Author:
Kuzmina Tatyana Sergeevna dermatologist, Ph.D.
Quick transition Treatment of nevi
A dermatologist or dermato-oncologist monitors nevi. A dermatologist, dermato-oncologist, or surgeon can remove a nevus. If the nevus is located on the conjunctiva of the eye, observation by an ophthalmologist is necessary.
Forms and complications of nevi
There are melanocytic (containing pigment cells - melanocytes) and non-melanocytic nevi (formed by cells other than melanocytes), which include epidermal nevus, nevus of the sebaceous glands, Becker's nevus and some other benign formations, vascular nevi of the skin.
Melanocytic nevi
There are acquired and congenital melanocytic nevi.
Acquired melanocytic nevi (AMN) are benign skin tumors. As a rule, they do not have a tendency to undergo malignant transformation. Special forms of acquired melanocytic nevi include Spitz nevus, Reed's nevus, spotted nevus (spilus), halonevus (Setton), and blue nevus (Jadassohn-Tiche) lying in the deep layers of the skin.
Atypical (dysplastic) nevi (AN) are classified into a separate group. Unlike common acquired melanocytic nevi, atypical melanocytic nevi may have some clinical characteristics of melanoma, such as asymmetry, ill-defined borders, multiple colors, or a size greater than 6 mm. Their main difference from a malignant tumor is stability, absence of changes over time and similar characteristics in one person. Atypical melanocytic nevi have a relatively increased risk of malignant transformation and require careful monitoring.
Congenital melanocytic nevi occur as a developmental defect (hemartoma) and are usually present at birth. Large congenital melanocytic nevi are also associated with an increased (but still low) risk of malignant transformation. Very rarely, they can be associated with a pathological accumulation of melanocytes in the central nervous system (neurocutaneous melanosis). Congenital melanocytic nevi with the expected size in an adult (over the course of life they will increase in proportion to the child’s growth) also require increased attention and medical supervision.
Nevi of Ota and Ito also have a melanocytic structure, but they are not based on excessive cell division, but on their accumulation in the deep layers of the skin.
Benign pigmented skin neoplasms (moles)
Nevus ( noncellular nevus , pigmented nevus , nevoid tumor , birthmark ) is a pigmented (colored) formation on the skin, which includes nevus (pigment) cells. Nevi are benign neoplasms; most researchers associate their occurrence with the migration in the embryonic period of the precursors of pigment cells (melanoblasts) from the neuroectodermal tube to the basal layer of the epidermis.
The nevus is of particular interest due to the fact that in place of a pre-existing congenital or acquired benign nevus, such a formidable malignant neoplasm as melanoma .
Almost all people have various congenital and acquired nevoid neoplasms. More than 90% of the population has pigmented skin tumors. The average number of nevi in each person is 20, ranging from 3 to 100, and their number usually increases with age. Not all nevi can potentially degenerate into melanoma, so they are usually divided into melanoma-hazardous and melanoma-non-hazardous.
Melanoma-dangerous nevi are much less common (about 10%) than melanoma-non-dangerous nevi. These nevi do not differ in the age of patients, localization of lesions and other clinical and anatomical data. It is important to consider that it is impossible to carry out differential diagnosis based on the degree of pigmentation of the lesion. Various injuries - mechanical, chemical, radiation, both acute and repeated - can be factors that provoke the transformation of some types of nevi into melanoma, primarily borderline or other melanoma-hazardous ones. In this regard, a biopsy of a suspicious skin element is strictly contraindicated, as well as its cosmetic treatment using directly traumatic methods (partial removal, electrocoagulation, cryotherapy, exposure to chemical and other agents). The percentage of melanoma patients who have clear indications of trauma preceding the development of the tumor (after incomplete cosmetic removal of a pigmented nevus, accidental trauma) varies from 20 to 78%. A biopsy or incomplete removal of the lesion in order to distinguish a melanoma-dangerous nevus from melanoma or other skin lesions is strictly unacceptable.
General principles of treatment of pigmented neoplasms
Any pigmented skin growths require special attention. Greater caution should be shown to nevi localized in traumatic areas of the skin, as well as to previously injured nevi that are rapidly growing or rapidly changing their pigmentation.
