue sexual activity immediately after childbirth or abortion, are susceptible to such inflammation.
Also, this disease causes the activity of microflora located in the woman’s body or entered into it through non-sexual means (activation of autoinfection). Streptococci, staphylococci, E. coli penetrate the appendages, after which they cause inflammation. As a rule, they cause other types of inflammation, but for some reasons (for example, a general decrease in immunity, the presence of other diseases in the body: dysbacteriosis, sinusitis and even ordinary caries) this microflora can become aggressive.
Prevention
Inflammation of the appendages in its clinical picture and symptoms is similar to many diseases of the genitourinary system, especially of infectious etiology. Therefore, there is no specific prevention; you need to follow some rules:
- treat inflammation without allowing the process to become chronic or develop complications;
- refuse to have sex during menstruation;
- be selective in sexual relationships;
- It is advisable to use a condom during sexual intercourse. This will not only protect you from infection, but also from unwanted pregnancy. Curettage of the uterus is a risk factor. A barrier contraceptive will not prevent infection;
- do not overcool;
- treat colds in a timely manner;
- visit the dentist - microbes in the oral cavity from caries, unhealthy teeth or gums can be a source of infection that enters the genital tract through the bloodstream;
- be physically active to prevent stagnation in the pelvis;
- maintain hygiene regularly;
- do not use other people’s towels or hygiene products;
- do not swim in unfamiliar bodies of water, especially during menstruation;
- strengthen the immune system: harden yourself, make sure that your diet contains enough useful microelements and that your food is fortified. It’s good to take vitamin courses every six months or a year. Only a doctor can prescribe medications. Hypervitaminosis is as dangerous as vitamin deficiency.
If alarming symptoms appear, it is better to immediately get checked by a doctor so as not to start the inflammatory process. Medical examinations cannot be ignored. Once a year you need to undergo a gynecological examination.
Why is this disease dangerous?
Inflammatory processes in the appendages can disrupt the integrity of the epithelium of the fallopian tubes, resulting in adhesions that make the fallopian tubes impassable. And this, in turn, leads to infertility.
Factors that can cause inflammation
These include:
- promiscuous sex life, lack of contraception, frequent change of partners;
- stress, poor and irregular nutrition, overwork;
- hypothermia: in no case should you neglect a hat in severe frost; you should not wear nylon stockings and tights in the cold season;
- using a heating pad when pain occurs: this will only provoke further development of inflammation;
- advanced diseases: sore throat, gastritis, untreated caries, dysbacteriosis.
What to do if symptoms appear? It should be remembered that treatment should only be carried out by an obstetrician-gynecologist.
Sexually transmitted infections (STIs)
STIs are a fairly large group of microorganisms that are mostly conditionally dangerous. In relatively small quantities, they create a certain “ecology” in the vagina, being part of its microflora. This flora also includes microorganisms that act as orderlies. They prevent the reproduction of the above-mentioned opportunistic flora. But in case of decreased immunity, the balance is disturbed and vaginal dysbiosis subsequently develops.
A decrease in immunity occurs in the following cases: during exacerbations of chronic diseases; for acute infectious diseases (for example, influenza, ARVI); after emotional stress or against the background of chronic stress that develops over a long period of time. In addition, a decrease in immunity can occur against the background of a sharp climate change or pregnancy.
All sexually transmitted diseases are characterized by their own distinctive features, but all of them are characterized by a chronic course, as well as minor symptoms. In most cases, women do not notice the disease, and only against the background of a common cold do they notice discomfort in the genital area, increased vaginal discharge, vague periodic nagging pain in the lower abdomen and itching.
Chlamydia
What are chlamydia? These are microorganisms that parasitize the epithelial cells of the patient, destroying them.
Infection occurs during sexual contact, not necessarily genital, but also oral or anal. The incubation period averages 7 – 14 days.
There are no problems with the treatment of chlamydia. Correct selection of an antibacterial drug, its dosage, correctly calculated duration of treatment, as well as the patient’s strict compliance with all doctor’s prescriptions (which is very important) will lead to successful treatment. In most European countries, the USA and Russia, the cost of treatment for chlamydia and other hidden infections is much lower than the cost of diagnosis.
Hidden infections are chlamydia, mycoplasma, ureaplasma and trichomonas. They are always subject to mandatory treatment, and for both partners, even if only one of them gets sick.
Treatment of adnexitis - antibiotics, surgery
The healing process depends on the type of inflammation of the appendages, the patient’s condition and the complications listed above. The basis of treatment for an acute condition is urgent hospitalization and intensive antibacterial therapy. An antibiotic for adnexitis must have a wide spectrum of action. Initially, the drugs are administered intravenously, then administered orally. The gynecologist will also prescribe a diet and apply cold compresses to the abdomen.
