Almost everyone is familiar with a “cold” on the lips. As soon as you catch a runny nose or get nervous, an unpleasant harbinger immediately appears - a tingling sensation somewhere around the mouth.
The herpes simplex virus is present in the body of 95% of people. And only a few have immunity, the reasons for which are still unclear.
The virus enters the body in early childhood: at 3–4 years, when the antibodies against the herpes virus transmitted to the baby by the mother are depleted. Most often, infection occurs if a child is kissed by carriers of the infection. In addition to a kiss, the virus can enter the body, for example, with saliva. It penetrates the mucous membranes, reaches the nerve endings, rises into the cranial cavity, where it “hides” in a nerve plexus called the trigeminal ganglion and “sleeps” there until it is reactivated.
Herpes “wakes up” when immunity decreases
Causes of recurrence of herpes on the lips: stress or emotional distress; various other diseases, in particular colds, flu, diabetes, HIV; poisoning or intoxication; drinking alcohol, caffeine and smoking; excessive ultraviolet radiation; hypothermia or overheating; onset of menstruation; overwork and exhaustion; poor nutrition/diet or stomach upset; other factors individual to each person.
After “awakening,” the virus travels back to the skin. As the virus moves through a nerve, it causes inflammation of the nerve tissue.
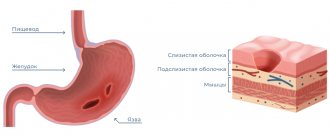
The development of herpes can be divided into several stages. At the first stage, the person feels unwell. At the site where the “fever” appears, there is pain, tingling, and the skin turns red. At the inflammation stage, a small painful blister filled with fluid forms. After some time, the bubble bursts and a colorless liquid containing billions of viral particles flows out of it. An ulcer appears in its place. At the final stage, the ulcer becomes covered with a crust.
Most often, herpes appears on the lips, but lesions can also appear on the face, in the ears or in the mouth.
How does primary infection occur?
Often, the initial infection with a herpes infection has no symptoms and is not noticeable. But it happens that complications appear along with herpes:
- gingivostomatitis - inflammation of the oral mucosa and gums;
- an increase in temperature, accompanied by the appearance of blisters and ulcers in the mouth;
- herpetic panaritium (inflammation of the finger tissue) - the infection can spread to the fingers if they are pulled into the mouth;
- rashes can occur throughout the oral cavity, affecting the gums, which turn red and bleed. The child refuses to eat because the process becomes painful.
What to do if you have a “cold” on your lips
At the moment, no drugs or treatment methods have been developed that would completely destroy the herpes simplex virus in the human body. But we can give some advice to those suffering from herpes.
- Strictly follow the rules of personal hygiene! Since herpes is contagious, it is necessary to wash your hands with soap and use separate utensils and towels.
- Don't put your hands near your eyes! And do not wet your lenses with saliva! Herpes can affect the mucous membrane of the eye.
- It is not recommended to touch the viral rash or kiss. The virus can be transmitted by wearing one lipstick or smoking one cigarette.
- If you try to remove a blister or scab over a sore, the virus can spread to other parts of the body.
- Avoid oral sex! The virus from the affected lips can cause genital herpes in a partner.
- A young mother must also take certain precautions to protect her baby from contracting herpes. If you have herpetic rashes, you must wash your hands with soap and water every time before touching your child. And under no circumstances should the affected surface come into contact with the child’s skin.
Diagnostics
Diagnosis includes visual inspection of the patient's clinical manifestations if an exacerbation is typical. The diagnosis of HSV infection is often based on clinically characteristic lesions. Laboratory confirmation may be necessary if the infection is severe, the patient is immunocompromised, or the patient is pregnant, and the lesions are atypical. Depending on the severity of the clinical picture, a number of necessary auxiliary diagnostic procedures are performed:
- a set of standard laboratory tests (general blood test, urine test, etc.);
- serological tests (ELISA) to detect antibodies to a specific type of virus in the patient’s blood;
- PCR analysis is a highly informative diagnostic method that allows you to detect the presence of a virus in the body with up to 99% accuracy.
Herpes simplex virus must be distinguished from herpes zoster, which rarely recurs and usually causes more severe pain and larger lesions that are distributed along the dermatome and usually do not cross the midline. It should also be noted that collections of vesicles or ulcers on an erythematous basis are uncommon in genital lesions other than those caused by HSV infection.
