Uterine pathology is a group of gynecological diseases, many of which reduce the patient’s quality of life, impair fertility, and provoke recurrent miscarriage.
Some diseases of the uterus can be congenital, others are acquired throughout life due to infections, dyshormonal disorders or other reasons.
Make an appointment
Bicornuate uterus and pregnancy
The formation of a bicornuate uterus during pregnancy can be triggered by various infectious diseases that the expectant mother can become infected with within 9 months, these include:
- measles;
- rubella;
- syphilis;
- flu;
- toxoplasmosis (in rare cases).
In addition, diseases of the endocrine system such as diabetes mellitus, thyrotoxicosis, as well as various heart diseases (congenital or acquired) can cause the development of a bicornuate uterus in a newborn baby.
A bicornuate uterus during pregnancy can also appear if the fetus receives insufficient oxygen. Fetal hypoxia during pregnancy can also have irreversible consequences in the future when a female child is born.
Pathological changes in the urinary system of a pregnant woman are also risk factors for the development of a bicornuate uterus.
Causes
The defect is formed in the fetus during embryonic development under the influence of various factors:
- intoxications of various kinds (alcohol, drugs, nicotine, chemicals);
- vitamin deficiency in a pregnant woman;
- stress, traumatic situations;
- endocrine disorders in the mother (thyroid disease, diabetes mellitus);
- heart defects;
- infectious effects, especially dangerous for a pregnant woman are influenza viruses, pallidum spirochete, which causes syphilis, rubella and measles pathogens and other infectious agents;
- irradiation;
- poor nutrition.
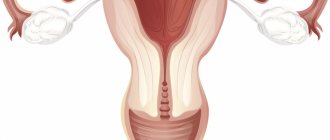
Often a bicornuate uterus is combined with other anomalies in the structure of the reproductive organs or the genitourinary system. The internal genital organs of the fetus are formed from the Müllerian canal, a paired organ that forms at 7-9 weeks of intrauterine development. In case of embryogenesis disorders, the Müllerian ducts are not completely connected, as a result of which one complete uterine cavity is not formed, and the cavity is divided into two niches. This happens around 10-14 weeks. With incomplete fusion of the Müllerian canals, two cervixes and an incomplete vaginal septum may form. Two horns can represent two full-fledged uterine cavities, or one horn is rudimentary (incipient state).
Formation of the uterus during embryonic development
Symptoms of a bicornuate uterus
Symptoms of the division of the uterus into two horns may not appear until the woman finds out about pregnancy. The outcome of the first pregnancy with a bicornuate uterus most often ends in spontaneous miscarriage or death of the embryo inside the womb. This occurs due to the woman’s ignorance of the specific anatomical structure of the uterus, as well as as a consequence of the careless attitude of specialists and improper examination of the patient.
The difficulties of a bicornuate uterus during pregnancy lie in the constant oxygen starvation of the fetus due to the pressure of one horn on the cavity of the other. The embryo develops in the area of one uterus. But there is not enough space for a comfortable stay in the womb, normal blood circulation and oxygen production. These circumstances can cause pregnancy loss. The period of maximum risk of possible embryo death is associated with the first trimester: at the stage of intrauterine formation of all vital organs.
The risk of premature birth or the presence of pathologies in the child with a diagnosis of “bicornuate uterus” may include the following signs:
- the position of the fetus before birth is transverse or oblique - indicators for cesarean section;
- breech presentation of the fetus;
- low placement of the fetus long before delivery;
- uterine bleeding;
- partial/complete placental abruption with bleeding;
- the presence of bleeding in the uterus after intimacy.
Classification
Uterine cleft occurs:
- complete - pronounced separation, can be at different angles, starts from the uterosacral ligaments. As a result of complete separation, two separate cavities are formed with a close location. A normal pregnancy in one of the cavities is possible;
- incomplete - splitting begins from the upper third of the organ, in which a shallow niche is formed between the horns of almost the same size;
- saddle-shaped - a saddle-shaped depression is formed at the bottom of the uterus. Conception is possible, but with combined defects, pregnancy will most likely end in spontaneous miscarriage. Independent childbirth is most often impossible.