Therapeutic tactics for pigmented nevi boil down, first of all, to the categorical refusal of any traumatic treatment methods: electrocoagulation, cryodestruction and the use of various cauterizing solutions.
Treatment of pigmented neoplasms is radical surgical excision of the lesion within intact skin. The use of modern non-traumatic suture materials and the rules of aesthetic surgery makes it possible to achieve barely noticeable postoperative scars. Surgical treatment (excision along the edge of the formation), as well as various cosmetic manipulations (cryodestruction, chemodestruction) of melanoma-free neoplasms do not carry the risk of malignant transformation of these formations.
A completely different tactic is followed for melanoma-dangerous nevi. If a melanoma-hazardous formation is suspected, the patient should be immediately sent to an oncologist! The tactics and technique of surgical intervention are determined by the location and size of the melanoma-dangerous pigmented nevus. The best limits for excision on the trunk and limbs, taking into account, on the one hand, the clear limitation of “quiet” nevi and, on the other hand, cosmetic considerations, is considered to be a distance of 0.5 cm in all directions from the borders of the nevus; this is quite sufficient for the prevention of melanoma. The nevus is excised with surrounding incisions along with the surrounding skin and the surface layer of tissue; the tissue is sutured with a cosmetic suture using non-traumatic suture material, which allows one to achieve good cosmetic results. On the face, neck, auricle, fingers and nail bed, for anatomical and cosmetic reasons, more economical excision of melanoma-dangerous nevi is allowed, but not less than 0.1-0.2 cm from their borders. On the face and neck, sutures are applied with a very thin thread, which allows for maximum cosmetic effect. In all cases of surgical excision of a pigmented nevus without exception, histological confirmation of the diagnosis is necessary - i.e. the excised area is necessarily sent for microscopic examination; if the result is atypical cells (melanoma), the patient is referred to an oncologist.
Patients who refuse radical surgical treatment, as well as in the case of its impossibility due to difficult anatomical localization, should carefully protect their tumor, exclude its injury, solar radiation and be monitored by an oncologist.
Borderline pigmented nevus
A borderline pigmented nevus is a flat dark brown or black nodule up to 1 cm in diameter with a smooth, dry surface, develops at the border of the epidermis and dermis, and is characterized by increased activity of pigment cells (melanocytes). Sometimes a border nevus looks like a spot of round or irregular shape with smooth wavy edges. Borderline nevus does not have a favorite location. It can be located on the skin of the face, neck, and torso. Pigmented nevi on the skin of the palms, soles, and genitals are almost always borderline. Borderline nevus is most often congenital, but can appear in the first years of life or even after puberty. An important differential diagnostic sign of a borderline pigmented nevus is the complete absence of hair on it.
Pigmented border nevus must be distinguished from cavernous hemangiomas, which are characterized by a softer consistency of the node, from seborrheic (“senile”) keratoma, which, as a rule, has a less smooth, “rough”, greasy surface. In the differential diagnosis between borderline pigmented nevus and early melanoma, anamnesis plays an important role. Most patients with melanoma indicate that their tumor developed in place of a pigmented nevus that existed for a long time or even from birth, which did not cause any inconvenience. The nevus grows slowly according to body weight. During puberty, patients may notice an acceleration in nevus growth - a consequence of hormonal changes and an increase in the level of metabolic processes, including pigmentation. Mechanical trauma is the predominant factor accompanying the malignancy of previously “quiet” nevi.
The following borderline nevi are especially dangerous: systematically injured, located on the sole, nail bed, or in the perianal area. Timely removal of nevi in these localizations is a reliable prevention of melanoma. Excessive insolation, thermal or balneological treatment of concomitant chronic diseases also play a negative role in the development of melanoma. Acceleration of nevus growth after injury or active insolation, inflammatory changes, discoloration, the appearance of itching, weeping, and induration should be alarming.