How to minimize discomfort
You should start using antiherpes medications as soon as you feel a tingling sensation. Medicines will not get rid of the virus, but they will stop its development and speed up recovery. There are drugs that prevent the development of the virus: tablets, ointments for external use, which help heal blisters and ulcers and reduce discomfort.
When applying the ointment, use cotton swabs to avoid transferring the virus from your lips to the skin of your fingers.
Herpes requires the attention of specialists! A “cold” on the lips can be a symptom of serious diseases: a sharp decrease in immunity, cancer, HIV infection.
If you are suffering from relapses of herpes, consult a doctor. A specialist will not only save you from unnecessary worries and eliminate health hazards, but will also help you choose a comprehensive program for the prevention and treatment of herpes.
In order to make an appointment with an immunologist or dermatologist for a program for the diagnosis and treatment of herpes, call the Family Doctor clinic (clinic hours: Mon-Fri from 8.00 to 21.00, Sat-Sun from 9.00 to 20.00), or sign up for reception and diagnostics via online registration form
Principles of treatment of herpes simplex
WITH
Among viral diseases, herpes infection occupies one of the leading places, which is determined by the widespread spread
of the herpes simplex virus (HSV)
, more than 90% of its infection of the human population, the lifelong persistence of the virus in the body, the polymorphism of the clinical manifestations of the disease, and its resistance to existing treatment methods.
Unfortunately, modern medicine does not have treatment methods that can eliminate HSV from the human body. Therefore, the goal of therapeutic measures is: a) suppression of HSV reproduction during an exacerbation, b) formation of an adequate immune response and its long-term preservation in order to block the reactivation of HSV in areas of persistence, c) prevention of the development or restoration of those disorders that are caused by HSV activation in the body.
Currently, there are two main directions in the treatment of herpes simplex:
1) use of antiviral chemotherapy
, the main place in which is given to acyclic nucleosides and, first of all, acyclovir;
2) complex treatment method
, including immunotherapy (specific and nonspecific) in combination with antiviral therapy.
Creation of acyclovir
(ACV) opened a new stage in the treatment of herpes. In many countries around the world, the industrial production of acyclovir-containing drugs (ACV drugs) has been established.
Antiviral chemotherapy
Etiopathogenetic therapy is based on the ability of chemotherapeutic drugs to selectively disrupt the process of interaction between HSV and cells, to be included in the development cycle of only HSV at the stages of viral DNA synthesis and assembly of viral particles, inhibiting their reproduction, which ultimately leads to a virusostatic effect. Chemotherapy takes a leading place in acute herpetic infection, which occurs with damage to the central nervous system and other systems and organs, as well as in herpes of newborns. Antiviral drugs are of great importance in the treatment of recurrent forms of herpes simplex with damage to the skin and mucous membranes.
Etiopathogenetic therapy
Acyclovir
- a synthetic acyclic analogue of deoxyguanosine, a natural component of DNA, and today remains the standard of antiherpetic treatment. Acyclovir penetrates predominantly into a cell infected with a virus, where, under the influence of a virus-specific thymidine kinase, it transforms into an active form as a result of phosphorylation with the formation of mono-, di- and triphosphate. Acyclovir has found its use in the treatment of all forms of herpes infection. Pronounced antiherpetic activity, low toxicity, and the presence of several dosage forms (ointment, tablets, cream, suspension, solution for intravenous administration) allow the drug to be widely and effectively used in medical practice.
It has been established that in 5–7% of patients suffering from recurrent herpes (HR)
, during treatment, resistance to acyclovir develops or it initially does not have a therapeutic effect. The mechanism of resistance is associated with a decrease in the activity or absence of viral thymidine kinase, damage to the substrate specificity of this enzyme and the appearance of mutations in the DNA polymerase gene.
valacyclovir, has been developed based on acyclovir.
, which is the L-valine ester of acyclovir. The advantage of valacyclovir in comparison with acyclovir is that its oral administration creates concentrations of acyclovir in the blood serum and other internal media that are equivalent to those achieved only with intravenous administration of acyclovir. This is what allows the patient to reduce the number of doses of the drug during a relapse to 2 times a day (as opposed to acyclovir, which is taken 5 times a day) and take valacyclovir once a day for suppressive therapy.