The shape and severity depend on the area of the splitting, as well as accompanying abnormalities.
Cleavage can be complete or incomplete
Diagnosis of a bicornuate uterus
In order to find out what a bicornuate uterus is in women and whether you have it, you need to undergo a series of gynecological examinations. Signs by which the presence of a bicornuate uterus can be determined are the following complaints to the doctor:
- frequent miscarriages;
- uterine bleeding;
- heavy discharge during menstruation accompanied by severe pain;
- inability to get pregnant.
Medical diagnosis of the uterus will consist of a number of studies:
- vaginal ultrasound of the pelvis;
- external ultrasound;
- laparoscopy;
- MRI diagnostics;
- hysterosalpingography.
When diagnosing the division of the uterus into two horns, it is necessary to conduct additional research to determine the presence of just such a diagnosis, and not an intrauterine septum. Bicornus is quite often confused with the latter.
1.General information
A bifurcated uterus, or bicornuate (two-humped) uterus, saddle uterus is a relatively rare variant of malformation, i.e. incorrect, abnormal development of a key organ of the female reproductive system. The uterine “sac,” which is normally solid and symmetrical, in the case of bicornus, takes the form of a double wide anastomosis of the fallopian tubes, which merge into a single cavity only in the lower sections, closer to the cervical canal (cervix). Sometimes the bicornuate uterus is accompanied by doubling of the cervical canal, abnormalities of the vaginal septum, and asymmetry of the “horns.” The limiting case can be considered uterus didelphys - the presence of two anatomically separate uteruses, each with its own canal, and in some cases with a bifurcation of the vagina.
A bifid uterus occurs, according to various estimates, with a frequency of 1 to 5 cases per 1,000 women.
Sign up for a consultation
A must read! Help with treatment and hospitalization!
Treatment of bicornuate uterus
Treatment of bicornus can only be prescribed by a doctor, based on medical indicators. The main factor determining the need for an operation to eliminate uterine pathology is a woman’s constant miscarriages (at least 2-3 spontaneous abortions or death of the fetus inside the womb). These surgical interventions are aimed at changing the uterine area; the end result should be the formation of a single cavity.
Strassmann's operation is a surgical procedure that is performed to change the uterine cavity and remove the orifices. The operation involves correction through laparotomy, where the uterus is cut and the external parts of the orifices are connected. After surgery, it is necessary to install an intrauterine device for at least six months.
Forecasts
With a bicornuate uterus, a woman can bear a child without complications if the volume of the cavity and blood supply are sufficient for the full development of the fetus. The more pronounced the splitting of the uterine cavity, the higher the likelihood of infertility, spontaneous termination of pregnancy, premature birth, and bleeding. During pregnancy, there is often an incorrect location of the placenta, presentation, and premature detachment. The method of delivery is determined individually, taking into account the severity of the defect, complications, concomitant diseases, age, and additional factors. The threat of miscarriage in the third trimester is an indication for cesarean section.
If the embryo attaches to the rudimentary horn, then the pregnancy becomes ectopic, which leads to rupture of the rudimentary horn and intra-abdominal bleeding. Full pregnancy, childbirth, and menstrual cycles are possible with well-developed and blood-supplied horns. It is very rare that pregnancy develops in both horns at the same time.
The likelihood of spontaneous abortion is reduced by 30-90% after surgical treatment.
If, after correction, the uterine cavity has not acquired a volume sufficient to bear a child, then they resort to assisted reproductive technologies, in particular, surrogacy. In patients with bicornus, pregnancy management is aimed primarily at preventing miscarriage and bleeding. To minimize the occurrence of complications, you must strictly follow the doctor’s recommendations.
Forecasts for a bicornuate uterus
After Strassmann's operation, the ability to carry and give birth to a healthy child increases by 50%, and the threat of miscarriage is possible in only 30% of cases. In the presence of a bicornuate uterus, the development of the embryo in utero depends on the diameter of the orifice where conception occurred. With enough space, as well as the possibility of a normal supply of oxygen through the placenta to the embryo, natural birth without pathology is quite possible.
