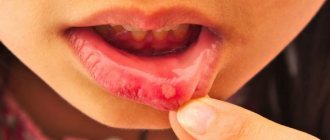
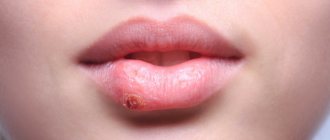
The yeast-like fungus of the genus Candida is always present in the human body, but under certain factors it begins to multiply faster. The consequence of this process can be inflammation. Unpleasant white spots and plaque form on the tongue and oral mucosa - the main manifestation of candidal stomatitis.
Infants are often susceptible to the disease, as their immune system has not yet fully developed. It can appear from the first weeks of life. Moreover, it occurs in children under 10 years of age and in older people, especially if they suffer from dry mouth.
Cause of candidal stomatitis
We have already said above that the main reason is the increase in the concentration of Candida fungus in the body. Let us emphasize once again that normally in the human body, including the oral cavity, these microorganisms are always present and do not cause harm.
We can distinguish two groups of factors that provoke this process: endogenous (internal) and exogenous (external).
Endogenous (internal) factors:
- metabolic disorders, gastrointestinal problems, diabetes and other diseases;
- lack of vitamins;
- acute and chronic infectious and non-infectious general diseases;
- weakened immune system;
- long-term treatment with antibiotics.
Among the exogenous (external) causes: various damage to the mucous membrane (for example, due to dentures), thermal or chemical burns, poor personal hygiene.
Causes of candidal stomatitis
The most common cause of candidiasis stomatitis is a fungus of the Candida albicans group. It is worth noting that these fungi are always present on the mucous membranes of the mouth, and do not cause any harm to the body until they begin to multiply.
The causes of the development of candidal stomatitis are the following factors and diseases:
- Weak immunity;
- People with Sjögren's syndrome;
- Neglect of general rules of oral hygiene;
- Constant stress;
- Various diseases of the oral cavity;
- Taking antibiotics or corticosteroids;
- Having a disease such as diabetes. This is all due to the fact that the blood contains a large amount of sugar, and this serves as an excellent environment for the development of fungus of the genus Candida.
It is also worth noting that adults who suffer from excessive dry mouth can get candidal stomatitis. The most common cause of such dryness is the abuse of dental elixirs.
Another factor that can cause the development of candidal stomatitis is pregnancy. After all, it’s no secret that it is during this period that significant hormonal changes occur in a woman’s body, which, in turn, greatly affect the bacterial balance in the mouth.
Types of disease
Pseudomembranous. One of the most common types, which has several forms. To a mild extent, a white coating appears on the mucous membranes of the cheeks and tongue. In the middle, it becomes denser and begins to grow into the mucous membrane, erosion and bleeding appear, and regional lymph nodes enlarge. In severe form, weakness appears, body temperature rises, ulcers form under a white coating, and local lymph nodes enlarge.
Atrophic. It can develop independently or after the pseudomembranous form. Its manifestation is dry mouth, burning or pain when eating, and spots form on the surface of the tongue. The mucous membrane turns red, swells, and tongue movements become limited. Inflammation begins in the corners of the mouth.
Chronic. Candidomycosis stomatitis develops into this form if treatment is not carried out at the initial stage. In this case, changes begin in the mucous membrane (thinning, drying, redness), it becomes difficult to swallow, and a burning sensation is felt in the mouth. If left untreated, there is a risk of damage to the larynx, esophagus and intestines.
It can also be classified by location: candidal stomatitis of the corners of the mouth, yeast glossitis (appears on the surface of the tongue), thrush (plaque covers the mucous membrane of the cheeks and gums).
Who's at risk
First of all, these are people who have the following unfavorable factors:
- Weakened immunity.