Famciclovir
is transformed in the body into an active antiviral compound - penciclovir, effective against HSV-1, HSV-2 and other herpes viruses. Penciclovir reaches HSV-infected cells, where it is converted to triphosphate by the action of viral thymidine kinase.
Acyclovir, val acyclovir and famciclovir are “first aid” drugs for any form of herpes. However, ACV drugs exert their indirect virusostatic effect by interacting with the thymidine kinase of herpes viruses, which to a certain extent limits the universality of their action on HSV strains with genetically altered viral thymidine kinase activity. Therefore, the list of specific antiherpetic drugs has been supplemented with foscarnet.
Foscarnet
is a competitive inhibitor of pyrophosphate and has a wide spectrum of antiviral activity, inhibiting the DNA polymerase of herpes viruses. However, it should be noted that this phosphorus-containing drug is more toxic than acyclovir, which may limit its use.
There are a number of drugs with different mechanisms of antiviral action that can be used for herpes: brivudine, ribamidil, metisazone. And yet they are significantly inferior to acyclovir in therapeutic effectiveness.
Immunotherapy for herpes simplex
Impaired immune response is the most important link in the pathogenesis of herpes simplex. As a rule, the disease occurs against the background of suppressed immune reactions: there is a decrease in the total number of T- and B-cells, a change in their functional activity, disturbances in the macrophage component of immunity, in the interferon system. Correction of violations of nonspecific and specific immunity is one of the directions in the complex therapy of herpes simplex.
Nonspecific immunotherapy
includes the use of:
1) immunoglobulin;
2) interferons and interferon inducers;
3) drugs that stimulate the T- and B-links of cellular immunity and phagocytosis.
Mechanism of action of immunoglobulins
For a long time, herpes was explained by a replacement effect against the background of the inherent failure of humoral immunity for this disease. In recent years, it has been found that immunoglobulin preparations also have immunomodulatory and antitoxic effects and activate opson-phagocytic reactions.
Normal human immunoglobulin is used to treat recurrent herpes. The drug contains a sufficient amount of specific antiherpetic antibodies to achieve a therapeutic effect, which is explained by the almost 100% carriage of HSV in the population.
To treat severe forms of herpetic infection (central nervous system lesions, neonatal herpes, primary herpes in pregnant women), human immunoglobulin with a high content of antiherpetic antibodies (Sandoglobulin) or domestic immunoglobulin for intravenous administration can be used.
Wide spectrum of antiviral activity, absence of interferon-resistant (IF)
virus strains predetermined the prospect of using interferon as a means of etiopathogenetic therapy of herpes simplex. Interferons are factors of natural immunity, produced by cells in response to the influence of viruses, bacteria, foreign antigens and cause activation of effector immune cells involved in the reactions of elimination of infectious agents from the body. According to modern concepts, interferons, along with antiviral activity, have antiproliferative and immunoregulatory effects. IF increases nonspecific cell resistance (stimulates phagocytosis, increases the activity of natural killer cells), and the level of interferon formation can be used to judge the general immunological reactivity of the body.
Commercial series of human leukocyte interferon (HLI) produced by the domestic industry are species-specific and are quickly eliminated from the body (with intravenous administration after 4–6 hours, with intramuscular administration - after 20 hours). The high cost and complexity of industrial production of CLI to a certain extent limit its use. In practical healthcare, CLI is currently used in several dosage forms: 1) nasal drops; 2) PLI for injection - a mixture of interferons-a produced by leukocytes of clinically healthy donors, administered intramuscularly, subcutaneously, intravenously; the activity of 1 dose of the drug is 100,000 IU, 500,000 IU, 1000,000 IU; 3) leukinferon (for injection) – a natural complex preparation containing interferon-a and cytokines (1 dose – 10,000 IU); 4) interlock (for injection), 1.0 ml – 50,000 IU; 5) CLI in rectal suppositories (1 suppository contains 40,000 IU of antiviral activity).
The idea of interferon therapy found its development in the creation of genetically engineered interferons and in the use of endogenous interferon inducers.