Blue or blue nevus
Blue or light blue nevus (Jadassohn-Tiche nevus) is a dark blue or bluish node, sharply demarcated from the surrounding skin, round in outline, densely elastic consistency with a smooth, hairless surface. The blue color is due to massive accumulations of melanin in the deep layers of the dermis. The size of the node, as a rule, does not exceed 0.5 cm. Blue nevus is most often located on the face, limbs, and buttocks. In most cases, blue nevus is a solitary formation. Blue nevus occurs in all age groups, most often in middle-aged women . Clinically, a blue nevus is difficult to distinguish from a pigmented borderline nevus. However, clinical features such as large demarcation and infiltration, blue or blue color, appearance at a later age and hemispherical shape allow for a differential diagnosis. With a deeper location in the skin, a blue nevus sometimes has to be differentiated from a dermatofibroma. Symptoms such as less infiltration, color and usually a solitary lesion help to distinguish it. The development of melanoma at the site of a blue nevus is rare, but this nevus is classified as melanoma-dangerous .
Nevus Ota
Nevus of Ota, or oculodermal melanocytosis, is a large, usually unilateral pigmented nevus on the face in the area of innervation of the I and II branches of the trigeminal nerve (the area of the forehead, cheeks and nose). Clinically, dark brown pigmentation is noted in various parts of the eye: conjunctiva, sclera, iris. At the same time, a massive pigmented nevus (or nevi merging with each other) is detected on the cheek, upper jaw and zygomatic region of the same side, black and bluish in color. All this creates the impression of “dirty skin” on the affected side of the face. In rare cases, the red border of the lips and the mucous membranes of the soft palate, pharynx, larynx and nose are affected. Women get sick more often. Nevus of Ota is congenital, but can occur in early childhood or even during puberty. It usually grows slowly. Apart from cosmetic inconveniences, it does not cause any disorders, including visual impairment. There are known cases of melanoma developing in its place. Close to the nevus of Ota and an even rarer variety is considered to be the nevus of Ito, located in the supraclavicular, scapular regions and the deltoid muscle region.
Giant pigmented nevus
A giant pigmented nevus is always congenital, increases in size as the child grows, reaching a large size (from the palm of the hand or more) and sometimes occupies a large part of the torso, neck and other areas. Usually, over a considerable extent, the surface of the nevus is lumpy, warty, with deep cracks in the skin. Areas of hypertrichosis (hair nevus) are common. The color varies from grayish to black and is often heterogeneous in different areas. Malignancy of a giant pigmented nevus occurs in 1.8-10.0% of cases. Treatment tactics for suspected pigmented borderline and blue nevi, especially if they are located on accessible insolation and frequently injured areas of the skin, boil down to the categorical refusal of any traumatic treatment methods: electrocoagulation, cryotherapy, the use of various cauterizing solutions and incomplete surgical excision. If necessary, economical surgical excision of the lesion with the surrounding skin is performed at a distance of 0.5 cm in all directions from the borders of the nevus along with subcutaneous fatty tissue; this is quite enough to prevent melanoma. On the face, neck, auricle, fingers, due to anatomical features, a more economical excision of melanoma-dangerous nevi is permissible with a deviation of 0.2-0.3 cm from its borders. For giant nevi, which cause great cosmetic inconvenience to patients, step-by-step excision is used, followed by skin plastic surgery .
Dubreuil's melanosis
Dubreuil's melanosis is a nevoid formation, the connection of which with melanoma is indisputable. Dubreuil's melanosis usually begins as a small brownish pigmented spot that slowly spreads around the periphery. A clinically mature lesion has blurred boundaries and an uneven surface of dark brown and sometimes black color, more saturated than the color of pigmented nevi. Within the formed focus there are areas of different shades (brown, gray, black, bluish). The skin pattern over the lesion remains unchanged and becomes rougher. Elements resembling a senile wart may appear. Sometimes atrophy, hyperkeratosis, and flat surface papillomatosis develop. Characterized by increased pigmentation along the periphery of the lesion. Inflammatory phenomena are extremely rare. In most patients, Dubreuil's melanosis manifests itself in one focus. The most common location is open areas of the skin, especially the face (cheeks, nasolabial folds, nose, forehead), less often the neck and scalp. Dubreuil's melanosis mainly affects older people, which allows it to be classified as a senile dermatoses. The clinical picture of limited precancerous Dubreuil's melanosis, especially in the stage of a formed lesion, in most cases is so characteristic that it does not cause great diagnostic difficulties.