Defects in immune defense are the main factor predisposing to the occurrence of mycoses (fungal infections)1,2,4. The increase in their incidence in all countries of the world is due, first of all, to various types of conditions accompanied by weakened immunity1,[3]. It is not for nothing that “thrush” is called “the disease of the sick”1. Among its reasons:
- severe general diseases, for example, infectious2,3;
- cancer accompanied by sudden weight loss, lack of vitamins and microelements, requiring radiation and chemotherapy2,3;
- congenital and acquired forms of immunodeficiency, including AIDS2,3;
- endocrine disorders, for example, diabetes mellitus2,3.
- Dental diseases.
- Inflammatory , such as caries and its complications, gingivitis, periodontitis, periodontal disease and others2. The huge number of bacteria present during inflammation weakens the immune system and contributes to the proliferation of fungal microflora2. A diseased tooth with a carious cavity “infested” with microbes or a periodontal pocket filled with pus may well provoke the development of “thrush”3,[4].
- Non-inflammatory , which change the structure of the oral mucosa, for example, folded tongue and leukoplakia4. It is easier for fungi to attach to a damaged surface than to a healthy one.
- Constant dry mouth.
- Insufficient saliva (xerostomia), associated with a variety of problems, contributes to the development of oral mycosis4. Saliva contains many enzymes and antibodies that protect the mucous membrane from the action of microbes4. If there is little saliva, it dries out, its protection is weakened, which creates favorable conditions for the development of other infections.
- Defects in oral hygiene.
- Insufficient care . Problems more often arise in those who rarely brush their teeth and ignore the care of their tongue, interdental spaces and dentures4.
- Injuries . Sometimes the cause of an “outbreak” of oral mycosis is a too hard toothbrush or rough manipulation of dental floss and toothpicks. Injured gums are easy prey for fungi2.3,4.
- Incorrect use of removable dentures.
- Poorly customized removable dentures can rub the gums3,4, making them accessible to germs.
- No night break in using prostheses4. The gum located under the prosthesis is poorly enriched with blood, it lacks oxygen, it is not washed with saliva - this predisposes to the development of infection4.
- Improper care of dentures. Artificial teeth need care just as much as your own. Deprived of attention, they become covered with a thin film of various microbes, which then “attack” the gums.
- Age.
- Most often, doctors find “ thrush” in the mouth of infants and the elderly4. The reason for this is the imperfections of the immune system, which create favorable conditions for the proliferation of pathogenic microflora1,4,[5]. In addition, in childhood, dietary habits affect, and in old age – constant dry mouth and lack of teeth, forcing you to wear dentures1,5.
- Medicines
- Antibiotics. They kill not only pathogenic microbes, but also beneficial ones, thereby disturbing the balance of microflora and creating conditions for mycoses to flourish1,2.
- Drugs that inhibit cell proliferation (cytostatics). They interfere with the renewal of surface mucosal cells and disrupt local and general defense mechanisms against infections1,2.
- Immunosuppressive medications, which are prescribed when immune responses need to be suppressed, such as during transplantation1,2.
- Inhaled corticosteroids, which are used in the treatment of bronchial asthma and, due to their side effects, increase the susceptibility of the mucous membrane to infections2,[6].
- Unbalanced diet
- Lack of iron, vitamins C and B12, and folic acid1 in the diet, which leads to decreased immunity.
- Excess carbohydrates1,2. Excessive consumption of sweets, flour products, sweet fruits, starchy vegetables and other foods containing large amounts of simple carbohydrates contributes to the appearance of thrush in adults and children1,2.
Up to contents
Symptoms of candidal stomatitis
Clinical manifestations of oral candidiasis are varied. As a rule, a milky-white cheesy coating forms on the back of the tongue, palate, and cheeks. When it is removed, the eroded bleeding surface of the mucous membrane is exposed, and painful sensations appear when swallowing. A common symptom is dry mouth and an unpleasant metallic taste.
In the earliest stages, a small number of white spots form. As the disease progresses, their number increases and they turn into ulcers. In severe forms, the white plaque cannot be removed and it completely covers the oral cavity.