Surgery for inflammation of the appendages is used in case of failure of conservative treatment, deterioration of the patient’s condition, or the appearance of symptoms of peritonitis. Antibiotics are also used for chronic and sub-spatial conditions. Only complications of the resulting inflammation of the appendages are operated on. The most dangerous of them is peritonitis, caused, for example, by rupture of an ovarian abscess.
In life-threatening conditions, surgeons use an open surgical method, which consists of a wide incision in the abdominal tissue and cleansing the abdominal cavity of pus. For less serious complications, such as a fallopian tube cyst, laparoscopy may be used.
Treatment of inflammation of the appendages with home remedies is ineffective, and any attempts to use natural methods, including herbs, can only do harm and delay a visit to the gynecologist.
Complications
In men, chlamydia causes inflammation of the epididymis (epididymitis), and in women it causes cervical disease, inflammation of the epididymis, and tubal infertility. During pregnancy, chlamydia can cause serious pathology of the fetus. It also leads to Reiter's disease (severe damage to the eyes and joints).
Monitoring the results of treatment for chlamydia, as well as other hidden STIs, should be carried out no earlier than 3 weeks after stopping medication. Symptoms may persist for several weeks or even months after successful treatment. As for resuming sexual activity, this is possible only after a follow-up examination of two partners.
Ureaplasmosis
Ureaplasmas are very small microorganisms that do not have and do not need their own cell membrane. This feature allows them to penetrate the cells of the host body, so very often they are not visible to the protective cells of the immune system. Consequently, ureaplasma can exist in the human body for more than 10 years. Note that ureaplasmosis is more common among women than among men.
Ureaplasmas received this name because of their ability to break down urea - ureolysis. That is why ureaplasmosis is a urinary infection; without urea, ureaplasma cannot survive. Very often, ureaplasmosis is associated with diseases of the urinary system, chronic cystitis, urethritis and pyelonephritis.
Ureaplasma is usually transmitted sexually, but it is also possible for a child to become infected during childbirth. The incubation period is approximately 1 month. The further development of the disease depends on the body’s immunity, the presence or absence of other vaginal diseases, etc.
In most cases there are no symptoms. Sometimes patients may complain of more abundant discharge than usual, a burning sensation when urinating, discomfort in the genital area and intermittent nagging pain in the lower back and lower abdomen.
Ureaplasma and pregnancy
Ureaplasma can lead to a destructive process in the appendages and uterus, thereby contributing to the development of complications that can lead to pathologies during pregnancy. That is why during this period it is imperative to get tested for this infection, and if it is confirmed, then undergo treatment.
Ureaplasma does not cause malformations in the fetus. In most cases, infection of the baby occurs during childbirth during the passage of the fetus through the infected birth canal. In addition, ureaplasmosis can cause miscarriage, premature birth, threatened miscarriage and endometritis (one of the postpartum complications).
Treatment during pregnancy is most often carried out at 18-20 weeks.
Treatment of ureaplasmosis
Treatment of this disease must be comprehensive and long-term. First of all, antibacterial drugs are prescribed, but taking antibiotics alone is not enough, since ureaplasma can easily adapt to the effects of antibiotics during treatment. Also used in treatment are drugs that increase general and local immunity; antifungal drugs, since antibiotics can cause thrush. The drug complex also includes drugs that can protect the intestines from the effects of antibiotics.
As for the need to treat a partner if he does not have an infection, this is a controversial opinion. This issue must be resolved by the attending physician and the partners themselves.
During pregnancy, the choice of drugs is limited. Only those drugs that are approved during this period can be used. Antibiotics include Vilprafen, Rovamycin, and Erythromycin.
What are appendages
The appendages in women are paired organs of the reproductive system that are located in the lower part of the small pelvis. They include 2 ovaries, fallopian tubes. The latter have an average length of 10 cm and a lumen diameter of 2-4 mm. The fallopian tubes connect the ovarian tissues and the cavity of the reproductive organ - the uterus.
Under conditions of stable functioning of the female reproductive system, the appendages are completely sterile, and their tissues and the surface of the mucous membrane do not contain pathogenic microflora.
In the event of the development of a bacterial imbalance, infection of the genital organs with infectious microorganisms, inflammation increases in the appendages, which reduces or completely stops their functional activity.
Healthy ovaries and fallopian tubes do not cause pain or other discomfort. Disturbances in the functioning of these organs of the reproductive system cause the appearance of painful symptoms.
Gardnerellosis
The disease is not an STD. It is caused by gardnerella vaginalis, and, in fact, gardnerella is a manifestation of vaginal dysbiosis. That is, this is not inflammation in the vagina. That is why this disease is also called bacterial vaginosis.