For the treatment of various forms of recurrent herpes, domestic rectal suppositories Viferon, which contain recombinant a2-interferon, are used. A combined drug, kipferon, has been created (consists of immunoglobulins and recombinant a2-interferon) in the form of suppositories for rectal and vaginal administration.
With the help of interferon preparations (natural or genetically engineered), replacement therapy is carried out, as a result of which the production of the patient’s own endogenous IF can be blocked. This must be taken into account when prescribing long-term (more than 2 weeks) courses of IF therapy, especially genetically engineered forms (Reaferon, Viferon). In cases of long-term administration of IF to patients, they should be discontinued gradually, reducing the dose to 3, then 2 times a week, followed by complete discontinuation of the drug.
The ability to induce the production of endogenous IF
has a large group of natural and synthetic compounds: levamisole, dibazole, vitamin B12, pyrogenal, prodigiosan, which are the drugs of choice for the treatment of herpes.
A synthetic interferon inducer, the domestic drug Poludan (poly A:U), which has been used since the 1970s, has a pronounced therapeutic and prophylactic effect in recurrent herpes. and is still widely used in the form of eye drops and subconjunctival injections for the treatment of ophthalmoherpes and other viral eye diseases. Convincing clinical data have been obtained on the high effectiveness of poludan for the treatment of recurrent herpes affecting the skin and mucous membranes. If smooth skin is affected by recurrent herpes of the buttocks and thighs, the lesion is injected with poludan (200–400 mcg per lesion). Poludan has a general immunostimulating effect, which makes it possible to use it in secondary immunodeficiency conditions caused not only by herpesvirus infections.
IF inductors used per os
, which allows patients to independently carry out preventive and anti-relapse treatment courses recommended by the doctor.
Amiksin, alpizarin, flocazide, arbidol, being inducers of IF, stimulate the production of endogenous IF in the patient's body. This explains the positive therapeutic effect of the listed drugs in many viral diseases (recurrent herpes, influenza, adenovirus infection), which makes it possible to recommend them in the complex treatment of herpesvirus infections, especially in patients suffering from frequent colds and acute respiratory viral infections.
To stimulate the T- and B-links of cellular immunity in patients with recurrent herpes, the drugs taktivin, thymalin, thymogen, myelopid, etc. are successfully used. Treatment must be carried out under the control of an immunogram.
Specific immunotherapy
consists of using a domestic herpetic vaccine (polyvalent, tissue, killed). The therapeutic effect of the vaccine is associated with the stimulation of specific reactions of antiviral immunity, restoration of the functional activity of immunocompetent cells and specific desensitization of the body.
Comprehensive treatment of herpes simplex
Considering the peculiarities of the pathogenesis of herpes simplex, the most appropriate way to achieve a therapeutic effect is to use drugs with different mechanisms of action. Thus, the use of chemotherapy drugs with different mechanisms of antiviral action prevents the emergence of resistant strains of HSV; the use of interferons and their inducers in combination with a herpetic vaccine and immunomodulators makes it possible to comprehensively address the issues of herpes simplex therapy.
Treatment regimens for recurrent herpes can be different, which is determined by the clinical manifestations of HSV infection, the patient’s immune status and the doctor’s choice.
Treatment of recurrent herpes
The most pronounced therapeutic effect is achieved with an integrated approach to therapy
, which includes several stages:
1) antiviral therapy in combination with immunocorrection and interferon therapy, taking into account the data of an immunological examination and the study of interferon status;
2) anti-relapse treatment with a herpes vaccine in combination with immunomodulators and symptomatic use of antiviral drugs;
3) the use of adaptogens, repeated courses of vaccine therapy (re-vaccination), symptomatic use of antiviral drugs.
The duration of observation and the intensity of therapy for patients depend on the severity of herpetic infection, which is determined by the frequency of relapses, the presence or absence of a prodromal period, intoxication, pain, and the involvement of various systems and organs in the infectious process (Table 1).
The effectiveness of the therapy is assessed by reducing the duration and frequency of relapses, as well as the intensity of general symptoms of the disease.
The main remedy for stopping relapses
herpes simplex are ACV drugs (acyclovir, val acyclovir and famciclovir). There are two fundamentally different approaches to prescribing antiherpetic chemotherapy drugs:
a) episodic treatment - taking ACV drugs at the time of relapse, in therapeutic doses, observing the frequency and duration of drug administration.
b) suppressive therapy - long-term, long-term, constant use of ACV drugs without relapse in lower doses.