If left untreated, the fungus can invade the area of the larynx, esophagus and even the intestines. The pain intensifies and the red border of the lips and corners are affected. When the lips are affected, candidal cheilitis begins to develop, due to which cracks and erosions form, thin films and crusts grow. Seizures may also appear in the corners of the mouth, which bleed and cause pain when opened.
Symptoms
A number of symptoms are characteristic of candidal stomatitis:
- The appearance of a white or yellowish coating on the tongue, cheeks or palate. When trying to eliminate it, bleeding wounds may appear on the mucous membrane.
- Constant metallic taste.
- Feeling of heartburn on the tongue.
- Painful sensations from touching plaque.
- Later, as plaque spreads, difficulty swallowing occurs.
- Deterioration of tongue sensitivity and poor taste perception.
Diagnosis of the disease
Before starting treatment for stomatitis, you should consult a dentist. The doctor will listen to complaints, conduct a visual examination of the oral cavity and skin, and also take scrapings from the affected areas. In some cases, consultation with a therapist, dermatologist, allergist and endocrinologist may be required.
Remember that timely diagnosis is the key to successful treatment and easy progression of the disease. Also, regardless of the causes and form of the disease, treatment in newborns should be carried out under the supervision of doctors.
Clinical researches
Repeated clinical studies have proven that the two-component mouth rinse ASEPTA ACTIVE more effectively combats the causes of inflammation and bleeding compared to single-component rinses - it reduces inflammation by 41% and reduces bleeding gums by 43%.
Sources:
- The role of anti-inflammatory rinse in the treatment of periodontal diseases (L.Yu. Orekhova, A.A. Leontyev, S.B. Ulitovsky) L.Yu. OREKHOVA, Doctor of Medical Sciences, Prof., Head of Department; A.A. LEONTIEV, dentist; S.B. ULITOVSKY, Doctor of Medical Sciences, Prof. Department of Therapeutic Dentistry of St. Petersburg State Medical University named after. acad. I. P. Pavlova
- The use of adhesive balm "Asepta®" in the treatment of inflammatory periodontal diseases L.Yu. OREKHOVA*, Dr. med. Sciences, Professor, Head of Department V.V. CHPP**, Dr. med. Sciences, Professor, Head of Department S.B. ULITOVSKY*, Dr. med. Sciences, Professor A.A. LEONTIEV*, dentist A.A. DOMORAD**, O.M. YAKOVLEV** SPbSMU named after. acad. I.P. Pavlova, St. Petersburg - *Department of Therapeutic Dentistry, **Department of Microbiology
- https://cyberleninka.ru/article/v/puti-sovershenstvovaniya-pervichnoy-profilaktiki-zabolevaniy-parodonta Acute herpetic stomatitis in children, Baranaeva E.A. Merkulova E.P. magazine "Medicine and Healthcare"
- https://cyberleninka.ru/article/v/osobennosti-protivoretsidivnogo-lecheniya-allergicheskogo-stomatita Acute stomatitis in children, Drobotko L.N., Strakhova S.Yu.
Treatment of candidal stomatitis
The course of treatment depends on the type and severity. Often the complex includes local and general methods:
- rinsing with antiseptic, antimycotic and analgesic drugs;
- use of antifungal ointments, aerosols, gels;
- when it spreads to other body systems, systemic antimycotics are prescribed.
With properly selected therapy, its duration is two weeks. If stomatitis has become chronic, then courses of treatment must be repeated to avoid relapses. In the most advanced cases, this is from 1 to 3 months.
With a mild degree of the disease, candidiasis can be eliminated forever. In other cases, there is a possibility of relapses, and even the development of candidal sepsis, so prevention is of great importance.
Features of “thrush” in the mouth in children of the first year of life
Mycoses in children, and very young ones at that, are not that uncommon. According to statistics, the first illness of a newborn in 33% of cases is associated with Candida fungi5. Moreover, they mainly affect the skin and tissues of the oral cavity5.
Why does thrush appear in the mouth of a child under one year old?