Differential diagnosis must be made with large seborrheic (senile) keratoma, pigmented basal cell carcinoma, and some forms of nevi. However, all these nosological forms are characterized by clearly demarcated lesions. With basal cell carcinoma, a raised ridge with “pearls” is visible (especially through a magnifying glass); the central part of the tumor is often ulcerated. The surface of a seborrheic keratoma is more lumpy and often “greasy” to the touch. A clinical symptom such as uneven hyperpigmentation, as well as medical history - onset of the disease in old age and very slow progression of a single lesion - are very helpful in diagnosing Dubreuil's melanosis.
The causes of malignancy of Dubreuil's melanosis have not been established; trauma and insolation are considered to be the impetus for the onset of invasive tumor growth . Dubreuil's melanosis is a more pre-melanoma skin lesion than borderline pigmented nevus, not to mention other melanoma-dangerous nevi. Therefore, Dubreuil’s melanosis is considered not so much melanoma-dangerous as directly pre-melanoma and even an absolute precancer of the skin .
The treatment strategy for Dubreuil's melanosis differs significantly from that for melanoma-dangerous nevi. First of all, it is unacceptable to leave patients without active treatment , which is possible with Ott’s nevus and other melanoma-dangerous nevi after warning patients about the danger of injury. Another difference is that wide surgical excision of Dubreuil's melanosis , given its predominant location on the face, is associated with serious technical and cosmetic difficulties, especially with large lesions . Sometimes excision of large lesions on the body is completed with plastic surgery using displaced flaps. The method of choice for Dubreuil's melanosis on the trunk and limbs is excision of the lesion, 0.5 cm from its edges.
Fibroepithelial nevus
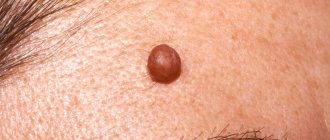
Fibroepithelial nevus belongs to the group of melanoma-NON-dangerous nevi and nevoid skin lesions . Fibroepithelial nevus, along with pigmented intradermal nevus, is the most common nevoid formation on human skin and the most common reason for visiting a surgeon. Fibroepithelial nevus often first appears during various periods of intrauterine life, sometimes existing from birth. Its growth is usually very slow. Localization can be very different, but mainly on the face and torso. The number of formations varies from one to several dozen. Histologically, fibroepithelial nevus has the structure of a soft fibroma.
Clinically, a fibroepithelial nevus is a hemispherical, painless formation rising above the skin level with a soft or soft-elastic consistency ranging from a few millimeters in diameter to the size of a bean and, rarely, larger. Color varies from normal skin or pinkish-red (usually with a slight bluish tint) to bluish-violet and dark brown. With the latter or close to it coloring, the greatest difficulties arise in differential diagnosis with borderline pigmented and blue nevus. The shape of a fibroepithelial nevus is usually regular, round, and the surface is smooth, although less smooth than that of a borderline pigmented nevus. The surface of the nevus is often penetrated by single vellus or bristly hairs or even a coarse tuft of hair, especially in women (fibroepithelial pilaris nevus). With a pronounced vascular component in the form of a telangiectatic mesh on the surface, they speak of angiofibroepithelial nevus, which can also be hairy.
In most patients, there is no inflammation around the fibroepithelial nevus. Sometimes after an injury the nevus becomes inflamed (when shaving the face, after a blow). In these cases, an inflammatory rim develops around the circumference. In typical cases, diagnosing a non-inflammatory fibroepithelial nevus is not difficult. Differences from borderline pigmented and blue nevi: color (even with pigmented fibroepithelial nevi, the color is less saturated), shape, multiplicity, frequent presence of hair. In its clinical picture, an inflamed fibroepithelial nevus differs sharply from the picture observed during malignancy of a melanoma-dangerous nevus.
Papillomatous nevus
Papillomatous nevus has an uneven, bumpy surface, often localized on the scalp, but can also occur on any other part of the skin. The sizes are often large, up to several centimeters, the outlines are irregular, the color varies from the color of normal skin to brownish, less often - dark brown or even black. Like fibroepithelial nevus, papillomatous nevus is often riddled with hair. As a result of injury, the papillomatous nevus becomes inflamed. The location of the papillomatous nevus on the face and other open areas of the skin causes patients to persistently desire to get rid of the formation, which can be subjected to cosmetic treatment.