Unlike other infections, with gardnerellosis the symptoms are pronounced and specific. Symptoms include heavy, thin vaginal discharge that is white or yellowish in color and has a very unpleasant odor, similar to rotten fish. This odor may become stronger during and after menstruation, as well as after sexual intercourse. This disease causes discomfort and burning in the external genital area.
During a gynecological examination, an experienced doctor will be able to immediately make a diagnosis, since the discharge has a slightly foamy characteristic appearance. In some cases, there may be no symptoms, so gardnerella can only be detected during an examination.
Gardnerella is located directly in the vagina. This infection most often does not penetrate further, therefore there are no symptoms such as, for example, pain in the lower abdomen.
Gardnerella and pregnancy
Gardnerella can cause a lot of trouble during pregnancy. It is possible, although very rare, that intrauterine infection may occur. Gardnerella can also cause inflammation of the uterus after childbirth or abortion. That is why bacterial vaginosis during pregnancy must be treated immediately when it is detected.
Gardnerella usually appears in a simple smear on the flora. The PCR diagnostic method is also used to identify them.
Treatment
Treatment is carried out in 2 stages. First, the infection is destroyed, and then the microflora in the vagina is restored.
At the 1st stage, drugs such as flagyl, fasigin, clindamycin, trichopolum are used.
The 2nd stage is longer, it can last 1 month or even more. Here you need to be patient, because... If the microflora is not restored, the disease will return again. Sexual activity during the treatment period is possible, but only if the partners use a condom.
In men, gardnerella “takes root” and does not develop, so treatment of sexual partners is not required.
Diagnostics
With inflammation of the female organs, consult a gynecologist. At the appointment, the patient is asked what is bothering her, her medical history is ascertained, and a gynecological examination is performed. Using a mirror, the doctor detects enlargement, thickening, swelling of the appendages, redness of the mucous membrane, and uneven surface. There is a change in tissue structure, pathological discharge, unpleasant odor, and pain on palpation.
It turns out whether abortions, curettage, or operations were performed. Was there pregnancy and childbirth, method of delivery. How does menstruation happen and how long does it last? Questions are asked about intimate life.
After examination and conversation, a diagnostic complex is prescribed:
- blood biochemistry;
- general urine test;
- PCR testing to exclude STDs;
- a smear from the infected area for bacterial culture to determine the type of microflora so that an effective antibiotic can be selected;
- transvaginal ultrasonography. For pregnant women, ultrasound is performed transabdominally;
- pregnancy test. In some cases, ectopic pregnancy may have symptoms similar to inflammation of the appendages.
If a tuberculous form of adnexitis is suspected, menstrual blood is taken for bacterial culture and a Pirquet or Mantoux test is performed.
For differential diagnosis of inflammation of the appendages or in case of an unclear diagnosis, the following can be performed:
- hysterosalpingography - X-ray contrast examination of the fallopian tubes and uterus;
- colposcopy – a detailed examination of the uterine cavity using a colposcope (binocular with a lighting device);
- hysteroscopy – the uterus and appendages are examined using a hysteroscope. As with colposcopy, biopsy material can be taken;
- Laparoscopy – allows you to simultaneously examine organs and perform surgical procedures.
A biopsy is needed to exclude atypical cell degeneration and assess the risk of neoplasms. MRI and computed tomography with contrast can be performed.
Human papillomavirus
Recently, this infection has received the attention of most researchers, as well as practitioners. This is due to the fact that the ability of this infection to cause cancer of the genital organs in both women and men has been proven.
Human papillomavirus infection, like many other STDs, very often occurs without symptoms, thereby contributing to its even greater spread in the human body. Not all cases of HPV cause cancer, but almost every case of cancer is caused by HPV.
Currently, more than 120 types of HPV have been identified, 34 of which affect the genitals, as well as the perineal area. Moreover, each virus is responsible only for its own “area”.
How does a person become infected with this virus?
HPV can be transmitted during direct contact of mucous membranes and skin when:
- traditional sexual intercourse (the main route of transmission of infection);
- non-traditional sexual intercourse (anal or homosexual sex). It is also believed that HPV transmission is possible through oral-genital contact;
- during childbirth during the passage of the fetus through the infected genital tract of the mother;
- The household route of transmission is also possible: through hands, bath accessories, dirty clothes.
Factors that provoke the development of HPV
These factors include:
- promiscuity, early sexual activity, a large number of partners;
- repeated abortions;
- the presence of other STDs (chlamydia, ureaplasma, mycoplasma);
- smoking;
- chronic diseases of the genital organs (inflammation of the uterus, appendages, vagina);
- anal sex;
- aggravated medical history (cervical cancer in close relatives).