Mycotic stomatitis, or fungal inflammation of the oral mucosa, is the most common form of mycosis in children under one year of age1.5. How do mushrooms get into a baby’s mouth and why do they take root there? There are many reasons for this.
- Infection during childbirth.
During childbirth, the fetus comes into contact with the microflora of the woman’s vagina. If the mother suffered from vaginal candidiasis before giving birth and did not undergo the necessary course of treatment, the baby has every chance of inheriting a large amount of the causative agent of this disease1.5, which is a big burden for the immature immune system. According to statistics, on the first day of life, Candida fungi are found in the oral stool of 25-40% of newborns5.
- Unsanitary conditions.
Infection is possible due to violation of the rules of care for the newborn and defects in the hygiene of the nursing mother herself1,5. The infection is transmitted through dirty nipples and hands during feeding, through toys, nipples, dishes and linen.
- Imperfect immunity1, 5.
In a baby under one year old, the immune system is only “gaining experience”, because in the womb it did not come into contact with the infection and therefore “did not learn” to fight it.
- Prematurity and illness.
Candida can only harm a weakened body. The best conditions for their development are created if the birth occurs before term, the fetus is premature and/or has developmental defects or congenital diseases5.
- Nutritional features.
The threat is posed by regurgitation, the habit of putting the baby to bed with a bottle of milk and feeding with sweet artificial formulas. If milk remains in the mouth, which also contains a large amount of sugar, it becomes an ideal breeding ground for mushrooms.
- Features of salivation.
Due to physiological characteristics, the salivary glands of infants produce little saliva1 - they simply do not need it, since food is already liquid. At the same time, saliva has antifungal activity, and when there is little of it, the likelihood of oral thrush in a newborn increases1,5.
What does oral candidiasis look like in children?
The symptoms are the same as in adults: first, white “grains” appear on the mucous membrane, then “clumps” resembling curdled milk, and white films1. The difference is that the process is almost always accompanied by severe tissue swelling and the formation of numerous painful ulcers on the oral mucosa and tongue1,5. Therefore, due to oral thrush, infants often refuse to eat5.
In children, a fungal infection can affect not only the tonsils (tonsillitis), but also the pharynx (pharyngitis) and larynx (laryngitis). If the larynx is affected, the baby's voice becomes hoarse and low, and there is a risk of swelling of the airways and breathing problems1, 5.
Up to contents
Prevention
To prevent the manifestation of candidal stomatitis, you must adhere to the following rules:
- learn to brush your teeth so as not to injure the mucous membrane;
- use mouth rinses to cleanse the mouth;
- change your toothbrush every 2 months and rinse thoroughly after use;
- if you wear a denture, you must wash it thoroughly using special products, and also follow the storage rules;
- get rid of bad habits;
- if you are taking antibiotics, you must use antifungal drugs and probiotics as prescribed by your doctor;
- wash and treat with boiling water accessories that small children come into contact with;
- Nursing mothers are advised to maintain breast hygiene;
- hardening, physical education in the fresh air;
- visit the dentist regularly.
Treatment
First of all, when treating candidal stomatitis, you need to determine and eliminate the cause, adhere to the principles of proper nutrition and strengthen the body's immune system. And, of course, it is necessary to monitor oral hygiene. In most cases, this is quite enough for recovery.
If the disease is in a moderate or severe stage, the doctor often prescribes special medications for oral administration and antifungal ointments. Taking medications continues until the symptoms in the oral cavity are completely eliminated, in order to exclude possible relapses.
Treatment of mild forms of candidal stomatitis is carried out at home and does not require special conditions. Antifungal elixirs and lozenges are used. On average, the treatment course takes no more than two weeks.
More severe forms are characterized by the fact that the infection enters the digestive tract. Antifungal drugs are used to combat the disease. The course of treatment lasts from 2 to 4 weeks.
Recurrent forms of candidal stomatitis require much more time and money. Treatment is carried out until all symptoms disappear completely. Various antifungal agents are used.