Verrucous nevus
Verrucous nevus is a clinical type of papillomatous nevus. Its surface is even more lumpy, in pronounced cases it has the appearance of a “head of cabbage”, penetrated by deep folds and cracks. It protrudes significantly above the surface of the skin and is usually more pigmented (pigmented, or pigmented verrucous nevus). Like papillomatous nevus of the extremities, most often there is a single focus. Clinical recognition of verrucous nevus does not present any particular difficulties. Sometimes, especially if it is small, a verrucous nevus can be mistaken for a giant common wart. Correct recognition is helped by anamnestic data (exists from birth or early childhood, grows very slowly), frequent presence of hair on the surface; usually the lesion is single. The treatment and tactical approach is similar to papillomatous nevus.
Halo nevus (Setton's nevus)
Halo-nevus is clinically a reddish-brown nodule, slightly raised above the skin level, 4-5 mm in diameter, round or oval, surrounded by a rim of depigmented skin. The width of the depigmented area is 2-3 times greater than the diameter of the hyperpigmented nodule. Halo nevus is often multiple, predominantly localized on the torso and arms, less often on the face. Often, Halo nevus undergoes spontaneous regression. The clinical picture of Halo-nevus is typical and does not cause differential diagnostic difficulties. The development of melanoma at the site of the Halo-nevus, even after injury, is not observed. It has been noted that Halo nevus sometimes occurs in malignant tumors of internal organs and melanoma.
"Mongolian Spot"
“Mongolian spot” is an irregularly shaped rounded skin lesion, colored bluish or brownish, up to 5-6 mm in diameter, located exclusively in the lumbosacral region. The “Mongolian spot” is almost always a congenital formation; in most patients it disappears without a trace in childhood. The development of melanoma at the site of the “Mongolian spot” is not observed and does not require treatment.
Intradermal nevus
Intradermal nevus, or common birthmark, occurs in almost all people. Birthmarks are located in the skin and mucous membranes. Most often, these nevi are congenital; the pigmentation is usually brown. For the vast majority of people, birthmarks do not cause cosmetic discomfort.
Dysplastic nevus
Dysplastic nevus is an acquired pigment formation, histologically represented by a random proliferation of polymorphic atypical pigment cells (melanocytes). It occurs on clear skin or as a component of a complex nevus. Dysplastic nevus has characteristic clinical and histological features that distinguish it from acquired noncellular nevi. It is considered a precursor to superficial spreading melanoma and is considered a risk factor for melanoma.
Dysplastic nevus are pigmented spots of irregular shape and with unclear boundaries, slightly raised above the skin level, their color varies from reddish-brown to dark brown on a pink background. Dysplastic nevi first attracted attention for their unusual appearance and increased frequency in some families (they are inherited). As a rule, they are larger than ordinary birthmarks, reaching 5–12 mm in diameter; the localization is also different: dysplastic nevi, although they can occur anywhere, are more often found in areas usually covered by clothing (on the buttocks, chest), or on the scalp. Most people have an average of 10 ordinary moles, while dysplastic nevi can have more than 100. Ordinary nevi usually appear during puberty, while dysplastic nevi continue to appear even after 35 years.
Comparative characteristics of dysplastic nevus and acquired noncellular nevus
| Sign | Dysplastic nevus | Acquired noncellular nevus |
| Color | Heterogeneous - various combinations of light brown, brown, black, red and pink; dysplastic nevi can differ significantly from each other | Uniform - light brown or brown |
| Form | Incorrect; fuzzy, blurred boundaries; peripheral areas are at skin level | Regular, round or oval; boundaries are clear; the formation is either at the level of the skin or evenly raised above it |
| Dimensions | Usually > 6 mm in diameter, often > 10 mm; occasionally < 6 mm | Typically < 6 mm in diameter |
| Quantity | Often multiple (> 100), but single lesions possible | On average, an adult has from 10 to 40 nevi; approximately 15% do not have them at all |
| Localization | Open areas of the body, most often the back; found on the scalp, mammary glands and buttocks | Typically exposed areas of the body above the waist; scalp, mammary glands and buttocks - extremely rare localization |
Vascular nevus
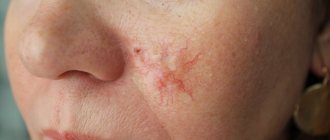
Vascular nevus (naevus flammeus, port-wine stain) is an anomaly of the capillaries of the dermis, manifests itself in the form of a spot from light pink to red-brown. Vascular nevus, located in the center of the face or back of the head, is not combined with other developmental defects and usually fades with age. With an asymmetrical, unilateral localization (on the face or limbs), a vascular nevus is usually one of the manifestations of Sturge-Weber syndrome or Klippel-Trenaunay syndrome. In this case, with age, the nevus usually darkens, and its surface in some places becomes bumpy and rises above the skin level.