When registering during pregnancy, after diagnostic measures are carried out, careful monitoring of the entire period of pregnancy is necessary. In the later stages (after 26 weeks), in the presence of bleeding and isthmic-cervical insufficiency, it will be necessary to perform a cesarean section.
In the normal course of pregnancy, immediately a few weeks before birth, it is necessary to carry out ultrasound monitoring to determine the position of the embryo in the uterus. After this, the issue of the birth itself is decided.
Indicators of the presence of bicornuate uterus pathology in women in the world reach 0.5% (!) of cases. These are very low numbers, but if they exist, it is worth thinking about how to properly manage pregnancy so that our future generation does not suffer from the problems of their mothers. And for this it is enough to lead a healthy lifestyle before conception and during pregnancy.
Pathology of the cervix
Female pathologies of the uterus can affect different parts of this organ. Cervical pathology is quite common. This is a group of diseases, many of which threaten not only fertility, but also the life of a woman. Among them:
- pathology of the cervical epithelium (true erosion, pseudo-erosion, ectopia, ectropin, leukoplakia, erythroplakia);
- inflammatory diseases (cervicitis, endocervicitis, ectocervicitis);
- post-traumatic conditions (scars on the cervix, isthmic-cervical insufficiency)
- oncological diseases and precancerous conditions (polyps, dysplasia, cancer).
Causes of cervical pathology
Congenital pathology of the cervix develops very rarely; much more often the disease affects a woman during her life. The causes are different for different diseases. These are mainly dishormonal disorders, infections, and lifestyle features.
Pathology may develop after operations, abortions, complicated childbirth, which can cause the formation of scars on the cervix. Isthmic-cervical insufficiency develops, which reduces the chances of bearing a child during pregnancy (the damaged cervix is not able to withstand the pressure exerted by the fetus).
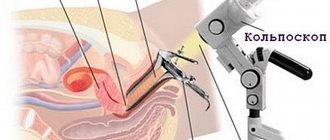
Diagnosis of various types of cervical pathology
Diagnosis of cervical pathology is carried out using colposcopy. The Schiller test (staining the cervix with Lugol's solution) and the acetate test (treating the cervix with 3% acetic acid) are used. If necessary, tissue is taken for biopsy.
Treatment of cervical pathology
Treatment for cervical pathology may vary depending on the type of disease. In some cases, conservative treatment is used (for example, for dishormonal diseases), in others - surgical treatment (isthmic-cervical insufficiency, benign or malignant tumors, precancerous conditions).
At VitroClinic you can diagnose any type of pathology of the cervix and uterine body. For this we have all the necessary equipment.
Make an appointment
What exactly is a uterus?
The uterus is a muscular organ. It is located in the pelvic area. In a non-pregnant state (normally) it is the size of a matchbox. The uterus is a hollow organ consisting of 3 main layers:
- perimeter (external) – covers the body of the organ, borders the peritoneum and bladder;
- myometrium (muscular) – is the middle layer. Serves to stretch and reduce the size of the organ, participates in labor during contractions of the uterus (contractions);
- endometrium (internal) – grows anew every menstrual cycle. It serves as the attachment site for the embryo and plays a huge role in the development of the baby. If pregnancy does not occur, it dies from the uterus and comes out mixed with blood (menstruation).
During a special period in a woman’s life—pregnancy—the uterus can stretch many, many times. This organ is the only one in the body that has such elasticity. Agree, it’s hard to imagine a soft matchbox into which you could put a newborn baby. What if it's twins or triplets?
Recently, the number of multiple pregnancies has increased sharply. This can be attributed to the fact that many couples in the 21st century began to resort to modern reproductive technologies, for example, in vitro fertilization (IVF). Now the birth of triplets is no longer nonsense. Multiple births have occurred before. A sufficient number of cases described in world medicine indicate the birth of four, five, six and even seven living healthy twins at once. The only case in the world of the birth of eight viable babies at the same time was registered in the USA in 2009. American Nadia Suleiman gave birth to 6 boys and 2 girls at the same time as a result of IVF. But the absolute world record, listed in the Guinness Book, was set by a resident of India. She gave birth to 11 living children. Her uterus reached an unrealistically large size during pregnancy.