Treatment of candidal stomatitis must be combined with a special diet. First of all, you should stop eating foods that are rich in starch and various confectionery products, minimize the consumption of cereals, baked goods, potatoes, etc.
When treating candidal stomatitis, other concomitant diseases should be eliminated, in particular:
- Caries;
- Periodontal disease;
- Chronic diseases of internal organs.
Diagnosis of oral mycosis
Most often the diagnosis is obvious. However, in difficult situations, for example, in the presence of complications or individual intolerance to certain drugs, to confirm it, microscopic and cultural analysis of scrapings from the surface of the mucous membrane is used to determine the sensitivity of the microflora to antifungal drugs. Moreover, the mere presence of Candida threads in scrapings from the oral cavity is not always enough to make a diagnosis - fungi can be present in the mouth, but not cause any diseases. In such a situation, quantitative assessment is important, that is, counting the pathogen cells, and increasing their number when re-analyzed after 2-3 days.
Up to contents
Types of stomatitis
Stomatitis comes in different forms: it depends on the causative agent of the disease. So, it can have a viral, microbial or mycotic etiology. Accordingly, the symptoms, description and principles of treatment of the disease will be different.
Aphthous stomatitis: treatment
The exact reasons why this type of stomatitis occurs have not yet been established. Some experts consider staphylococci and adenoviruses to be the source of ulcers, while others attribute the disease to a viral disease. Some doctors equate aphthous stomatitis with herpetic stomatitis, with the only difference being that in the first case, instead of ulcers, aphthae appear - round white or yellow plaques with a red frame. Aphthae are concentrated on the cheeks, lips, and tongue.
The disease occurs against a background of decreased immunity and can transform into an ulcerative-necrotic form.
Treatment of aphthous stomatitis in adults is as follows:
1. Local treatment, including treatment of aphthae and rinsing the oral cavity with disinfectants and antiphlogistic agents, such as hydrogen peroxide (diluted 1:1 with water), furatsilin tablet, boric acid, sea buckthorn oil.
2. Drug therapy aimed at detoxification and desensitization.
3. Vitamin therapy.
4. Use of sedatives and antihistamines.
5. Physiotherapy.
6. Diet, which consists of excluding spicy, allergenic and rough foods from the diet.
Aphthous stomatitis in adults often occurs against the background of exacerbation of pathologies of the nervous, endocrine systems and diseases of the gastrointestinal system. Therefore, its prevention will be the treatment of concomitant diseases.
Since aphthous stomatitis is often caused by staphylococcus, a pathogen that multiplies in dental plaque and teeth affected by caries, a thorough improvement of the oral cavity is necessary. With surgical dental treatment and removal of dental plaque, the problem of aphthous stomatitis in adults is minimized.
Herpetic stomatitis: symptoms
Herpetic or herpes stomatitis is the most common form of manifestation of the disease. Almost 90% of the adult population are carriers of the herpes virus, which in itself does not cause any discomfort. But with a decrease in immunity, exacerbation of chronic pathologies or trauma to the oral cavity, it can intensify and manifest itself in the form of herpetic stomatitis.
This type of stomatitis most often affects the cheeks, tongue, and palate. The clinical description of the oral cavity will be as follows: the mucous membrane becomes swollen and red. Against this background, small rashes appear.
The disease lasts about ten days, during which the adult usually does not experience any acute reaction to the appearance of ulcers. Body temperature remains normal, no symptoms of intoxication are observed, and the person feels relatively well. In case of reduced immunity or in a child, general intoxication, malaise and high fever are possible.
Discomfort is caused only by the process occurring in the mouth, consisting of:
• formation of bubbles;
• merging them into a group;
• bursting of ulcers and the formation of painful erosion (it hurts a person to drink, eat, talk).
The disease is also often accompanied by enlarged lymph nodes.