The incubation period ranges from 1 to 8 months. People aged 17-26 years are most often susceptible to HPV infection, which is associated with increased sexual activity at this age. But this does not mean that older people cannot be infected.
Sometimes there are cases that the virus leaves the body on its own, without treatment. This happens most often in young people over 30 years old. If the virus enters the body after 35 years, then the likelihood that it will leave the body on its own is, unfortunately, small.
Forms of infection
This infection can occur in 3 forms:
- Latent form. It is asymptomatic. In this case, there are no changes or abnormalities, but the infected partner can transmit the infection through sexual contact.
- Subclinical form. Patients may have the following symptoms: vaginal discharge, a feeling of discomfort and dryness in the external genital area, which intensifies after sexual intercourse, itching, burning. At the same time, an ordinary gynecological examination will not reveal changes in the genital area. They can only be detected through a detailed examination (for example, colposcopy).
- Clinical form. Finally, the most common symptom of HPV is condylomas. This is a type of wart that is located on the mucous membrane of the genital organs, namely: at the entrance to the vagina, in the area of the clitoris, anus, urethra, and on the walls of the vagina. Occasionally they can be found on the skin of the perineum and labia.
Condylomas are skin growths that resemble a cockscomb in appearance. They can be on a stem or on a base. The color of condylomas is no different from the color of the surrounding tissues.
HPV is detected using the PCR diagnostic method.
Treatment
Condylomas are removed chemically (using various medications), using a laser, and also by cryodestruction. Then treatment is carried out aimed at increasing the body's immunity. In this case, vaginal and rectal suppositories are prescribed for local immunity and various drugs that stimulate general immunity - tablets or intramuscular injection.
It is also necessary to screen your partner for this disease. Sexual intercourse during treatment is possible only with the use of a condom.
Functions
In women, the appendages are located in the pelvic area and belong to the internal reproductive organs. Without their presence, stable functioning of the body, maintaining a constant level of female sex hormones, conception and birth of a child is impossible. The main function of the ovaries is to synthesize steroid hormones.
The follicular part of the appendages produces the main female hormone - estrogen, as well as progestins and androgens in much smaller quantities.
The corpus luteum of the appendages, which in its physiological structure is a temporary gland with a secretory function, acts only in the luteal phase of the menstrual cycle. The function of this element of the appendages is to produce progestin, but the corpus luteum also synthesizes estrogens and androgens in small quantities.
The functional activity of the ovaries is a cyclical process. During the maturation period, one of the follicles acquires the properties of a dominant one and slows down the development of the others. An egg develops inside the dominant follicle, which can eventually be fertilized by a sperm.
When the maturation process of the follicle is completely completed, its shell is destroyed, and then an egg is released into the abdominal cavity. This is a function of ovulation, which is carried out with the direct participation of the appendages. The released egg is fixed by fimbriae and, together with the flow of fluid, the direction of which is created by the synchronous movements of the fallopian tube, enters its cavity.
Then the egg migrates through the appendage of the reproductive system - the fallopian tube - into the inside of the uterus. If in the period 3 days before ovulation a woman has had unprotected sexual intercourse and a sufficient number of viable sperm with a sufficient level of motility has entered the vagina and uterine cavity, then there is a high probability of fertilization of the egg.
This is another function of the appendages associated with the process of conceiving a child. Thus, the main functions of the female appendages in the form of ovaries and fallopian tubes are to ensure stable synthesis of sex hormones, participate in the process of maturation of the egg, and transport it to the cavity of the reproductive organ.
Stable functional activity of the appendages ensures the preservation of the health of the female reproductive system, and also maintains the balance of sex hormones.
Why Central Clinical Hospital RAS
Even for a regular preventive examination, it is better to go to a highly qualified, experienced gynecologist. And when health problems arise, this becomes especially relevant. The hospital's excellent equipment with equipment from leading global manufacturers allows the cause of the disease to be quickly and accurately determined. It has its own clinical diagnostic laboratory - you don’t have to wait long for tests, and most of them are ready on the day of your visit.
But the most important thing is that doctors who are in love with their profession work here. Many of them have an academic degree - these are C.M.N., professors, doctors of the highest category. Gynecology is one of the most important medical areas of the Central Clinical Hospital of the Russian Academy of Sciences. All specialists constantly improve their skills and use the latest achievements of researchers in various fields. In complex and controversial cases, the question of prescribing the necessary treatment is decided by the council.
A warm, friendly atmosphere, affordable prices, convenient registration by phone or online are pleasant additional advantages. In addition, you can always be sure that at the Central Clinical Hospital of the Russian Academy of Sciences you are welcome and ready to help in the most difficult situation.