Capillary hemangioma
Capillary hemangioma or strawberry nevus is the most common congenital vascular tumor. It begins as one or more pale pink papules that grow rapidly, become lobulated, and range in color from bright red to dark blue. Capillary hemangiomas appear at 3-5 weeks of life; 70% of them disappear spontaneously by the age of 7 and do not require treatment. Treatment. If the location and rapid growth of the tumor lead to visual or respiratory problems, resort to the injection of corticosteroids into the lesion, cryodestruction, laser therapy or surgical excision.
Symptoms of nevi
Nevi look like spots or nodules on the skin. Some of them are barely noticeable, others have a rich brown (melanocytic or pigmented) or red (vascular nevi) color.
As a rule, nevi do not cause any discomfort and are not felt.
Nevi can change their appearance and increase throughout life. It is important to correctly assess these changes; such manifestations can not only be a variant of the norm, but also serve as one of the signs of malignant skin formations.
How to distinguish a dysplastic nevus from melanoma?
A theoretically prepared reader, after reading the table, will exclaim: “You have now listed almost all the symptoms of melanoma!!! How can you tell them apart???” Unfortunately, a person without experience in diagnosing skin cancer, as a rule, cannot do this.
If you find moles on your skin with signs of dysplastic nevi, you need to see an oncologist. This doctor will examine them and also tell you about the signs of nevi turning into melanoma and the principles of monitoring such formations.
Stages of changes in nevi
Melanocytic nevi , both acquired and congenital, are characterized by staged changes throughout life. The classic path of development includes 3 stages, which differ in the depth of the formation:
- a simple nevus or borderline nevus is a superficial flat brown spot;
- a complex or combined nevus is located deeper and looks like a brown spot or raised formation on the skin;
- An intradermal nevus is a light-colored, raised formation located deep in the skin.
How they appear
Moles are divided into congenital and acquired.
Congenital nevi
This species represents a defect of embryonic development. Because of it, the transition of melanoblast cells into the skin is disrupted. Nevi appear due to the accumulation of these cells.
Moles appear in the first years of a person’s life.
Small-diameter nevi almost never degenerate. In larger ones, this process is most likely, so if there are such nevi, you need to be constantly monitored by specialists. It is forbidden to irradiate these nevi under ultraviolet light, and, if possible, it is better to remove them in a timely manner.
Acquired nevi
Nevi form in new places on the skin, changing contours, relief, and color. It is necessary to monitor these processes and have follow-up examinations with a doctor.
The appearance of moles can be genetic and can be passed on from parents to children.
Often moles begin to appear due to changes in the endocrine system associated with pregnancy or teenage changes. Also, the number of moles increases due to excessive exposure of the skin to sunlight, so excessive exposure to solariums and sunbathing negatively affects health.
By adolescence, the number of nevi increases, but by old age it decreases.
Treatment of nevi
In most cases, no treatment is required, only observation is required, since nevi are benign formations. If a malignant nature is suspected and formations with a high risk of malignant transformation are identified, surgical excision is performed. It is possible to remove the nevus at the request of the patient for aesthetic reasons or because of discomfort (for example, when localized in areas of frequent trauma by clothing).
Features of the treatment method
Surgical excision of the nevus is optimal. This method allows for radical removal with a scalpel followed by suturing of the wound surface. In some cases, when nevi protrude above the surface of the skin, a radio knife, electric knife or laser knife can be used. In all cases of surgical treatment of melanocytic nevi, it is necessary to conduct a histological examination of the removed tissue.
Diagnostics
It is necessary to diagnose melanoma in time and determine the stage of its development in order for the treatment of the disease to be successful.