Sometimes herpetic stomatitis can develop into gingivitis, characterized by sharp redness of the gums around the teeth. Also, with gingivitis, rashes can affect the red border of the lips. Treatment for gingivitis is problematic, so it is better to prevent herpes from developing into gingivitis.
Treatment of stomatitis consists of taking medicinal anti-inflammatory, anesthetic and antiviral drugs. It should be remembered that herpes is not sensitive to conventional disinfecting infusions, so herbs and chlorhexidine are not a help here.
Local treatment and vitamin therapy also help. It should also be borne in mind that this form of the disease is contagious, therefore, during the period of illness, close contacts associated with kissing, drinking from the same cup, etc. should be limited. This especially applies to people whose disease has progressed to gingivitis.
Candidal stomatitis: treatment
This is already a fungal manifestation of a disease that is characteristic only of people with a very weakened immune system, suffering from chronic diseases or taking steroid hormones.
The causative agent of the disease is the Candida fungus, which is always present in the oral cavity. Its reproduction and manifestation in the form of a cheesy coating and white spots begins only in the presence of provoking factors.
The treatment regimen for stomatitis in adults consists of the following measures:
• taking antifungal medications;
• treatment of lesions with antifungal gels and ointments;
• if you have dentures, treat them with antiseptic solutions;
• rinsing the mouth;
• exclusion of easily digestible carbohydrates from food;
• visiting a gastroenterologist and endocrinologist, since the disease is often caused by pathologies characteristic of these medical areas.
Catarrhal stomatitis: causes of occurrence
This is the mildest and most common form of stomatitis. Often this is where other types of disease begin. With timely rinsing of the mouth, the disease will subside within a couple of days. Otherwise, it may develop into a more severe form. The patient only has to follow one simple rule: you need to rinse your mouth for at least a minute.
Externally, the disease looks like a light coating on the mucous membrane and is accompanied by slight swelling and redness. You may also experience bad breath, increased salivation, and a severe burning sensation in the mouth.
The main reason why catarrhal stomatitis occurs is oral candidiasis, which occurs against the background of a general inhibition of the body's defenses. The causes of the disease also include:
• inadequate oral care;
• diseases in the gastrointestinal tract of a chronic nature;
• damage to the body by worms;
• dental problems – untreated caries, periodontitis, dental plaque.
Regular visits to the dentist will help eliminate the problem of the development of catarrhal stomatitis and its transition to another form of the disease.
Allergic stomatitis
Allergic stomatitis in adults is not an autonomous disease: it can accompany any allergic reaction in a person. Particularly susceptible to illness are individuals who react with allergies to food or medications when there is direct contact of the allergen with the oral mucosa. People also often react to dentures with allergic stomatitis.
Allergic stomatitis comes in several types:
• viral;
• bacterial.
It depends on the causative agent of the infection. Often, due to allergies, aphthous stomatitis can occur, which is called aphthous allergic stomatitis.
Signs of stomatitis are manifested by the appearance of white spots or small blisters in the mouth. The mucous membrane turns slightly red and becomes covered with pinpoint hemorrhages. The person may experience pain, burning, severe itching, or dry mouth.
Treatment of stomatitis comes down to taking medicinal antihistamines and eliminating the main cause of the allergy.
Prosthetic stomatitis: causes
Prosthetic stomatitis in adults manifests itself in two types: allergic and bacterial. In both cases, the clinical picture is manifested by a sharp reddening of the mucous membrane of the prosthetic bed. And with the allergic type, redness also occurs in all areas of the mucous membrane that are in one way or another in contact with plastic.
The causes of prosthetic stomatitis depend on its type:
1. Allergic
This is a common allergic reaction to dentures. The main reason for this is the monomer included in the structure of acrylic plastic, which is used in the manufacture of prostheses. Also, the reason for the body’s reaction to dentures may not be the competence of the dental technician, who committed a violation in the selection of the proportion of components in the manufacture of plastic.
Replacing a low-quality prosthesis can solve the problem.