For episodic treatment during a relapse, patients are recommended to include the drug IF or an oral interferon inducer in the course of treatment in order to strengthen antiviral immunity and prevent possible complications of a viral infection (for example, Viferon and Arbidol).
Treatment of mild forms of RG
is often limited to prescribing ACV-drug in ointment and tablet forms and one or two courses of amixin or alpizarin, multivitamins during a relapse. Considering that the majority of patients with RG have impaired interferon status, it is advisable for them to prescribe an IF inducer or viferon, kipferon during a relapse.
If there is no effect from several repeated courses of nonspecific immunotherapy, vaccine therapy is indicated for patients with a mild form of herpes. The methods of choice are: repeated courses of immunoglobulin (2-3 per year), long-term (up to 1.5 months) administration of amixin or alpizarin in combination with antioxidants, course administration of dibazole with eleutherococcus, multivitamins, prodigiosan, etc.
In the course of treatment of patients suffering from moderate and severe forms
RG, it is necessary to include a herpes vaccine. It is advisable to combine vaccine therapy with immunomodulators (poludanum, myelopid), which increase its immunogenicity. In this case, the antiherpetic vaccine is prescribed after a course of immunomodulator.
Treatment of patients with frequent relapses
(moderate “b” and severe forms) begin with nonspecific immunotherapy, including immunoglobulin, stimulators of T- and B-cell immunity (under the control of an immunogram). Against the background of immunotherapy, patients note an improvement in general well-being, increased performance and a decrease in the frequency and severity of relapses. At the end of nonspecific immunotherapy, patients are prescribed a herpetic vaccine.
Patients with continuously recurring forms of herpes
Vaccination is indicated against the background of a 3-4 month course of suppressive therapy with ACV drugs.
Every 6–8 months, patients suffering from RH need to undergo revaccination. In the intervals between revaccinations, patients in these groups (according to indications) can be prescribed maintenance courses of nonspecific immunotherapy.
Features of local treatment for RG
The problem of local treatment of RH of the skin and mucous membranes was solved with the advent of acyclovir in the form of cream and ointment. With timely use of the drug (at the first signs of relapse or when prodromal local phenomena appear), the relapse is stopped in 1–2 days. Patients with intolerance to ACV or with low effectiveness are prescribed creams, ointments, gels, lotions, and sprays with other antiherpetic drugs.
External administration of antiviral drugs for herpes of the skin and mucous membranes is necessary to reduce clinical manifestations in the lesion, accelerate epithelization and reduce the duration of virus isolation from the lesion.
Without local treatment for herpetic lesions of the genitourinary system in men
It is almost impossible to achieve a significant therapeutic effect. To treat herpetic urethritis, you can use the liniment of cycloferon or poludan, which is injected into the urethra in the form of instillations. For herpetic proctitis, a pronounced therapeutic effect is observed when patients are prescribed Poludan solution in the form of microenemas, as well as with rectal administration of Kipferon suppositories.
Along with medicinal local treatment, men with chronic herpetic diseases of the pelvic organs undergo traditional local manipulations: bougienage of the urethra, massage of the prostate, followed by total instillation of Poludanum solution or Cycloferon liniment. To achieve a more pronounced anti-inflammatory, absorbable and analgesic effect, such patients should include low-frequency laser therapy in the course of treatment.
Local treatment of urethritis and proctitis in women
carried out in the same way as for men. For the treatment of herpetic cervicitis and colpitis, Kipferon suppositories (vaginally) and Cycloferon liniment are used.
However, even with such an integrated approach to the treatment of GC, there are cases with low therapeutic efficacy
, manifested:
1) torpidity to the therapy, when despite the ongoing antiviral and immunocorrective treatment (including vaccine therapy), the frequency and intensity of relapses of herpes in patients remains the same;
2) persistence of symptoms of persistent impairment of general well-being (weakness, malaise, psychoasthenia) and decreased ability to work against the background of a pronounced improvement in the clinical course of RG achieved as a result of treatment (reduction in the frequency and duration of relapses).
Virological examination of patients with low therapeutic efficacy often reveals an association of two herpes viruses: HSV and CMV
, which requires correction in the therapy.