First, an anamnesis is collected, the doctor learns about changes in the nevus.
Do not take a biopsy or expose the mole to chemical and electrical effects unnecessarily.
To diagnose you need to do:
- Histological examination (a superficial smear is taken if there is bleeding or cracks, provided that the tumor is removed immediately after the diagnostic results);
- Epiluminescent microscopy (examination of a mole using a special apparatus to determine its structure);
- CT (image recording, data processing, comparison with standards).
How are nevi treated in the Rassvet blade?
The doctor will examine the patient's skin completely to eliminate the risk of missing melanoma or other skin cancer. Suspicious formations are further studied using a device that allows you to examine the skin with 10 times magnification - a dermatoscope. The patient's chart describes nevi that require observation. The doctor will suggest surgical removal of suspicious nevi, followed by histological examination of the removed material (sent to an expert laboratory). Removal of nevi for aesthetic reasons can be performed at the request of the patient.
Recommendations of a dermatologist for patients with nevi:
- avoid excessive ultraviolet irradiation of the skin (tanning, sunbathing, solariums, ultraviolet drying of manicure and pedicure coatings); when staying outdoors for a long time, use a broad-spectrum photoprotective cream with SPF 30 or higher, clothing that covers the skin, a hat and glasses with an ultraviolet filter;
- try not to injure nevi when shaving, combing, changing clothes;
- undergo an annual preventive examination of nevi with a doctor;
- independently examine nevi according to the ABCDE rule;
- if there are a large number of nevi (50-100 or more), especially in combination with the presence of risk factors (sunburn, visits to a solarium, melanoma and skin cancer previously identified or in close relatives, the presence of atypical nevi), undergo a digital skin mapping procedure.
Dysplastic nevus syndrome
Unfortunately, there is a syndrome that in Russian literature is often called nevus dysplastic syndrome (in foreign literature - FAMMM).
This disease has 2 diagnostic criteria
- the number of dysplastic nevi on the skin is more than 50
- melanoma in relatives
This disease may be associated with a mutation in the CDKN2A gene, which also increases the risk of developing pancreatic cancer
With this syndrome, the risk of developing melanoma, according to different authors, varies from 56 to 100%. The disease requires regular (once every few months) monitoring by an oncologist.
Out of sight, out of sight. How to get rid of moles
Not an easy question. Many factors influence the ability to remove tumors. Unfortunately, no pills have yet been invented that will relieve you of annoying or dangerous moles.
Yes, treatment of small nevi usually does not cause problems.
Successful removal depends on:
- Doctor's qualifications
- Mole size
- Nevus locations
The first option is surgery. The doctor cuts off the mole, some adjacent skin, and then stitches the wound. After removal, the nevus heals quite quickly, but a noticeable mark remains.
Whether this is good is up to you to decide.
What about laser surgery?
Yes, modern technologies do offer new treatments, but they do not work miracles, as some people believe. Some skin diseases are treated with lasers. But not all nevi.
The laser beam vaporizes the outer layer of skin and cells of the mole. The deeper it is rooted, the more difficult it is to destroy it completely - sometimes the surface layer is burned out, but the base remains intact. Then the nevus grows back.
The operation has to be repeated again and again, and there is no guarantee of results. So the surgical procedure is sometimes more reliable than laser surgery.
However, in some situations, a high-tech procedure accomplishes the task. Removes small nevi. Working with large tumors is much more difficult.
We recommend choosing laser nevus removal only after consulting a dermatologist and checking the tumor.
Another important point is the choice of doctor. Many doctors have accumulated vast experience in removing small moles. Everyone has them. Therefore, doctors work with them very often and know well how to quickly remove nevi.
But what about large moles?
They are not common and therefore it is difficult to find a doctor who regularly operates on them. Read reviews about nevus removal on the websites of different clinics. This is useful. You will learn what operations the doctors of these medical institutions performed and the patients’ impressions of their work.
Gather more information.
When you see your dermatologist, ask about available methods for removing moles. Perhaps in your case, surgery and laser therapy are not the best options. Harmless nevi do not need to be removed at all.
Many medical institutions remove moles. But where to go? We would like to recommend one of these clinics.