2. Bacterial
In this case, the “owner” of the prostheses himself becomes the culprit of the disease. It must be remembered that removable dentures require the same care as teeth. They must be constantly cleaned after eating. Otherwise, pathogenic elements may form on the surface of the product, which, in addition to the proliferation of bacteria, become a source of unpleasant odor.
Therapy for denture stomatitis consists of disinfecting rinsing of the oral cavity and treating the inner surface of the denture and the mucous membrane underneath it. It is enough to apply a small layer of antiseptic to relieve the painful condition.
Vincent's ulcerative necrotizing stomatitis
The main difference between ulcerative stomatitis is the presence of large, small-sized ulcers in the oral cavity coupled with the death (necrosis) of gum tissue. The disease is quite rare and may be a consequence of untreated catarrhal stomatitis.
Favor the development of Vincent's stomatitis:
• bacterial growth due to poor oral hygiene;
• weakened immunity;
• smoking;
• previous viral diseases.
The cause of the disease is often gastric ulcers and various poisonings.
The development of pathology occurs according to the following scheme:
1. Changes in the oral cavity
The patient notices dryness of the mucous membrane, bleeding gums, the appearance of ulcers on the hills between the teeth, which are later covered with plaque. Inflammation affects the inside of the cheeks, palate, and tongue, making eating and talking painful.
2. General health
The disease is accompanied by fever, weakness, and loss of appetite. The lymph nodes may become enlarged and tender to the touch.
To treat ulcerative stomatitis, the help of a specialist is necessary. Under anesthesia, he will remove dead tissue, bacterial plaque and tartar. Otherwise, you can get exposure of the roots of the teeth and massive necrosis of the gums.
Further therapy consists of the use of antibiotics and antihistamines, disinfectant rinsing and local treatment of the mucous membrane. If necessary, antipyretic and painkillers help. A course of vitamins also has a therapeutic effect.
Stomatitis acute and chronic
Stomatitis in adults differs not only in the form of manifestation. There are also differences in the nature of the disease. So, it can be acute and chronic. The first is characterized by the following description:
• swelling and hyperemia of the mucous membrane;
• formation of ulcers, erosions and plaque.
Stomatitis transforms into a chronic form if it becomes acute. And if a person’s immunity is weak, then the causative agent of the disease remains in the oral cavity constantly even after treatment. As a result, inflammation takes on a chronic form, characterized by a sluggish course with relapses.
The most common chronic form of the disease is characteristic of herpetic stomatitis. The herpes virus, even despite complete recovery, continues to constantly remain in the nerve endings of cells and is activated at the slightest weakening of the immune system.
Microbial carious stomatitis
There is another type of major stomatitis, which is an accompanying disease and manifests itself during the development of infectious diseases - microbial carious stomatitis. The origin of the disease in this case may be related to:
1. With any dental problems that are a source of infectious processes
Tartar, caries, dental plaque - all this is a place where carious bacteria - streptococci and staphylococci - are concentrated. At the slightest trauma to the mucous membrane, carious infection leads to the development of stomatitis.
2. With scarlet fever or sore throat
Scarlet fever is accompanied by a strong white coating on the tongue, which after a few days is replaced by a bare, bright red surface of the mucous membrane. In this case, they also talk about bacterial microbial stomatitis. A white coating on the tongue also accompanies a purulent sore throat. In the case of stomatitis, inflammation spreads not only to the mucous membrane and throat, but also to the gums, which look reddened, swell and hurt.
Therapy for microbial carious stomatitis consists of antiseptic rinsing and diet.
How to get rid of stomatitis?
Stomatitis is perhaps the most common and unpleasant disease of the oral cavity. When an infection enters the body, ulcers form in the mouth. They cause discomfort and can subsequently lead to serious complications. How to treat stomatitis ?