Conclusion
Modern international standards for the management of patients with herpesvirus infections determine the following requirements for doctors:
1. The minimum standard for monitoring a patient is to establish an accurate diagnosis. To do this, it is necessary to examine the patient, take a smear from the site of skin or mucous membrane lesions and conduct a virological examination.
2. The patient should receive reasoned advice on a healthy lifestyle and recommendations on antiviral therapy. The doctor must be aware that the patient needs complete information about the disease.
3. As with other STDs, for genital herpes it is necessary to obtain biological materials for the diagnosis of other genital infections, and this should be discussed jointly between the doctor and the patient.
4. The doctor’s responsibility is:
- diagnosing a patient with clinical symptoms of herpes;
- familiarizing the patient, based on the diagnosis, with the prognosis of the disease, the risk of transmission of infection and the possibilities of antiherpetic treatment;
- involving the patient in deciding on the choice of method (episodic or preventive) and treatment program for recurrent forms of genital herpes.
| Historical reference . , symptomatic therapy occupied an important place in herpetic lesions of the skin and mucous membranes . Treatment consisted of local use of antiseptic drugs to help disinfect and limit the spread of foci of infection, reducing subjective sensations. During the 60-80s. In the 20th century, Soviet scientists created a number of antiviral drugs with different mechanisms of action, allowing for etiotropic therapy . The most numerous group of antiviral drugs includes nucleoside analogues, similar in structure to intermediate products of DNA and RNA biosynthesis. The mechanism of the antiviral action of purine and pyrimidine analogues is that they are included in the viral DNA molecule, replacing thymidine, and this leads to the formation of defective viral nucleic acid, devoid of infectious properties. A pronounced inhibitory effect against DNA-containing viruses, including HSV, is exerted by a group of chemical compounds - halogen derivatives of deoxyuridine: 5-bromo-2′-deoxyuridine (IDU), 5-bromouridine, 5-fluorouracil, cytosine arabinoside, adenine arabinoside (vidorabine , Ara-A). Ribavirin, which exhibits antiviral activity against 20 RNA and DNA viruses, was used for systemic therapy. Clinically, the most studied of these drugs are IDU and AZUR (6-azauridine). They have found application in ophthalmology, mainly for superficial forms of keratitis. However, drugs in this group do not have the ability to cross the blood-brain barrier, which did not allow their use in cases of HSV lesions of the central nervous system. For external use for herpetic lesions of the skin and mucous membranes, domestic scientists have created: oxolin, florenal, tebrofen, bonaftone, riodoxol, adimal, gossypol, megosin, etc. |
How to treat herpes in adults (medicines) –
Very often, patients ask questions about how to cure herpes forever. Unfortunately, at the moment medicine does not have the ability to achieve complete removal of the herpes virus from the body. However, modern antiviral agents (ointments and tablets) can effectively block the replication of the virus, especially when it comes to the herpes simplex virus (types HSV-1 and HSV-2). It can be much more difficult to cure herpes on the body, which is referred to as “shingles” or “herpes zoster”.
Modern antiviral tablets and ointments for herpes can significantly reduce the severity of herpes infection, speed up healing, and also reduce the frequency of relapses. There is also a domestic vaccine against the herpes simplex virus (types HSV-1 and HSV-2) called “Vitagerpavak”, which can reduce the frequency of repeated outbreaks of herpes infection by several times. Below we will tell you about the best remedy for herpes - both among means for external use and among tablet preparations.
But in order for herpes treatment to be as effective as possible, you must strictly follow the following rules:
- Herpes therapy will show good effectiveness if it is started no later than 12 hours from the moment the first herpetic rash appears. Keep in mind that the later treatment is started, the less effective even the best herpes medications will be.
- The maximum effectiveness will be shown by therapy that is started in the prodromal period (i.e., when the actual herpetic blisters have not yet appeared, but the patient already feels itching, burning or swelling of the tissue in this area). If treatment begins during this period, then the number and size of herpetic blisters formed in the future will be significantly smaller, and in this case, complete healing can be achieved in just 4-5 days.
- Remember that if you start treatment later than 48 hours , or after the herpetic blisters have opened, such therapy will not noticeably affect the speed of recovery (healing of lesions). However, in patients with severe and frequent relapses, such therapy can avoid complications.