Treatment of any infectious diseases first of all involves going to the doctor. Antibacterial therapy should be carried out under medical supervision. Bacterial disease most often goes away in 1-2 weeks. If the stage is not advanced, it can be treated independently. How to treat stomatitis at home :
- Rinse your mouth with soda solution. Add 1 spoon of soda to a glass of warm water. You can also use boric acid (1 teaspoon per 150 ml of water) or hydrogen peroxide (1 teaspoon per half a glass of water).
- Chamomile decoction. Heals wounds quickly.
- Sea buckthorn oil has an antibacterial effect. You can use antiseptics: chlorhexidine or miramistin.
- Anesthetic dental gels will help relieve severe pain. They should contain lidocaine.
Soda solution can also be used to treat stomatitis in infants .
Wipe the mouth and tongue with moistened gauze. If signs of stomatitis (bacterial) do not disappear, you should consult a doctor.
In case of aphthous form of the disease, you should urgently go to the clinic. How to determine:
- multiple large and deep ulcers;
- grayish coating in the center;
- red rim around the wound.
This type of stomatitis should not be treated at home. It is forbidden to cauterize ulcers with alcohol, iodine, or brilliant green. An advanced disease can lead to suppuration and tissue death.
How to get rid of stomatitis in children?
Basic methods of local therapy:
- Treating the oral cavity with baking soda. For preparation you will need 1 tablespoon per glass of boiled water. Apply 3-6 times a day.
- Rinse with Blue solution. Or 2% boric acid.
- Use of antifungal agents. This includes medicated creams and ointments. For example, Clotrimazole, Pimafucin, Nystatin, Candide.
Symptoms of stomatitis in children and treatment can be determined by a doctor. Treatment is carried out in accordance with the doctor's prescriptions. If the dosage is not followed correctly or the course is interrupted, side effects may occur.
You should not self-medicate, as this can harm the baby.
Only a pediatric dentist will prescribe the correct therapy. He can also advise treating stomatitis in children at home .
Types of stomatitis
Depending on the depth of tissue damage and the cause of inflammation, experts distinguish the following types of stomatitis:
- catarrhal;
- aphthous;
- candida;
- ulcerative;
- herpetic;
- traumatic;
- allergic.
The catarrhal form of stomatitis is the mildest and rarely causes complications. But treatment is still required, mainly local. The most severe course is ulcerative necrotizing stomatitis, which often causes bacterial complications.
The candida type occurs more often in young children.
Each type of disease has its own characteristics, causes of development and symptoms. It is difficult to determine the shape yourself.
Sometimes even specialists do not have enough clinical picture to make an accurate diagnosis. Additional laboratory tests are often required to determine why stomatitis occurs in the mouth and whether it is associated with other diseases.
Diagnosis of the disease
The pathology of stomatitis is diagnosed by infectious disease specialists, pediatricians, and pediatric dentists. The diagnosis is made on the basis of clinical and epidemiological data.
Based on materials from smears, scrapings, and blood, the following studies are carried out:
- virological;
- bacteriological;
- immunological;
- cytological.
Diagnostics such as polymerase chain reaction and enzyme immunoassay are performed. In some cases, the child has a blood test for the presence of sugar, and a consultation with an endocrinologist, allergist and other specialists is carried out.
Correctly conducted diagnostic examinations will help establish the correct diagnosis and prescribe effective treatment so that the situation does not worsen.
Prevention of stomatitis in children
Irritative stomatitis can be prevented with good oral hygiene, regular dental check-ups and proper nutrition. Because many adults and children carry the herpes virus and can transmit it even without symptoms, there is no practical way to prevent herpetic stomatitis. However, parents may discourage their child from kissing, eating, or playing in close contact with people who have an active herpes infection.
Ulcers can be minimized by teaching children to avoid injury, even minor trauma to the mouth. If our doctor determines that a child has a nutritional deficiency, parents can make sure the child is taking appropriate supplements and eating recommended foods. It won’t hurt to visit the dentist once every six months if we have previously discovered stomatitis in the child. Regular visits to our clinic will help prevent serious complications and detect the disease in time.